Veterinary Anesthesia
| Site: | EHC | Egyptian Health Council |
| Course: | General Veterinary Surgery Guidelines |
| Book: | Veterinary Anesthesia |
| Printed by: | Guest user |
| Date: | Wednesday, 6 May 2026, 12:53 AM |
Description
"last update: 26 January 2025" Download Guideline
Table of contents
- - Acknowledgement
- - Abbreviations
- - Glossary
- - Scope
- - VETERINARY ANESTHESIOLOGY
- - Local Anaesthesia by surface application (Topical)
- - REGIONAL ANAESTHESIA
- - Classification of epidural anaesthesia
- - Epidural
- - Intravenous Regional Anaesthesia
- - Lower limb regional anesthesia for declaw
- - PREANAESTHETIC MEDICATIONS
- - Classification
- - Tranquillizers (Atractic or neuroleptic drugs)
- - Narcosis
- - Muscle relaxants
- - GENERAL ANAESTHESIA
- - Cardiac arrest and Resuscitation
- -References
- Acknowledgement
We would like to acknowledge the committee of National Egyptian Guidelines for Veterinary Medical Interventions, Egyptian Health Council for adapting this guideline.
Executive Chief of the Egyptian Health Council: Prof. Mohamed Mustafa Lotief.
Head of the Committee: Prof. Ahmed M Byomi
The rapporteur of the Committee: Prof. Mohamed Mohamedy Ghanem.
Scientific Group Members: Prof. Nabil Yassien, Prof. Ashraf Shamaa, Prof. Amany Abbass, Prof. Dalia Mansour, Dr Essam Sobhy, Dr. Mohamed Elsharkawy, Prof. Gamal Sosa. Dr. Naglaa Radwan, Dr. Hend El Sheikh
Scientific Editor: Prof. Ashraf Aly Eldesoky Shamaa Prof. Mohamed Mostafa Saied Amer, Prof. Shaaban Mohamed and Dr. Mohamed Mostafa Bahr Mostafa,
- Abbreviations
mg Milligram Kg kilogram mL milliliter
IM intramuscular IV intravenous S/c subcutaneous
hrs Hours ug microgram Br Breathing Rate
HR Hart Rate Dy day Sec second
APR Abdominoperineal resection ETV Endoscopic third ventriculostomy
IPPV Intermittent positive-pressure ventilation OD Overdose
- Glossary
· Sepsis means presence of the pathogenic microorganism in the living tissue or in the body fluid
· Contamination the presence of microorganisms on the living tissues, materials and equipment
· Infections the growth of microorganism on, and their invasion of living tissues
· Sterilization means complete elimination of all microorganisms (including both vegetative and spore forming) by using physical and chemical methods of sterilization.
· Asepsis is the state of being free from disease pathogenic microorganisms in the living tissue or in the body fluid (such as bacteria, viruses, fungi, parasites).
· Antisepsis is the methods to combat pathogenic microorganisms or inhibit their growth by antiseptics and disinfectants.
· Contamination is the presence of microorganisms on the living tissue, materials and equipments.
· Infection is the growth of microorganism on and their invasion of living tissues.
- Scope
This guideline outlines the basics of general surgery, suture materials and techniques. In order to perform surgery in animals, it is important to know and understand the different techniques of anesthesia and correctly diagnose, construct surgical plan and follow up treatment using diagnostic imaging. So, complete understanding the different anesthetic drugs and techniques as well as the different methods of diagnostic imaging for all animal species is essential and must be achieved.Also know and understand the surgical problems of the different body systems including digestive, respiratory, cardiovascular, urogenital and abdominal wall. Moreover, to accustom students how to pick the principles up, to recognize case appraisal, etiology, clinical signs, diagnosis and differential diagnosis, prognosis and different traits used of treatment.understand and diagnose lameness in different animal species. Moreover, to accustom students how to pick the principles up, to recognize case appraisal, etiology, clinical signs, diagnosis and differential diagnosis, prognosis and different traits of eye, ear as well as back diseases
- VETERINARY ANESTHESIOLOGY
– Definition:
Anaesthesia means insensibility. It is the name given to the whole art and science relating to the production of insensibility.
It is a reversible process to produce a convenient, safe, effective, yet inexpensive means of chemical restraint so that medical or surgical procedures may be expedited with minimal stress, pain, discomfort, and toxic side effects to the patient or to the anaesthetist.
- Criteria for selection of drugs and techniques of anaesthesia
The choice of the anaesthetic agent or technique depends on several variables:
1) Facilities and anaesthetic equipment available.
2) Personal knowledge and experience.
3) Safety of the anaesthetic agents and cost.
4) The species of animal involved:
a- Size of the animal
b- Demeanor (Temperament).
c- Anatomical and physiological peculiarities.
5) Nature of the operation to be performed:
Magnitude, site and duration of the operation.
6) Physical status of the animal.
Peripheral Anaesthesia
Local and Regional Anaesthesia
Local anesthesia
Local anaesthetics / analgesics
Loss of sensation in a defined body area without loss of consciousness.
These are substances having selective and transient paralytic action on the sensory nerves and nerve endings and are used for inducing both local and regional anaesthesia.
Vasoconstrictor + local anaesthetic
|
Potency ratio |
Uses |
Trade name |
Anaesthetic agent |
|
1:1 |
1-4% |
Novacaine |
1- Procaine Hcl |
|
5:1 |
1-2% |
Pantocaine |
2- Amethocaine Hcl |
|
2:1 |
1-2% 2-4% topically |
Xylocaine |
3- Lignocaine Hcl (Lidocaine) |
|
2.5:1 |
Carbocaine |
4- Mepivacaine |
|
|
8:1 |
0.5-1.0% |
Marcaine |
5- Bupivacaine |
|
20.0 |
0.5% |
Nupercaine |
6- Dibucaine |
· increase duration almost 5 times.
Hyaluronidase + local anaesthetic
· doubles the anaesthetized area.
· Potentiation of local anaesthetics:
Toxic effect of local anaesthetics:
· Drowsiness, twitching and convulsions.
· Respiratory depression, bradycardia and hypotension.
- Local Anaesthesia by surface application (Topical)
1- Intended line infiltration
2- Field block
Onset Duration
Lidocaine 10-15 min 1-2 h
Mepivacaine 5-10 min 2-2.5 h
Bupivacaine 15-20 min 2.5-6 h
Ropivacaine 5-15 min 2.5-4 h
Local anesthetic – how do they work?
- Diffusion into the nerve
- Sodium channel blockers
- Lipid solubility – potency
- Concentration – onset time and block intensity
- Protein Binding – duration of action
Adverse effects
- Local site reaction
- Central nervous system
- Cardiovascular system
- Nerve injury
– Needle induced
– Drug induced
- Allergic reaction – methylparaben
- Methemoglobinemia
The principal advantages of field block are:
a- Absence of distortion of the anatomical features in the line of incision.
b- Ischemia of the tissues within the blocked area if a vasoconstrictor is incorporated in the solution of local analgesic.
c- Muscle relaxation.
d- Absence of interference with the healing of the wound which often claimed to be the chief objection to direct local infiltration analgesia.
Topical application
- Ophthalmic – proparacaine
- Laryngeal – lidocaine
- Topical – prilocaine + lidocaine
CNS Toxicity
- Large blood vessels (epidural)
- CNS toxicity symptoms usually occur before cardiovascular toxicity
- Seizure activity - diazepam + oxygen
Toxic dosage
- Lidocaine 10 to 20 mg/kg
- Bupivacaine 2 to 3 mg/kg
- USE ½ OR LESS THAN TOXIC DOSAGE -
- Cats are more sensitive than dogs
- Birds are more sensitive than cats
- REGIONAL ANAESTHESIA
It is loss of sensation in a region of the body. It is affected by blocking the conduction in the sensory nerve or nerves innervating the region where an operation is to be performed
Perineural injections commonly used in veterinary practice including :
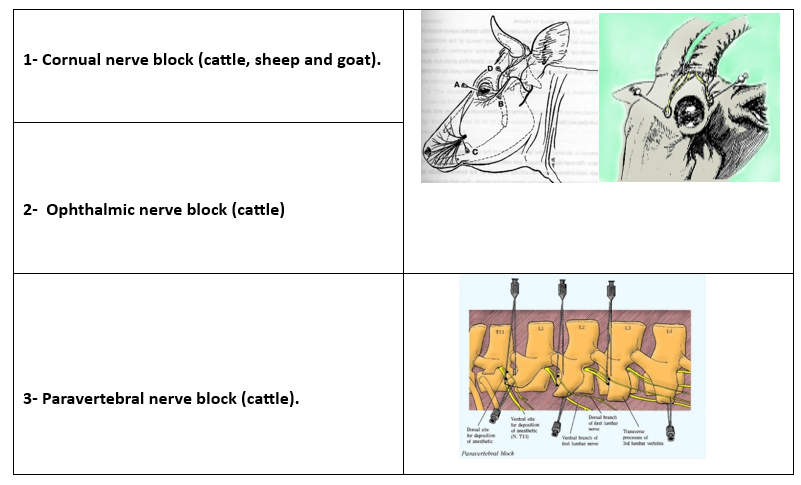
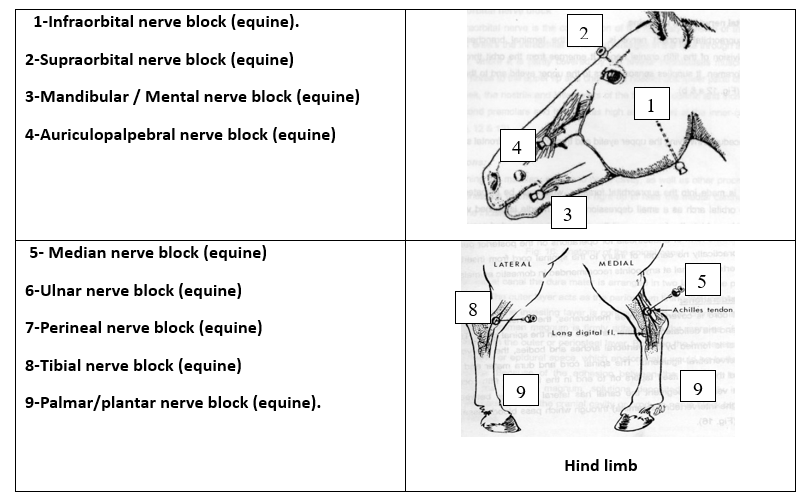
Equine - Limb regional anesthesia
- Epidural
- Brachial Plexus Block
- Ring block
- Paw block
- Classification of epidural anaesthesia
1) According to the site of injection:
a- Lumbar epidural anaesthesia: Injection is made in lumbo-sacral space and is indicated for small animals.
b- Caudal epidural anaesthesia: It is indicated for large animals and the injection is made either in the sacrococcygeal space such in buffaloes (with perpendicular angle), or in the first intercoccygeal space such as in cattle (perpendicular angle), camel (perpendicular angle) (perpendicular angle), horses (with angle 60 °), and donkeys (with angle 30 °) .
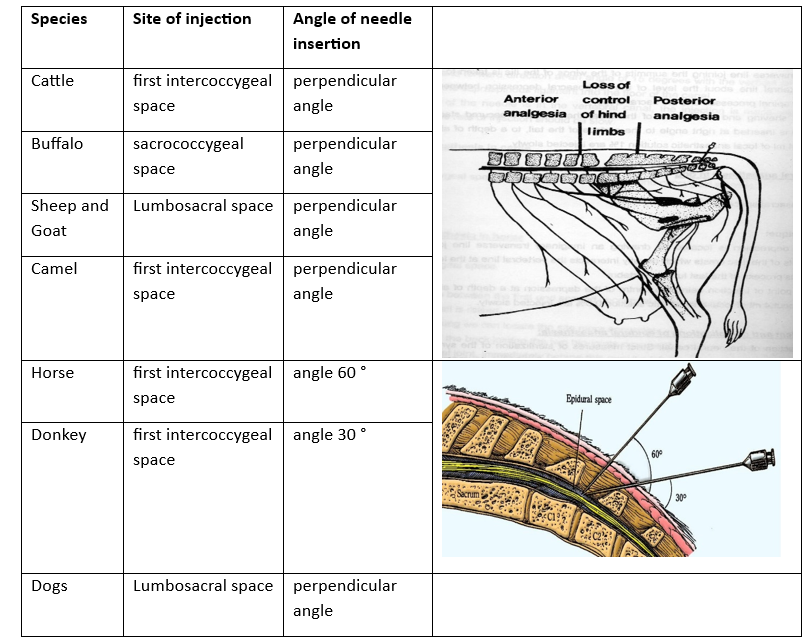
2) According to the distance forwards the anaesthetic solution spreads in the spinal canal, and thus the extent of the area in which the sensory and motor paralysis subsequently develop, into:
a- Posterior type:
b- Anterior type
Use epidural for:
▪️ Caudal surgery
– Tail amputation
– Perianal surgery
– Rear limb surgeries
▪️ Abdominal surgery
– Cesarian section
▪️ Urogenital surgery
▪️ Thoracic surgery (neuraxial analgesia)
Do not use epidural if:
▪️ Absolute
– Systemic or local infection
– Blood withdraw
– Allergies (local anesthetics or opioids) .
– Coagulopathies
▪️ Relative
– Hemodynamically unstable
– Pelvic fracture
Confirmation of succus injection
▪️ Loss of resistance
– Air or saline
– Hanging drop
– Bubble compression
▪️ Nerve irritation
▪️ Radiography
▪️ Anal relaxation
▪️ Blood, CSF
Adverse effects
▪️ Hypotension
▪️ Hypoventilation
▪️ Pruritus
▪️ Sedation
Complications
▪️ Dural puncture – subarachnoid injection
▪️ Venous puncture
▪️ Retention of urine
▪️ Infection
▪️ Neurological sequelae
- Epidural
▪️ Drug protocol
– Bupivacaine (5mg/ml) use 0.2ml/kg
– Morphine preservative free 0.1mg/kg
– Total volume 0.2 ml/kg
▪️ The injection under Sterile procedure
– Clipping, scrub, surgical gloves
– Spinal needle – 22G; 1.5” or 2.5”
Site of injection
Epidural anaesthesia in buffalo
Sacrococcygeal space
Epidural anaesthesia in cattle
First intercoccygeal space (between the first and second coccygeal spines).
Epidural anaesthesia in horse
First intercoccygeal space.
Epidural anaesthesia in sheep and goat
Lumbosacral space.
Epidural anaesthesia in Dog
Lumbosacral space
Brachial Plexus Block
- Intravenous Regional Anaesthesia
1-Head regional anesthesia
- Upper lip and nose
Lower lip block
Mental nerve block
Mandibular nerve block
Cheek teeth, canine, incisors, skin and mucosa of the chin and lower lip.
Interpleural nerve block
- Lower limb regional anesthesia for declaw
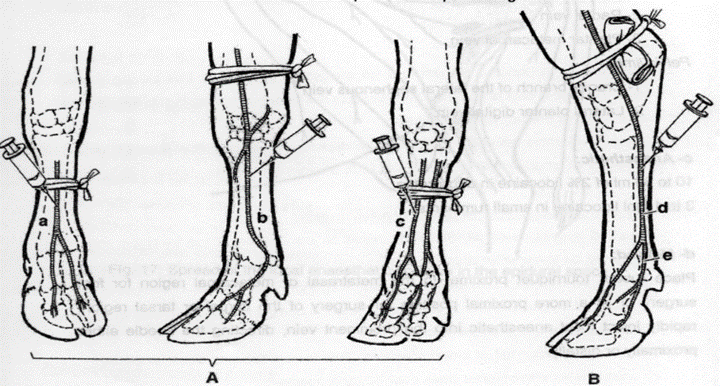
A: Fore limb (a: medial digital vein, b: lateral palmar vein, c: dorsal branch of proximal palmar vein)
B: Hind limb (d: cranial branch of lateral saphenous vein, e: lateral plantar digital vein)
Advantages of regional anesthesia
▪️ Very effective
▪️ Little side effects
▪️ Low cost
▪️ Relatively easy
- PREANAESTHETIC MEDICATIONS
Indication of preanaesthtic agents administration:
1- Reduce the amount of the general anaesthetic
2- Prolong the duration of anaesthesia.
3- Calm the patient.
4- Reduce the salivary and bronchial secretions.
5- Reduce gastric and intestinal mobility and prevent vomiting.
6- Smooth recovery.
7- Block the vago-vagal reflex, thus preventing cardiac slowing or arrest (against shock).
8- Together with local and regional analgesia / helps to restrain the patient during operation, i.e. Rumenotomy in cattle.
9- Produce muscular relaxation.
- Classification
A) Anticholinergics (atropine sulfate and scopolamine Hcl) (Parasympatholytics).
B) Atropine sulfate (Anticholinergic, parasympatholytic)
C) Tranquilizers:
|
Minor tranquilizers |
Major tranquilizers |
|
Less potent tranquilizers or central relaxants |
Potent tranquilizers or autonomic suppressants |
|
Propanediol derivatives |
Phenothiazine derivatives |
|
Mebropamate Benzodiazepines (Diazepam) |
e.g. chlorpromazine Hcl promazine Hcl Propionyl promazine Acetyl promazine |
|
Alpha2-adrenoceptor agonists e.g. Xylazine Hcl, Detomedine, Medetomidine, Romifidine |
D) Narcotics:
- Chloral hydrate (large animals)
- Morphine & morphine substitutes (methadone Hcl) ® dogs
D) Neuroleptanalgesics (Tranquilizers - Narcotic combination)
- Methadone-acetyl promazine
E) Muscle relaxants
- Tranquillizers (Atractic or neuroleptic drugs)
Types, doses and routs of administration of some tranquilizers in different animals
|
Dose |
Animal |
Trade name |
Tranquilizers |
|
|
All routes |
1-2 mg/kg b.wt. |
Dogs & cats |
LargactilÒ, NeurazineÒ |
Chlorpromazine Hcl |
|
IV / IM |
0.15-0.2 mg /kg b.wt |
Horse |
||
|
IV |
2-5 mg / kg b.wt. |
Dogs & cats |
SparineÒ |
Promazine Hcl |
|
IV |
1 mg / kg b.wt. |
Horse & cattle |
SparineÒ |
Promazine Hcl |
|
IM |
1- 3 mg/kg b.wt. |
Dogs & cats |
CombelenÒ |
Propionyl promazine |
|
IM/IV |
0.2 mg/kg b.wt. |
Horse |
CombelenÒ |
Propionyl promazine |
|
IM/IV |
1-2 mg/kg b.wt. |
Dogs & cats |
AcepromazineÒ |
Acetyl promazine |
|
IM/IV |
0.1-0.2 mg/kg b.wt. |
Horse |
AcepromazineÒ |
Acetyl promazine |
|
IM |
0.05-0.15 mg/kg b.wt |
Buffaloes |
RompunÒ |
Xylazine Hcl |
|
IM |
0.1-0.3 mg/kg b.wt |
Cattle |
RompunÒ |
Xylazine Hcl |
|
IM |
0.1-0.3 mg/kg b.wt |
Sheep & goats |
RompunÒ |
Xylazine Hcl |
|
IV/IM |
0.3-1.0 mg/kg b.wt |
Dogs |
RompunÒ |
Xylazine Hcl |
|
IM |
0.8-2.0 mg/kg b.wt |
Cats |
RompunÒ |
Xylazine Hcl |
|
IV |
1.0-1.1 mg/kg b.wt |
horse |
RompunÒ |
Xylazine Hcl |
|
IV IV IV |
5-80 mg/kg b.wt. 10-30 mg/kg b.wt. 40-80 mg/kg b.wt |
Horse Cattle Horse |
DemosedanÒ DomitorÒ SedivetÒ |
Detomedine Medetomidine Romifidine |
NB. Antidote: YohimbineÒ or Atipamezole (AnticidanÒ) (according to prescription).
Symptoms of toxic doses:
Hypotension, tremors, dyspnea, convulsions, ataxia and death.
Treatment of toxic doses:
Norepinepherine or phenylephrine
Uses
1- Therapeutic uses;
a- As preanaesthetic sedative
b- To relieve anxiety in hospitalized animals.
c- To restrain refractory animals during examination and radiology.
d- To prevent animals from licking wounds or chewing bandages and splints.
e- As an antiemetic for car sickness or prior to administration of anthelmintics.
f- For treatment in tetanus and colic.
2- In transportation or shipment of large animals.
3- For fattening (calming).
- Narcosis
A sleep-like state (unconsciousness) accompanied with varying degrees of analgesia (dulls the sense i.e. relieve pain).
Narcotics are used as a preanaesthetic in horse and in dogs.
Narcosis in Horse
- Chloral hydrate
- Increasing narcotic doses produces progressive depression of the cerebrum (mild to deep narcosis).
Narcosis in dogs:
Morphine and morphine substitutes
Dose: 5 mg/kg b.wt. SC
- Contraindicated in dogs suffering from shock, and in cats because it causes maniac state and tonic convulsions ending with death in large doses.
- Muscle relaxants
Classification of muscle relaxants:
1) Depolarizing agents:
- Succinylcholine (IV 4 mg/50 kg b.wt. for horse)
Disadvantages:
- Relaxation of intercostal muscle leading to asphyxia.
- Decamethonium (safe in pregnant animals)
2) Non-depolarizing agents:
- d-Tubocurarine chloride (2 mg/10 kg b.wt. for small and large animals)
- Gallamine (FlaxidilÒ) 1 mg/kg b.wt.
3) Dual blocking agents:
- Hexabischarbacholine
4) Miscellaneous group (central):
- Mephenesin
-Glyceryl guaicolate (Guaifenesin®): Commonly used in equine in a dose of 50 mg/kg 5% solution.
- Diazepam
Other muscle relaxant agents:
Magnesium sulfate (peripherally acting) used with chloral hydrate in treatment of tetanus (1 gm/100 kg b.wt.)
Neuroleptics as Methadone-Promazine
- GENERAL ANAESTHESIA
Definition:
It is a state of unconsciousness accompanied with hyporeflexia, analgesia and muscle relaxation. It is produced by administration of drugs having selective and reversible depression of the central nervous system.
Classification:
General anaesthesia is classified according to the rout of administration of the anaesthetic drugs into:
1- Intravenous general anaesthesia
2- Inhalation anaesthesia
3- Combination of intravenous and inhalation anaesthesia i.e. induction with intravenous and maintenance by inhalation.
Intravenous General Anaesthesia
Indications:
1- For induction of anaesthesia
2- As a sole anaesthetic agent for short term minor procedures.
Advantages:
1- Simple
2- Rapid onset
3- Relatively pleasant for animal
4- No apparatus needed
5- No explosion / pollution hazard
6- Non-irritant to airways.
Disadvantages:
1- Superficial vein may be difficult to find.
2- Animal may struggle.
3- Drug may be irritant if given perivascular.
4- Once injected it cannot be removed.
5- Drug may be cumulative
6- If the animal is not intubated, you are not ready for a respiratory emergency
7- Possible apnea on injection.
Intravenous anaesthetic drugs (Classes of drugs):
1-Barbiturates.
a- Thiopentone sodium
b- Methohexitone sodium
c- Pentobarbitone sodium
2- Propofol
3-Dissociative agents
Dogs
- Only licensed for use in combination with xylazine
- Ketamine (10 mg/kg) / Xylazine (1 mg/kg)
- Ketamine (5 mg/kg) / Diazepam (0.1 mg/kg)
Cats:
- Ketamine alone in a dose of 10-20 mg/kg IM
- Ketamine (10 mg/kg IM) / Xylazine (1 mg/kg IM)
- Ketamine (10 mg/kg IM) / Acepromazine (0.1 mg/kg IM)
4- Steroids mixture SaffanÒ
5- Neuroleptanaesthetic mixtures.
INHALATION ANAESTHESIA
Stages and planes of anaesthesia
|
Reflex response |
Muscular tone |
Pupil response to light |
Pupil size |
Eyeball position |
Cardiovascular function |
Respiration |
Stage of anaesthesia |
|
All present |
Good |
Yes |
Normal |
Central |
Normal |
Normal rate in dog (20-30 breath/min.) |
I) Induction |
|
All present |
Good |
Yes |
May be dilated |
Central may be nystagmus |
HR may increase |
Irregular , may hold breath or hypoventilation |
II) Excitement |
|
Swallowing poor or absent. Other present but diminished |
Good |
Yes |
Normal |
Central or rotated , may be nystagmus |
HR > 90 beat/min |
Regular rate (12-20 breath/min) |
III) Plane 1 Light anaesthesia |
|
Patellar, palpebral , and corneal may be present others are absent |
Relaxed |
Sluggish |
Slightly dilated |
Often rotated ventrally |
HR>90 beat/min |
Regular may be shallow (12-16 breath/min) |
III) Plane 2 Medium surgical anaesthesia |
|
All reflexes diminished or absent |
Greatly reduced |
Very sluggish |
Moderately dilated |
Centrally, may rotate ventrally |
HR is 60-90 beat/min, pulse is less stronger |
Shallow rate < 12 breath/ min |
III) Plane 3 Deep surgical anaesthesia |
|
No reflex activity |
Flaccid |
Unresponsive |
Widely dilated |
Central |
Cardiovascular collapse |
Apnea |
IÑ) Toxic stage |
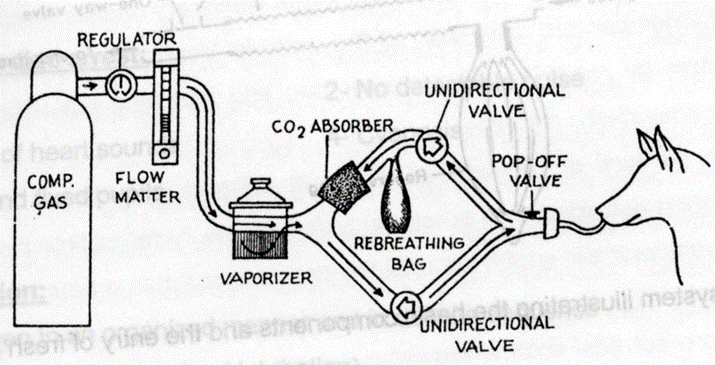
System of Classification of Inhalation Anaesthetic Apparatus
|
Closed |
Semi-closed |
Semi-open |
Open |
System |
|
Circle system |
- Circle system |
- Magill system - Ayre-piece - Norman elbow |
Mask Open drop Anaesthetic box |
|
|
Yes |
Yes |
Yes |
No |
Reservoir bag |
|
Complete |
Partial |
No |
No |
Rebreathing |
|
Yes |
Yes |
No |
No |
Co2-absorber |
|
- Flowmeter - Vaporizer - Reservoir bag Soda lime canister |
- Flowmeter - Vaporizer - Reservoir bag Soda lime canister |
- Flowmeter - Vaporizer - Reservoir bag - O2 cylinder |
- |
Component |
- Cardiac arrest and Resuscitation
Resuscitation: restoration of life after apparent death
Permanent brain damage is the consequence when brain hypoxia exceeds 4 minutes.
Signs of cardiac arrest:
1- Apnea 2- No detectable pulse
3- Absence of heart sounds 4- Cyanosis
5- Dilated and fixed pupils
Resuscitation:
Must be given in an organized manner and in definite sequence
a- Air way patent (endotracheal intubation)
b- Breathing controlled (8-12 breath/min).
The first action to establish patent airway and controlled breathing 8-12 breath/min
c- Cardiac resuscitation.
Cardiac resuscitation refers to external massage which initially is given at a rate of at least 60 compression/min. A pause after 6 compressions should be made.
d- Drugs.
- An IV catheter must be in place for administration of isotonic fluids at a rate not exceeds 80 ml/kg/hr. During the first few minutes the drip should be rapid.
- Usually the vascular bed is dilated and the added fluid volume is helpful and often essential for cardiac filling.
- Drugs given in the first few minutes are sodium bicarbonate (NaHCO3) (2 mEq/kg) and Calcl2 (10 mg/kg) to treat metabolic acidosis and to increase myocardial contractility.
- Isoproterenal (5-30 mg) , epinephrine (100 mg) or dobutamine (5-10 mg/kg/min) can be given to support ventricular function.
-References
1. Kurt A. Grimm، Leigh A. Lamont، Sheilah A. Robertson، Stephen A. Greene، William J. Tranquilli (2015). Veterinary Anesthesia and Analgesia
2. Daniel S. J. Pang، Gareth E. Zeiler (2024). Fundamental Principles of Veterinary Anesthesia
3. HuiChu Lin, Thomas Passler and Stuart Clark-Price (2022) Farm Animal Anesthesia: Cattle, Small Ruminants, Camelids, and Pigs, 2nd Edition
4. Janyce L. Cornick-Seahorn (2001). Veterinary Anesthesia The Practical Veterinarian
5. Lumb & Jones' Veterinary Anesthesia and Analgesia (William J. Tranquilli, John C. Thurmon, Kurt A. Grimm, 2007)
6. Small animal regional anesthesia and analgesia. (Luis Compoy) Wiley-Black Well. 2013
7. Textbook of Veterinary Diagnostic Radiology (Donald E. Thrall, 2002)
8. Veterinary Emergency and Critical Care Procedures Timothy B. Hackett, Elisa M. Mazzaferro,
9. In: Veterinary Medicine: A Textbook of the Diseases of Cattle, Horses, Sheep, Pigs, and Goats (11th ed.), Elsevier, St Louis, MO (2017), pp. 501-523.
10. Trent AM. Surgery of the abomasum. In: Fubini SL, Ducharme NG, editors. Farm
a. animal surgery. St Louis (MO): Saunders; 2004. p. 196–239.
11. Surgical Diseases and Techniques of the Digit. Andre Desrochers, David E. Anderson, Guy St. Jean,Vet Clin Food Anim 24 (2008) 535–550. doi: 10.1016/j.cvfa.2008.07.005.
12. 4- Mondal S, Karnam S.S, Baranwal A.K, Das P. Medial patellar desmotomy by blind method In large ruminants during upward Patellar fixation. Explor. Anim. Med. Res. 2013;3:183–185.
13. 5- Brooks, J.H. (2007) Intermittent Upward Fixation of Patella in the Horse: A Literature Review.
14. 6- Stashak, T.S. (2002) Upward Patellar Fixation. In: Adam’s Lameness in Horse, 5th Edition, Lippincott, Williams and Wilkins, New York, 737-741.
15. 7- Maggie, P., Koontz, Z.D., Lynch, T.M., Hughes, F.E. and Slone, D.E. (2015) Outcome of Medial Patellar Ligament Desmoplasty for Treatment of Intermittent Upward Fixation of the Patella in 24 Horses (2005-2012). Canadian Veterinary Journal, 56, 193-195.
16. Lumb & Jones' Veterinary Anesthesia and Analgesia (William J. Tranquilli, John C. Thurmon, Kurt A. Grimm, 2007)
17. Small animal regional anesthesia and analgesia. (Luis Compoy) Wiley-Black Well. 2013
18. Textbook of Veterinary Diagnostic Radiology (Donald E. Thrall, 2002)
19. Veterinary Emergency and Critical Care Procedures Timothy