Topogaraphical, clinical and therapeutic ophthalmology
- EXAMINATION OF THE EYE
I- EXTERNAL EXAMINATION OF THE EYEBALL
1- Naked eye examination
Large animals are examined first out-of-doors in day light then indoors in a reduced light. Determine if the lesions are bilateral or unilateral and the normal eye is examined first. The following is determined
a. Lacrimation or abnormal discharge
b. Size of the eye
c. Position of the eye:
d. Endophthalmia
e. Exophthalmia
f. Strabismus
g. Periorbital swellings
2- MICROBIOLOGIC SAMPLING( Corneoconjunctival smears, scrapings and cultures)
- It is used to evaluate the condition of the cornea and conjunctiva for presence of a microbial pathogen by cytological assessment, culture, polymerase chain reaction, or immunofluorescent antibody labeling.
- Microbiologic specimens have been collected with a moist swab. May prefer to collect more cellular specimens from corneal or conjunctival lesions by scraping or with a cytology brush.

Fig.6: Instruments suitable for collecting ocular surface samples for cytologic and microbiologic examination. Left to right, Kimura platinum spatula, handle-end of Bard-Parker scalpel blade, cytology brush. (Bauer , et al.,1996).
3- Schirmer’s tear test(STT)
- It is a test used to measure the amount of tears produced per one minute.
- The test is performed with sterile, individually packaged strips of absorbent paper with a notch 5mm from one end. Each strip is folded at the notch and hooked over the middle to lateral third of the lower lid for 60 seconds.
- The STT measures basal and reflex tearing, including that due to corneal stimulation provided by the test strip itself, it can gently contact the corneal surface if it is placed more medially.
- Each animal had normal values of STT Readings of less. are considered diagnostic for keratoconjunctivitis sicca. particularly if appropriate clinical signs are present.
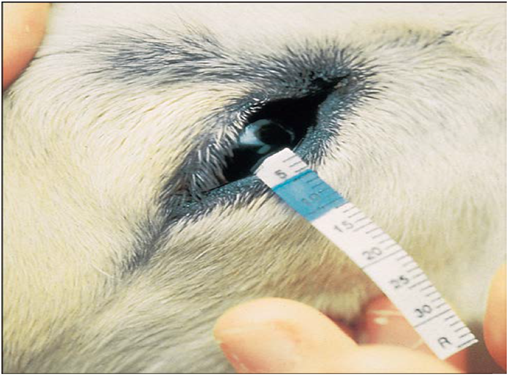
|
Fig.7: Schirmer tear test being performed on a horse. Note that the strip is placed into The lower lateral conjunctival fornix so that it lightly contacts the lateral cornea. (Abrams et al., 1990). |
II- Systemic examination
- The following structures are examined; eyelids (upper and lower), third eyelid, conjunctiva, sclera, cornea, anterior chamber, iris, lens, vitreous body and pupillary reflexes.
- A dark examination room for small animal and dark stall for large animal is suitable for detection of pupillary reflexes.
A- Pupillary reflexes (PLR) Direct pupillary reflex / Indirect pupillary reflex
- The reflex constriction of the pupil in response to light striking the retina is termed the pupillary light reflex. Its help to assess the pupil size, shape, and symmetry, pupil reactivity.
- Pupil shape and the speed and magnitude of the PLR differ among species.
- In most mammals, constriction of the pupil of the illuminated eye (the direct PLR) is slightly greater than that of the pupil of the contralateral or non-illuminated eye (the indirect or consensual PLR).
- If there is any pathology at any point along the neurologic pathway, iris atrophy (due to age), iris ischemia, (due to acute glaucoma), physical obstruction of the pupil (due to synechia or lens dislocation), prior use of a dilating drug, or high concentrations of circulating epinephrine (i.e., in fearful animals) the PLR may be decreased or absent.
- A positive direct pupillary light reflex is not a reliable indicator of vision or normal retinal function.
- Both the extent and speed of the PLR should be assessed and compared in the two eyes and against what is considered normal for that species.
1- Retroillumination
- Retroillumination is a simple but extremely useful technique for assessment of pupil size, shape, and symmetry. A focal light source (Fin off trans-illuminator or direct ophthalmoscope) is held up to the examiner’s eye and directed over the bridge of the patient’s nose from at least arm’s length from the patient so as to equally illuminate the two pupils and elicit the fundic reflection.
- This reflection is usually gold or green in tapetal animals and red in a tapetal individual.
- Retroillumination used to judge the clarity of all of the transparent ocular media (tear film, cornea, aqueous humor, lens, and vitreous).
- Retroillumination particularly useful for differentiating nuclear sclerosis from cataract.

Fig.8: Retroillumination used to judge the clarity of all of the transparent ocular media (David &Maggs,2022).
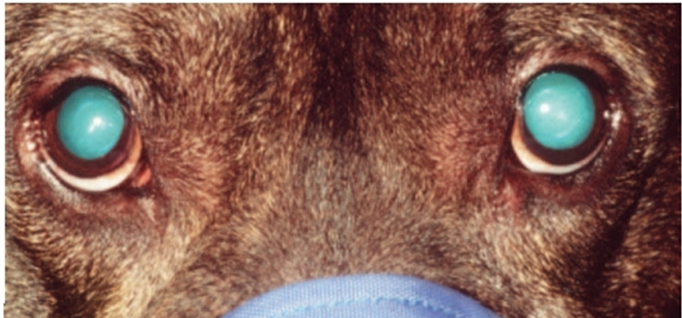
Fig.9: Retroilluminated view of a dog with bilateral nuclear sclerosis (Visible as a translucent ring inside the pupils of both eyes). (David &Maggs,2022).
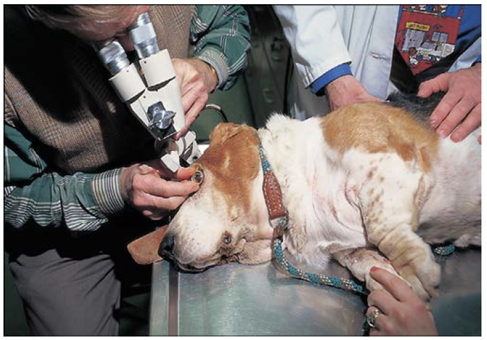
2- Slit – lamp bio-microscopy
- It is used for examination of the transparent structures of the eye (cornea and lens).
- it’s more sophisticated optical instrument that combines up to 40μ magnification and illumination and can be used to examine many different microscopic and optical features of the patient’s eye such as individual layers of the cornea that normally are invisible to the naked eye of the examiner. As such, it allows pathologic processes to be described more accurately so as to better guide diagnosis, prognosis, and treatment.
|
Fig.10: A slit-lamp bio-microscope in use. (Martin,1969).
Fig.11: portable slit lamp. |
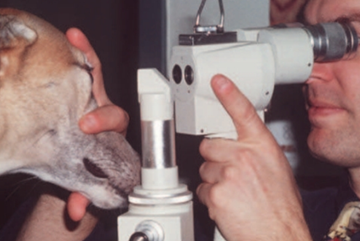
3- Gonioscopy
- It is a procedure used for examination of the anterior chamber angle on gonioscopic findings.
- Gonioscopy describes examination of the iridocorneal or “drainage” angle (the junction between the iris and cornea).
- In the normal eye of most species light rays that are reflected from the drainage angle strike the posterior cornea and undergo total internal reflection as in a prism.
- This occurs because of the difference in refractive index between the cornea and the surrounding air, and the high angle of incidence of the light rays from the drainage angle. By replacing the air surrounding the cornea with a goniolens that has an index of refraction close to that of the cornea, total internal reflection is avoided and light rays from the drainage angle can be viewed directly through the goniolens.
|
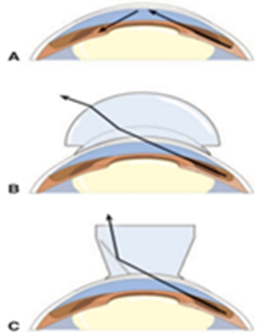
Fig.12:Performing gonioscopy in a non-sedated dog utilizing a slit lamp and a Franklin goniolens. (Bedford ,1973). Fig.13: Gonioscopy permits examination of the iridocorneal or “drainage” angle. A, Normally, light rays from the drainage angle undergo total internal reflection at the posterior cornea. B, A direct goniolens refracts light so that the drainage angle may be viewed directly. C, An indirect goniolens refracts light so that the image is viewed in a mirror. (Bedford ;1973). |
|
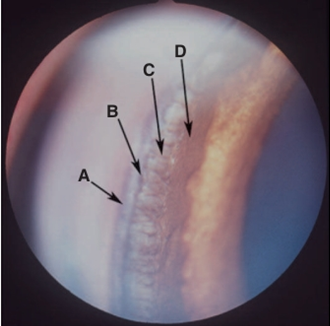
Fig.14: Gonioscopic view of a normal canine iridocorneal (drainage) angle. A, Outer pigment band; B, inner pigment band; C, pectinate ligaments; D, iris root (Martin,1969).
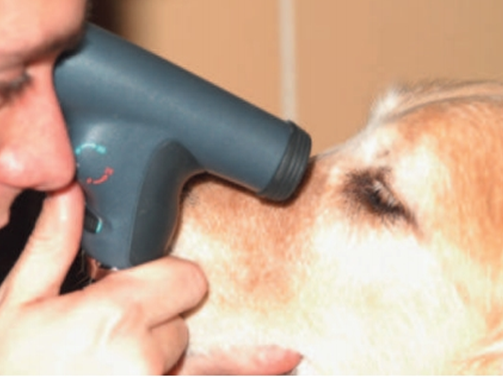
4- Tonometry
- It is the measurement of the intraocular pressure (IOP). It can be performed by three methods; digital tonometry, Schoitz tonometry and Applanation tonometry.
- normal canine and feline IOP is reported as approximately 10 to 20mmHg.
- It is a method of diagnosing anterior uveitis (where IOP is typically reduced) and of confirming the diagnosis of all other causes of reddened eye, such as keratitis, conjunctivitis, scleritis, and orbital cellulitis (in which IOP should be unaffected). Following confirmation of uveitis or glaucoma, tonometry should be an essential and perhaps the most important method of monitoring response to therapy and judging the augmentation of therapy.
- The IOP should be measured in all red, inflamed, or painful eyes to diagnose or eliminate from consideration both glaucoma and uveitis.
A- Indentation Tonometry
The Schiøtz tonometer relies upon indentation tonometry. In this method, a standard force is applied with a metal rod to the anesthetized cornea.
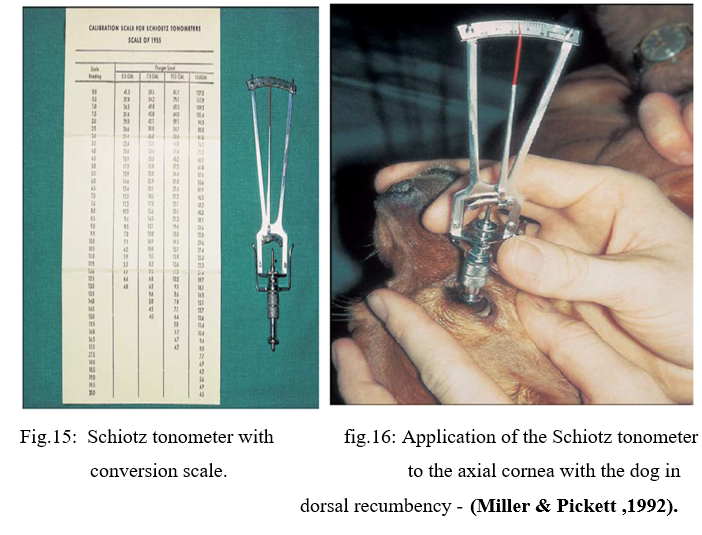
B- Applanation Tonometry
Unlike indentation tonometry, applanation tonometry using the Tono-Pen , is suitable for large animals, is unaffected by variations in ocular rigidity, requires no conversion tables, and needs no sterilization.
The advantages of the Tono-Pen include the following:
1- It is accurate and easy to use.
2- The animal’s head does not need to be held vertically, although the probe must a planate the corneal surface at right angles.
3- Errors induced by different sizes and curvatures of corneas in different species are less important.
4- Because of the small instrument head, irregular or diseased corneal areas may be avoided, and accurate readings obtained from even small corneas of exotic species.
5- The probe tip is covered with a disposable latex cap, which is changed between uses and prevents transfer of infections.
6- Minimal restraint is required.
7- The pressure is displayed in mm Hg without need for conversion via tables.
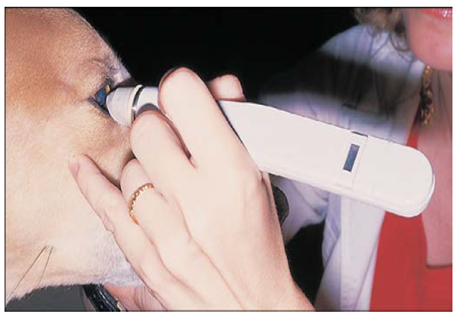
Fig.17: Tono-Pen in use by lightly tapping the cornea. (Leiva, et al.,2006).
C- Rebound Tonometry
Rebound (or impact or dynamic) tonometry is a third mechanism by which IOP may be measured and which uses a different mechanical principle. Rebound tonometer eject a small probe (such as a metal pin with a rounded end) at a fixed distance from the cornea and assess the motion of the probe as it strikes the cornea and is returned (rebounds) to the instrument.
|
Fig.18: Rebound tonometry using the TonoVet in a dog ( Görig et al. ,2006). |
. |
|
1-Ophthalmoscopy
- It is the study of the internal structures of the eyeball by ophthalmoscope directly through a widely dilated pupil by aligning the light beam with his/her visual axis and standing a short distance from the patient, as for retro-illumination .
a- Direct ophthalmoscopy
The direct ophthalmoscope directs a beam of light into the patient’s eye and places the observer’s eye in the correct position to view the reflected beam and details of the interior of the eye.

Fig.19: The direct ophthalmoscope. Controls for light intensity (A),
focusing lenses (B), light aperture size and shape (C), and filters (D).
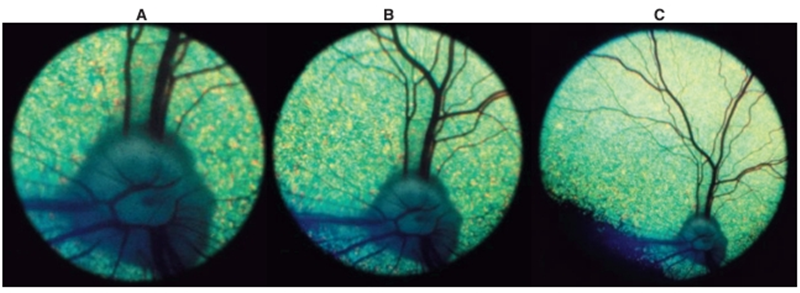
Fig.20: View of a canine fundus as seen through the direct ophthalmoscope (A), the monocular indirect (Panoptic) ophthalmoscope (B), and a 20-D indirect lens (C). Note that as magnification increases, field of view decreases. ( Ramsey et al.,1999).
b- Indirect ophthalmoscopy
Viewing the image of the fundus with a convex lens (typically 20 to 30 D) is placed between the observer’s eye and the patient’s eye and an inverted virtual image is formed between the lens and observer. The magnification and field of view depend on the dioptric power of the lens and on the size of the patient’s eye. However, with the lenses typically used in veterinary medicine, the magnification is always less and the field of view greater than that achieved with use of a direct ophthalmoscope.
|
Fig. 21: The monocular indirect ophthalmoscope (Panoptic) in use. (Moore , 2001) |
Fig.22: Binocular indirect ophthalmoscope. This unit has a rechargeable battery transformer that allows portability.
|
2- Electroretinography (ERG):
- Electroretinography (ERG) is the study of electrical potentials produced by the retina when light strikes it. Light of varying intensity, wavelength, and flash duration is directed onto the retina and the resulting potential differences are detected by electrodes placed around the eye.
- The ERG is performed with the animal under general anesthesia or deep sedation to minimize periocular muscle movements. It is useful in all species. Electroretinography is a test of retinal but not optic nerve or visual function. It is usually available only at specialty ophthalmology practices.
The ERG may be used for the following purposes
1- Preoperative evaluation of retinal function before cataract extraction when fundic examination is not possible.
2- Diagnosis and differentiation of inherited retinal disorders (e.g., rod-cone dysplasias, progressive retinal degeneration, hemeralopia)
3- Investigation of unexplained visual loss (amaurosis) in which retinal lesions are not visible ophthalmoscopically (e.g., sudden acquired retinal degeneration SARD, optic neuritis, CNS disease).

Fig.23: An electroretinogram being performed on a dog. Note the ground and reference (subcutaneous) electrodes as well as the corneal contact lens electrode. (Acland ,1988).
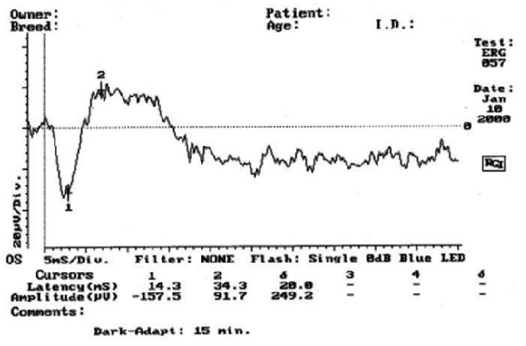
Fig.24: A normal electroretinogram (Acland GM ,1988).
3-Ultrasonography
- In ultrasonography, high-frequency sound waves above the audible range are directed posteriorly through the eye from the cornea, and the echoes are detected.
- Ultrasonography is used to examine the contents of eyes in which opacity of one of the usually clear ocular media (cornea, aqueous humor, lens,or vitreous) prevents visualization of the structures caudal to it. It is also useful to assess orbital structures and to guide fine needle aspiration of intraocular and orbital structures.
Ultrasonography is particularly useful for the following
- Detection of retinal detachment.
- Detection of lens dislocation or rupture.
- Detection of vitreous degeneration
- Detection of intraocular tumors or foreign bodies
- Characterization of retrobulbar disease
- Guidance of fine-needle aspirates of orbital and ocular lesions.
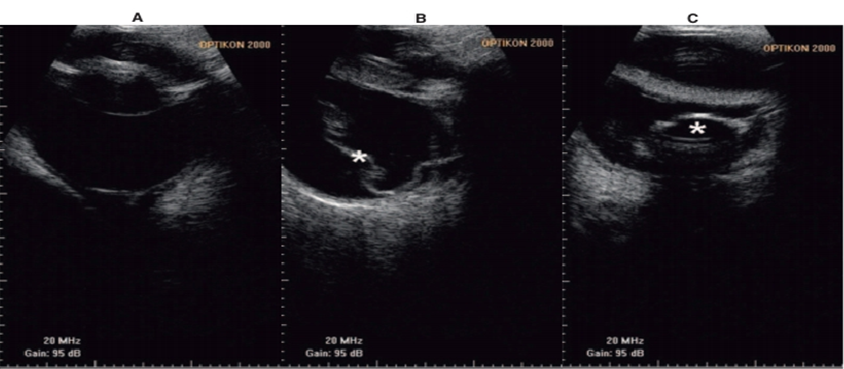
Fig.25: B-mode ultrasound images of A, a normal globe; B, a detached retina (*); C, a posteriorly luxated lens (Cottrill et al., 1989).
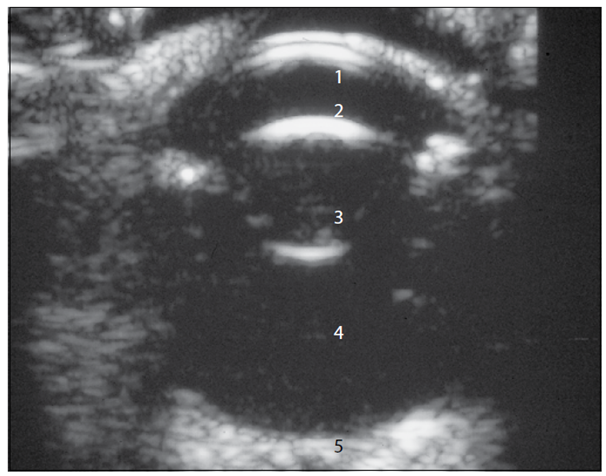
|
Fig.26: B-mode ultrasound image of a normal 11-year-old dog with a 10-MHz probe and direct contact with the cornea. (1: Cornea; 2: Anterior chamber; 3: Lens; 4: Vitreous; 5: Optic nerve (Cottrill et al., 1989). |
5- Anterior chamber paracentesis
- It is the collection of a sample of aqueous humour. The anterior chamber is entered at the limbus and is indicated in cases of hypopyon, chronic uveitis, malignant glaucoma, prior to surgery and diagnosis of anterior segment diseases.
- A 30-gauge needle has been inserted at the dorsolateral limbus and directed in a plane parallel to the iris. No syringe is attached, and aqueous humor is allowed to passively fill the needle hub. In this procedure, care should be taken not to touch the corneal endothelium, the iris, or the lens with the needle tip.
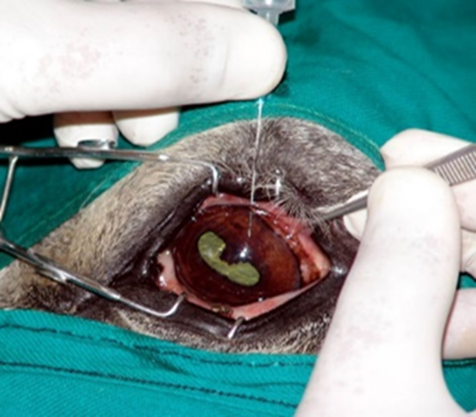
Fig.27: Anterior chamber paracentesis from a cat with uveitis. (Hamor ,2001)
6- Vitreous paracentesis
Vitreous paracentesis (hyalocentesis) in dogs is a procedure to collect small amount of vitreous fluid for diagnostic analysis, performed under general anesthesia after dilating the pupil and disinfecting the eye. The needle is carefully inserted through the sclera and pars plana ciliaris to avoid complications like retinal punctures or significant intraocular hemorrhage.
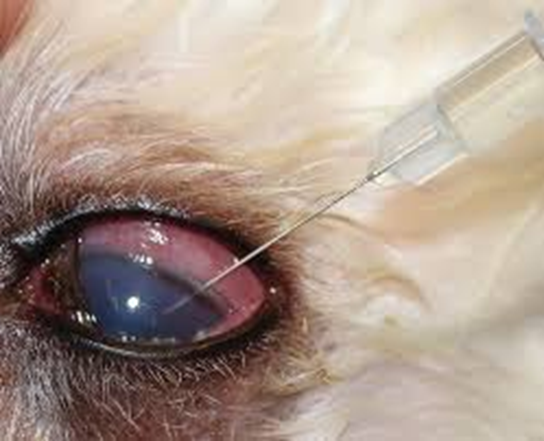
Fig.28: Vitreous centesis of a cat eye. Special care should be taken to avoid the lens (Hamor,2001)
6- Computed Tomography and Magnetic Resonance Imaging
- CT and MRI provide superb detail for localization of orbital lesions.
- Contrast sialography and dacryocystorhinography are as applicable to CT as they are to radiography and provide superior detail.
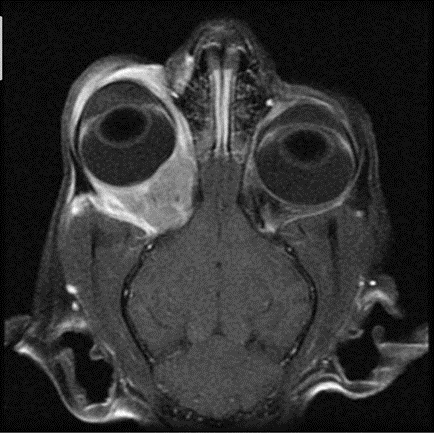
Fig.39: T1-weighted, post–contrast injection, frontal magnetic resonance image of a cat with a space-occupying mass behind the right eye. Cytology and culture testing performed on material aspirated from this mass permitted diagnosis of a bacterial retrobulbar abscess/cellulitis that responded well to antibiotic therapy (Calia et al., 1994).