Equipment used in the reception and emergency department
| Site: | EHC | Egyptian Health Council |
| Course: | Nursing Procedure Guidelines for the Reception and Emergency Department |
| Book: | Equipment used in the reception and emergency department |
| Printed by: | Guest user |
| Date: | Tuesday, 5 May 2026, 11:38 PM |
Description
"last update: 16 March 2025" تحميل الدليل
- Prepared by
Emergency guide
Under supervision
- Prof. Dr. Mohamed Latif, CEO of the Egyptian Health Council
Dr. Kawthar Mahmoud, Head of the Egyptian Nursing Syndicate - Member of the Senate
Supervised by
Dr. sherif wadie, advisor to the minster of health for emergency and urgent care
Prepared by
|
Title |
Name |
NO. |
|
Dean Of Faculty Nursing, Professor of Medical and Surgical Nursing, Tanta University |
Dr Afaf Abdel Aziz Abdel Aziz Basal |
1 |
|
Professor Of Critical Care Nursing |
Prof.Dr/Zeinab Hussain Ali |
2 |
|
Professor And Head of the Department of Medical Surgical Nursing. Faculty-. Benha University |
Prof.Dr Amal Said Taha Refaie |
3 |
|
Supervisor Of the Education Sector at Port Said University |
Prof.Dr Amal Ahmed Khalil Morsy |
4 |
|
Professor Of Medical Surgical Nursing- Faculty of Nursing- Cairo University |
Dr. Hanan Ahmed Al Sebaee |
5 |
|
Head of central administration on secondment at MOHP |
Dr Neveen ab drab al0nabi Mohamed |
6 |
|
Director Of Primary Health Care Nursing Department at MOHP. |
Maysa Hosny Ahmed Tammam |
7 |
|
Supervisor Of Technical Education- EHA |
Nancy Alaa Eldeen Abd-Elbaset Ali |
8 |
|
Supervisor Of Nursing Services Development- EHA |
Sherien Mohamed Saad |
9 |
|
Assistant Professor of Maternity and Neonatal Health Nursing - Faculty of Nursing- Ain Shams University |
Assist.Perof. Dr./Heba Mahmoud Mohammed |
10 |
|
General manager of general administration of health institutes affairs |
Dr Mai Galal Ibrahim Al-Assal |
11 |
|
Participants |
||
|
Director Of Curative Nursing Department MOHP |
Dr. Azza Galal Ahmed Khalil |
12 |
|
Member of the Nursing administration, EHA, Luxor Branch |
Mr. Ahmed Mohamed Ahmed Al Noubi
|
13 |
|
Nursing Specialist at the General Administration of Nursing - Ministry of Health |
MS. Angham Hamdy Abdel Khaleq
|
14 |
|
Nursing Specialist at the General Administration of Nursing - Ministry of Health |
Mr. Ahmed Muhammad Hussein Mubariz |
15 |
|
Nursing Specialist at the General Administration of Nursing - Ministry of Health |
Mr. Abdel-Azim Al-Saeed Abdel-Azim Al-Hanafi |
16 |
|
Nursing Specialist at the General Administration of Nursing - Ministry of Health |
Mr. Shawkat Yusre Hussein
|
17 |
|
nursing specialist at the General Administration of Nursing |
Mr. Karim Ahmed Sadik |
18 |
- The policy for using the monitor
| Policy no. | Managing Patients with Angina | Policy name | ||
| No. of pages |
| Review Date: |
| Issue Date and Number: |
| section | ||||
Purpose:
1. Measurement of vital signs
2. Electrocardiogram (ECG)
3. Measurement of blood pressure using a cuff around the patient's arm. Normal blood pressure is 120/80 ± 20/15
4. Measurement of body temperature using thermometers. Normal temperature is from 36.5°C to 37.5°C
5. Measurement of blood oxygen levels
Work procedures:
· Connecting the electrodes and sensors:
- Connect the ECG electrodes to the patient’s chest to monitor heart activity.
- Place the pulse oximeter on the patient’s finger to measure blood oxygen levels.
- Use the NIBP device to measure blood pressure periodically.
- If necessary, connect additional sensors like the respiratory rate monitor or central venous pressure catheter.
· Turning on the monitor:
- Turn on the device after connecting all electrodes and sensors.
- Ensure the device recognizes all connected sensors and displays the readings correctly.
· Reading the data:
- The monitor displays a range of data such as:
- Heart rate (HR): Displayed in beats per minute.
- Oxygen saturation (SpO2): Displayed as a percentage.
- Blood pressure (BP): Typically displayed as two numbers, systolic and diastolic.
- Respiratory rate (RR): Displayed as breaths per minute.
- ECG: Displays the electrical activity of the heart.
- Ensure you understand each of these readings and their significance for the patient’s condition.
· Setting the alarms:
- The device can be set to trigger an alarm if readings go beyond normal limits. Make sure to adjust the thresholds according to the patient's medical condition.
· Continuous monitoring:
- Continuously monitor the device to ensure readings stay within safe limits.
- If the monitor shows sudden changes or abnormal readings, take immediate action according to medical procedures.
· Recording the data:
- You may need to record the data displayed on the monitor periodically to track the patient’s condition or for review by the physician. If working in intensive care, it’s important to receive comprehensive training on using the monitor and understanding how to respond to changes in the readings.
Definition:
The medical monitor is an electronic medical device used for medical observation, continuously displaying physiological data on its screen.
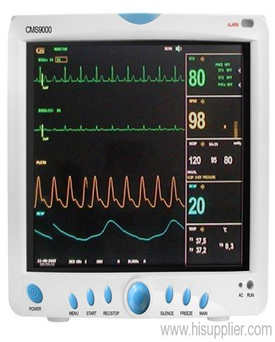

types:
1- Analog monitoring devices:
They were used in the past, where the device only displayed the heart's rhythm. After making specialized modifications, there was a monitor that measured blood pressure and another to measure the pulse. These devices were widely used and helped save many lives, but there were several obstacles in their way, such as electrical interference, the lack of alarms, and their high cost.
2- Digital Monitoring Devices:
With the presence of digital signal processing technology, medical monitors have developed significantly. All models have become digital, with the advantages of miniaturization and portability. Their measurements now include pulse rate, blood oxygen level, blood pressure, temperature, and electrocardiogram.
3- Monitors attached to a pacemaker.
These devices are often used in the emergency and reception unit to save time and effort in transferring the patient from one device to another..
1. The individuals who use these devices the most:
· Patients in critical care units.
· Patients in dialysis units.
· Patients in operating rooms.
· Patients in recovery rooms.
· Patients in emergency units until they are classified.
· Pediatric patients in neonatal intensive care units.
- The policy for Using the Electric Syringe
| Policy no. | Managing Patients with Angina | Policy name | ||
| No. of pages |
| Review Date: |
| Issue Date and Number: |
| section | ||||
Purpose:
The electric syringe (or electric injector) is primarily used to deliver fluids or medications into the patient's body in a precise and controlled manner. It is used in many medical applications, such as administering intravenous medications, insulin infusion, and intravenous feeding.
Work procedures:
Using the electric syringe (or intravenous pump) for medication administration requires careful steps to ensure safety and effectiveness:
- Prepare the equipment:
- Ensure the electric syringe is functioning properly and programmed for use.
- Prepare the medication to be administered according to the doctor's instructions, confirming the correct dose.
- Prepare the syringe: Fill the syringe with the medication, ensuring that any air bubbles are removed.
- Connect the syringe securely to the electric syringe device.
- Programming the electric syringe:
- Enter the required information into the device, such as flow rate and total dose to be administered.
- Verify the accuracy of the entered information by reviewing it again.
- Connecting to the patient:
- Connect the electric syringe to the patient’s intravenous (IV) line, ensuring that the line is functioning properly.
- Confirm that the connection is secure and there is no leakage.
- Monitoring the process:
- Start the electric syringe and closely monitor the medication flow.
- Periodically check that the syringe is functioning properly and that the dose is being administered as programmed.
- Observe the patient's condition for any abnormal signs or reactions to the medication.
- Stopping the syringe:
- Once the dose has been completed, stop the electric syringe.
- Remove the syringe from the device and dispose of it according to medical protocols.
- Follow-up on the patient:
- Monitor the patient’s response to the medication after administration.
- Record all details of the process in the patient's medical record.
Following these steps ensures the medication is administered safely and effectively.
- Policy for Dealing with a Patient on a Ventilator
| Policy no. | Managing Patients with Angina | Policy name | ||
| No. of pages |
| Review Date: |
| Issue Date and Number: |
| section | ||||
Policy:
Mechanical Ventilation: It is a method of breathing or assisting the breathing process using a mechanical device. It is used when a patient is unable to breathe sufficiently for adequate gas exchange to meet the body's and tissues' needs, or when the patient is completely unable to breathe. This can occur due to several reasons, such as respiratory failure or other conditions that require respiratory support to maintain oxygen levels in the blood and remove carbon dioxide.
Indications for placing a patient on a mechanical ventilator:
The Indication | The Abnormal Rate | Normal rate |
Respiratory Rate
| Greater than 35 breaths per minute | 10-20 breaths per minute
|
Tidal volume in one breath | Less than 5 mL/kg of body weight | 5-7 mL/kg of body weight |
Maximum inspiratory force
| Less than 25 cm of water
| 75–100 cm of water
|
Oxygen level in blood gas analysis
| Less than 60 mmHg when the patient is on 60% oxygen.
| 75–100 mmHg on air
|
Carbon dioxide level
| Greater than 60 mmHg
| 35–40 mmHg
|
With the presence of some indicators (cyanosis, excessive sweating, confusion, shallow and rapid breathing), it should be evaluated by a doctor.
Different methods of using a ventilator:
1- Continuous Mandatory Ventilation (CMV):
Through this method, the ventilator delivers a set number of breaths and a specific volume of air as determined by the doctor. In this case, the patient does not take any breaths on their own and relies entirely on the ventilator.
Uses of this method:
➡️ It is used for patients with head injuries, as involuntary breathing may lead to increased intracranial pressure.
➡️ During surgical procedures, to administer anesthetic drugs that relax the muscles.
➡️ In cases where anesthetic drugs or muscle relaxants are used, especially when the patient is placed on a ventilator.
2- Synchronized Intermittent Mandatory Ventilation (SIMV):
This method provides the patient with a set number of breaths and a specified volume of air, but the ventilator also allows the patient the opportunity to take breaths on their own.
Uses of this method:
- It is used as a method to begin weaning the patient off the ventilator.
- It is used in cases where the patient is able to start breathing on their own.
3- Continuous Positive Airway Pressure (CPAP):
This method involves supplying the patient with air at a specific pressure during the breathing process, allowing some air to remain in the alveoli of the lungs. This helps with gas exchange and improves lung efficiency.
Uses of this method:
- It is used as a method to wean the patient off the ventilator.
- It is used for patients who are able to breathe voluntarily but need assistance by being supplied with compressed air.
steps:
The nursing team must observe the following:
- Monitor the patient's vital signs and observe the monitor for any changes in heart rate.
- Observe the patient's color for any cyanosis or color changes, and check the amount of air entering the patient's chest using a stethoscope.
- The respiratory rate should be 10–12 breaths per minute.
- Any increase in airway pressure indicates a problem, such as the accumulation of secretions in the patient's chest.
- The patient's alertness on the ventilator or the presence of ventilator tube pressure.
- Ensure that the movement of the patient's chest is even on both sides to guarantee fair distribution of air in both lungs, as the endotracheal tube might enter one lung more than the other.
- The patient should be at a temperature of 34°C.
- Suctioning the endotracheal tube.
- Care for the tracheostomy tube.
- Regular exercises and maintaining the patient's cleanliness.
- Ongoing care and maintaining the patient's hygiene.
In the case of weaning the patient off the ventilator:
- Explain the steps to the patient to reduce fear and anxiety.
- Wear latex gloves.
- Position the patient in a sitting position (according to their health condition).
- Suction the endotracheal tube.
- Deflate the tracheostomy balloon.
- Encourage the patient to take some breaths.
- Remove the tube.
- Place the patient on an oxygen mask (O2) or according to the doctor's instructions using a T-Tube or Ventorey mask depending on the required concentration.
- Monitor changes in the patient's breathing.
- Encourage the patient to cough and clear phlegm.
- Perform a blood gas analysis for monitoring.
- Prepare a ventilator near the patient, ready for use, along with an endotracheal tube in case the patient needs to be reconnected to the ventilator.
- Policy for dealing with patients with defibrillators
| Policy no. | Managing Patients with Angina | Policy name | ||
| No. of pages |
| Review Date: |
| Issue Date and Number: |
| section | ||||
The policy:
Training nursing staff on the use of the defibrillator, which is a key element in cardiopulmonary resuscitation (CPR) in emergency departments.
The tools used:
- Gel
- Emergency cart, always equipped and ready for use
- Anesthetic, as per the doctor's instructions
steps:
Ensure all tools are prepared and verify the charge of the defibrillator.
In case of cardiac arrest:
- Ensure the environment is safe for all surrounding individuals and the patient (no water present, and avoid contact with the bed while discharging the shock).
- Apply gel to the patient's chest in the area where the shock will be discharged to prevent burns.
- Follow the doctor's instructions regarding the discharge of the shock, confirming loudly that it will begin, and monitor the monitor for any changes.
Conscious patient:
- Admit the patient to the emergency department and reassure them.
- Connect the patient to the monitor and measure vital signs regularly to track their condition moment by moment, while also monitoring the patient's level of consciousness.
- Follow the doctor's instructions regarding charging the device as per their guidance.
- Administer oxygen to the patient as per the doctor's instructions after delivering the shock.
- Observe the level of consciousness after delivering the shock.
- Perform an electrocardiogram (ECG) for the patient after the shock.