The Procedural Work for Allergy
| Site: | EHC | Egyptian Health Council |
| Course: | Evidence of nursing procedures for internal sections |
| Book: | The Procedural Work for Allergy |
| Printed by: | Guest user |
| Date: | Tuesday, 5 May 2026, 11:38 PM |
Description
"last update: 17 April 2025" تحميل الدليل
- Prepared by
Inpatient guide
Under supervision
- Prof. Dr. Mohamed Latif, CEO of the Egyptian Health Council
Dr. Kawthar Mahmoud, Head of the Egyptian Nursing Syndicate - Member of the Senate
Prepared by
|
Title |
Name |
NO. |
|
Dean Of Faculty Nursing, Professor of Medical and Surgical Nursing, Tanta University |
Dr Afaf Abdel Aziz Abdel Aziz Basal |
1 |
|
Professor Of Critical Care Nursing |
Prof.Dr/Zeinab Hussain Ali |
2 |
|
Professor And Head of the Department of Medical Surgical Nursing. Faculty-. Benha University |
Amal Said Taha Refaie |
3 |
|
Supervisor Of the Education Sector at Port Said University |
Amal Ahmed Khalil Morsy |
4 |
|
Professor Of Medical Surgical Nursing- Faculty of Nursing- Cairo University |
Dr. Hanan Ahmed Al Sebaee |
5 |
|
Head of central administration on secondment at MOHP |
Dr Neveen ab drab al0nabi Mohamed |
6 |
|
Director Of Primary Health Care Nursing Department at MOHP. |
Maysa Hosny Ahmed Tammam |
7 |
|
Supervisor Of Technical Education- EHA |
Nancy Alaa Eldeen Abd-Elbaset Ali |
8 |
|
Supervisor Of Nursing Services Development- EHA |
Sherien Mohamed Saad |
9 |
|
Assistant Professor of Maternity and Neonatal Health Nursing - Faculty of Nursing- Ain Shams University |
Assist.Perof. Dr./Heba Mahmoud Mohammed |
10 |
|
General manager of general administration of health institutes affairs |
Dr Mai Galal Ibrahim Al-Assal |
11 |
|
Participants |
||
|
Head of nursing administration at EHA, Ismailia branch |
Ms. Nahla Kamel Mostafa |
12 |
|
member of the Nursing administration at EHA, Ismailia branch |
Ms. Maha Mohamed Saad |
13 |
|
member of the Nursing administration at EHA, Ismailia branch |
Mr. Tharwat Abdel-Al Mohamed |
14 |
|
nursing specialist at the General Administration of Nursing - MOHP |
Mr. Mona Ali Abdul Rahman Al-Katami |
15 |
|
nursing specialist at the General Administration of Nursing - MOHP |
Ms. Sherine Abdel Hakim Abdel Hakim Khattab |
16 |
|
nursing specialist at the General Administration of Nursing - MOHP |
Mr. bahaa fuoad barsom |
17 |
- Oath of Profession
"I swear by Almighty God that I will be loyal to my
work, fear God in my profession, respect its laws and regulations, and perform
my duties with competence and dedication.
I will rely in my performance on knowledge derived from the sciences of nursing
and exert my utmost effort to care for those entrusted to my care, protect
their dignity, maintain their confidentiality, defend their rights, and protect
them from harm.
I will not fear any reproach in speaking the truth, and I will provide a safe
environment for the patient, the family, and the community.
I will continue to develop myself, honor and respect those who have taught me,
and cooperate with my colleagues in the profession for righteousness and piety.
And I bear witness before God to what I say."
- Vision and Mission of Nursing Care
Vision of Nursing Care in the Inpatient Care Unit
The nursing staff of the inpatient care unit aspires to elevate the nursing profession and provide effective, safe, and high-quality nursing care to patients in the unit in accordance with Egyptian, national, and international standards.
Mission of Nursing Care in the Inpatient Care Unit
The nursing staff of the inpatient care unit is committed to improving the health status of patients and providing the best nursing care in line with the hospital’s goals, procedures, and nursing management. It also works on advancing the scientific and practical level of all nursing staff in the unit and shifting their orientation toward modern trends in nursing and medical sciences.
- Nursing Care for Allergy Patients
Anaphylaxis
Medications are widely used to treat diseases and eliminate problems that still
pose a threat to our health. However, sometimes our bodies react differently to
certain medications, leading to allergic reactions, known as "drug
allergy."
Drug allergy occurs in about 5% of people who take medication. It is important
to recognize the allergy before it is too late, as the symptoms of drug allergy
intensify with increased sensitivity.
Allergy is an immune system response to certain substances (such as pollen, fungi, some foods, etc.). Normally, the immune system fights harmful substances that enter the body, but in the case of allergies, it mistakenly treats some substances as harmful by producing antibodies that cause allergic symptoms.
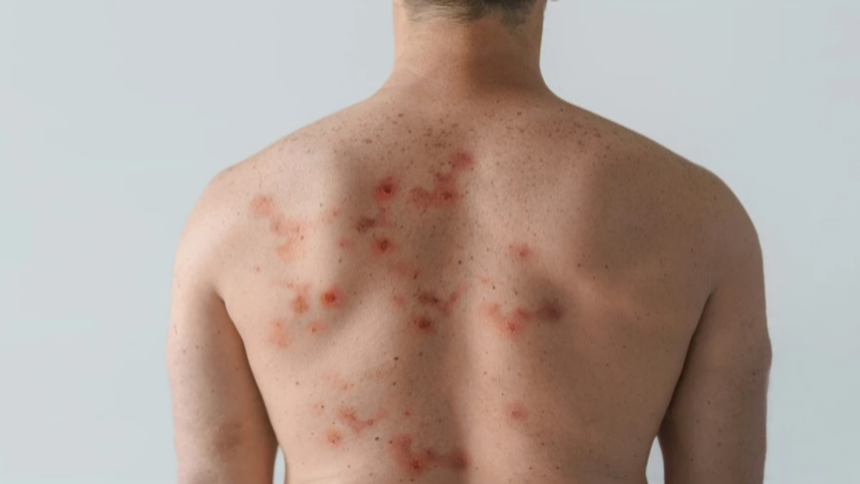
Drug Allergy
Drug allergy is a negative reaction to a medication that affects your body. This happens due to the immune system's response to the drug, which it perceives as an enemy and reacts to it. As a result, you may develop an allergy that lasts for a few days until the drug's effects wear off. There is a difference between the side effects of a drug and an actual allergy to the drug. People usually experience drug side effects, but only about 5-10% of people actually suffer from drug allergies.
Symptoms of Drug Allergy
Drug allergies have some clear symptoms in the affected person, which may include:
- Skin rashes
- Sudden high fever that lasts for several days
- Difficulty breathing
- Behavioral changes
- Irritation and itching
Risks of Drug Allergy
In most cases, drug allergies do not cause significant harm or risks to health. However, a person may become allergic to a particular medication, and the situation could worsen. If not treated promptly and symptoms continue to escalate, it can affect other organs and bodily functions. Severe drug allergies can lead to life-threatening complications. For example, anaphylaxis is a sudden allergic reaction that occurs in the body due to a drug or allergen entering the system. Due to this allergy, another reaction occurs in the body after taking the drug, which can lead to various heart and respiratory issues.
Drugs That Can Cause Allergies
It depends on the individual, as different people may be allergic to different types of medications. However, there are some drugs that people are commonly allergic to:
- Antibiotics, such as penicillin or sulfa-based antibiotics commonly used in medicine.
- Aspirin, which is widely used but can also cause drug allergies.
- Chemotherapy drugs.
- Dyes used in X-rays.
- Some non-steroidal anti-inflammatory drugs (NSAIDs) that are widely consumed.
- Drugs containing antibody-based treatments.
Definition of Anaphylactic Shock (Hypersensitivity):
Anaphylactic shock is a severe allergic reaction that can impair breathing, cause a significant drop in blood pressure, and affect the heart rate. It may appear within minutes of exposure to the allergen.
Allergy Triggers:
- Some foods (e.g., eggs, nuts, fish, certain fruits, etc.).
- Insect stings (e.g., bees, etc.).
- Latex allergy (used in gloves, balloons, erasers, rubber balls, some lab tubes and stoppers, etc.).
- Some medications, like antibiotics and aspirin.
- Certain substances used in medical tests, such as the dye used in radiology procedures.
Signs of Anaphylactic Shock:
- Swelling of the lips, tongue, face, or eyes.
- Rapid heart rate.
- Swelling and tightness in the throat.
- Difficulty breathing and speaking.
- Skin rash, vomiting, or abdominal pain.
- Dizziness, fainting, or loss of consciousness.
Treatment:
Anaphylaxis is an emergency condition that can be life-threatening. If someone exhibits symptoms of anaphylaxis, the following steps should be taken:
- Discontinue the medication: If the doctor determines an allergy to a medication or a potential allergy, the first step is to stop using that drug. This may be the only necessary intervention in many cases.
- Antihistamines: The doctor may prescribe an antihistamine or recommend an over-the-counter antihistamine, such as diphenhydramine (Benadryl). Antihistamines prevent the immune system from releasing certain chemicals during an allergic reaction.
- Corticosteroids: Corticosteroids may be taken orally or through injection to treat inflammation caused by more severe reactions.
- Anaphylactic Shock Treatment: Anaphylactic shock requires immediate injection of epinephrine (adrenaline). Hospital care is also necessary to maintain blood pressure and support breathing.
- Epinephrine Injection: The person should be injected with an epinephrine injection (epinephrine) as per the doctor’s instructions.
- Immediate reporting to a doctor.
- Administering antihistamines according to the doctor's instructions.
- Removing the allergen (e.g., any insect residue stuck to the skin if it caused the sting).
- Laying the person on their back and elevating their legs unless they are having difficulty breathing and need to sit up to help with breathing. If the person is pregnant, they should lie on their left side.
Epinephrine Injection:
This is a pre-filled self-injection containing adrenaline (epinephrine), specifically for immediate treatment during a severe allergic reaction (anaphylaxis) in patients who are at risk. Each injection contains one dose (one-time use) of epinephrine, which is discarded after use.
Conditions That Require Epinephrine Injections:
- Patients with anaphylaxis due to:
- Insect stings (e.g., bee, wasp, fire ants).
- Certain foods.
- Diagnostic test substances (e.g., radiology dye) and other allergens.
- Idiopathic anaphylaxis (unknown cause).
- Exercise-induced anaphylaxis.
Precautions Before Taking the Injection:
You should inform the doctor in the following medical conditions:
- If the patient is allergic to the injection or any of its components.
- If the patient has any of the following health problems: heart problems, high blood pressure, diabetes, thyroid issues, glaucoma, asthma, depression, Parkinson’s disease, kidney or prostate problems.
General Guidelines:
- It is crucial to know your allergens and avoid them.
- The injection is given into the middle of the outer thigh.
- Do not inject it into veins, hands, or feet. If accidentally injected in any other part of the body, seek emergency medical care immediately.
- Ensure the legs of a child are stabilized to limit movement during the injection.
- The injection should be regularly checked to ensure the solution isn’t pink, brown, cloudy, or contains particles.
- Epinephrine is sensitive to light and should be stored in its protective outer container to shield it from light.
- Avoid exposing the syringe to extreme cold or heat. Store it away from direct sunlight.
- The syringe is for single-use only.
- Do not reuse the remaining liquid from the syringe.
- Recognize the symptoms of an allergic reaction and know what to do in an emergency.
- Report to the doctor if any signs of infection (e.g., persistent redness, warmth, swelling) are observed at the injection site.
- Symptoms such as an increased heart rate, sweating, nausea, vomiting, pale skin, dizziness, or headaches may occur, but they usually subside with rest.
Drug Allergy Test
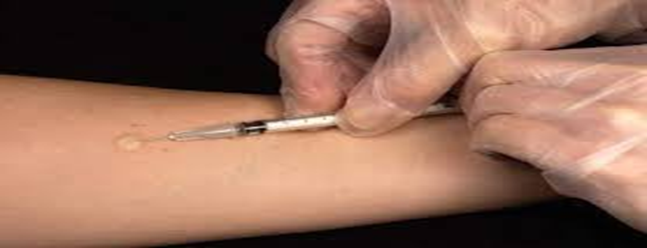
- Simple hand washing
- Preparation of tools and equipment: Alcohol wipe, ballpoint pen, latex gloves, 10cc syringe, insulin syringe, prescribed medication
- Explain the procedure to the patient
- Maintain patient privacy
- Wash hands thoroughly and wear latex gloves
- Clean the test site with alcohol
- Draw small marks on the skin and place a drop of the allergen extract next to each mark, then wipe them off
- This type of test uses very fine needles that barely penetrate the skin surface
- There will be no bleeding, but temporary discomfort may be felt, and a small bubble may form on the skin
- The results will appear within 15 minutes
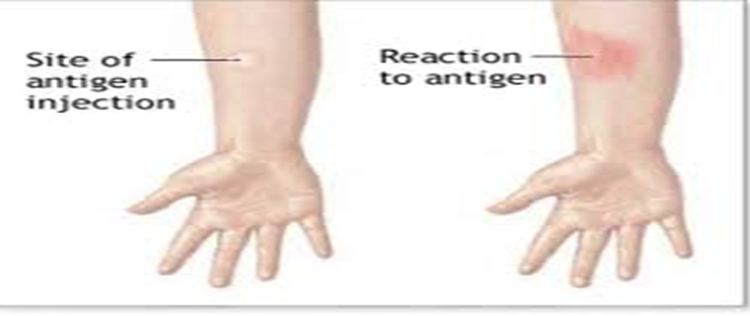
- If the patient is allergic to any of the substances being tested, a raised red and itchy bump will develop
- The skin prick test (SPT) is globally accepted and recommended as the first step in diagnosing allergies, as it is safe, easy, time-efficient, and will not trigger significant allergic reactions
- Perform subcutaneous injection steps at a 45-degree angle for a 3cc syringe and horizontally for an insulin syringe
- When injecting, only 1ml of the medication to be tested is injected
- Mark the area around the injection site
- Observe the injection site for 10 minutes after injection
- Report to the doctor if any reaction occurs (redness, swelling, or tendency to itch)
- Record this on the patient's ticket and allergy card
- Prepare the syringe with the medication to be administered and inject the patient if no reaction occurs
- Complete the remaining steps as usual for subcutaneous injection.
- References
- Procedural Work Manual, Inpatient Department, 2017