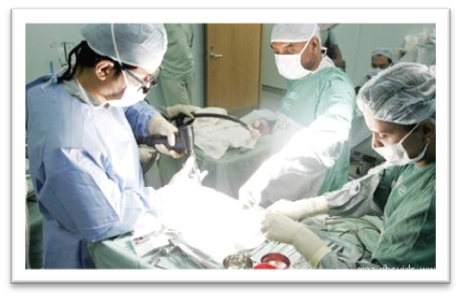
General patient coverage
- General patient coverage
Purpose:
To create a barrier against bacterial invasion of the wound.
Required Supplies:
- Required surgical drapes
- Additional drapes
- Towel clamp from the instrument tray
- Sterile wound cover, if needed
Procedure Steps:
1. Verify the surgical schedule to select the correct sterile drapes for the procedure.
2. Circulating nurse opens the drape pack, while the scrub nurse removes the required items following sterile technique.
3. Arrange the sterile drapes from the pack in the correct order of use.
4. The scrub nurse and the surgeon (or assistant) should drape the patient after skin preparation.
o Ideally, two sterile persons should perform the draping.
5. The scrub nurse hands the drape to the surgeon, ensuring proper coverage while avoiding leaning over the patient.
6. When unfolding the drapes, stand back from the operating table and spread the drape over a wide area.
7. Hold the drape at arm’s length and at a reasonable height to avoid contamination but not too high to touch the surgical light.
8. Do not shake the drape to unfold it.
9. Small drapes should be held at the corners for controlled opening.
10. Medium and large drapes or those for abdominal procedures should be unfolded as follows:
o Surgeon holds one end.
o Both surgeon and scrub nurse unfold and place it fully over the patient.
o Ensure it does not touch any unsterile surface before full placement.
11. Create a fold at the edge of the drape or wrap it around a gloved hand for controlled placement.
12. Perineal drapes should be placed using sterile forceps.
13. Before using a drape, check for moisture, tears, or damage:
o Discard if wet or torn.
o If already placed on the patient, cover with another sterile drape.
14. Drapes should remain dry throughout the procedure.
o If a drape becomes wet, cover it with a dry one.
15. Cover the operating table with two drape layers, including:
o Additional pieces
o Anesthesia armrests
o Anesthesia screen
16. Once placed, drapes should not be repositioned.
o If coverage is inadequate, add extra drapes.
17. If sterility is in doubt, replace or cover the drape immediately.
18. If using a split drape, it can be applied before or after general draping.
19. Use towel clamps to secure drapes at the incision site:
o If a split drape is used over cloth drapes, clamps may not be necessary.
o Ensure that only the drape fabric is clamped, not the patient’s skin.
o Avoid moving towel clamps after placement.
20. Drapes should extend at least 20 cm from the operating table sides.
o Ensure that the table legs, armrests, and anesthesia screen are fully covered.
21. If no anesthesia screen is available, use IV pole stands to hold the drape in place.
o Secure the barrier using towel clamps.
22. The instrument cleaning trolley should be removed from the OR, with staff wiping the wheels with disinfectant-soaked drapes before taking it to the dirty instrument storage area.
o The used drapes should also be taken to the dirty instrument storage area.
23. The operating room is ready for reuse once the floor is dry.
24. If no circulating nurse is available, the scrub nurse inside the OR should:
o Remove the mask and apron after cleaning.
o Change gloves before handling suction bottles and specimens outside the OR.
25. Once the scrub nurse exits the OR, they must not re-enter.
26. If the surgical field is contaminated, notify the head nurse, who will arrange for additional sterile equipment and disinfectants.