Care for cancer patients with artificial openings
| Site: | EHC | Egyptian Health Council |
| Course: | Evidence of nursing procedures for the Oncology Department |
| Book: | Care for cancer patients with artificial openings |
| Printed by: | Guest user |
| Date: | Wednesday, 6 May 2026, 2:33 AM |
Description
"last update: 5 May 2025" تحميل الدليل
Table of contents
- - Prepared by
- - Introduction to the Concept of Artificial Openings
- - Types of Artificial Openings in the Abdominal Wall
- - Colostomy
- - Types of Colostomy
- - Reasons for Colostomy Surgery
- - Types of Colostomy
- - Colostomy Care
- - Types and Sizes of Colostomy Bags
- - How to Care for the Colostomy?
- - Dietary Recommendations for Colostomy Patients
- - General Tips for Colostomy Patients
- - Impact of Colostomy on Daily Life
- - Consult a Doctor After a Colostomy Procedure
- - Urostomy
- - Types of Urostomy
- - Reasons for Urostomy Surgery
- - Complications of Urostomy
- - Urostomy Care
- - Types of Urostomy Bags
- - Nursing Care for Urostomy Patients
- - Dietary Tips for Urostomy Patients
- - General Tips for Urostomy Patients
- - Impact of Urostomy on Daily Life
- - When to Consult a Doctor After Urostomy
- - References
- Prepared by
Oncology guide
Under supervision
- Prof. Dr. Mohamed Latif, CEO of the Egyptian Health Council
Dr. Kawthar Mahmoud, Head of the Egyptian Nursing Syndicate - Member of the Senate
Supervised by
Prof. Dr. Hussein Khaled, former Minister of Higher Education
Prepared by
|
Title |
Name |
NO. |
|
Dean Of Faculty Nursing, Professor of Medical and Surgical Nursing, Tanta University |
Dr Afaf Abdel Aziz Abdel Aziz Basal |
1 |
|
Professor Of Critical Care Nursing |
Prof.Dr/Zeinab Hussain Ali |
2 |
|
Professor And Head of the Department of Medical Surgical Nursing. Faculty-. Benha University |
Prof.Dr Amal Said Taha Refaie |
3 |
|
Supervisor Of the Education Sector at Port Said University |
Prof.Dr Amal Ahmed Khalil Morsy |
4 |
|
Professor Of Medical Surgical Nursing- Faculty of Nursing- Cairo University |
Dr. Hanan Ahmed Al Sebaee |
5 |
|
Head of central administration on secondment at MOHP |
Dr Neveen ab drab al0nabi Mohamed |
6 |
|
Director Of Primary Health Care Nursing Department at MOHP. |
Maysa Hosny Ahmed Tammam |
7 |
|
Supervisor Of Technical Education- EHA |
Nancy Alaa Eldeen Abd-Elbaset Ali |
8 |
|
Supervisor Of Nursing Services Development- EHA |
Sherien Mohamed Saad |
9 |
|
Assistant Professor of Maternity and Neonatal Health Nursing - Faculty of Nursing- Ain Shams University |
Assist.Perof. Dr./Heba Mahmoud Mohammed |
10 |
|
General manager of general administration of health institutes affairs |
Dr Mai Galal Ibrahim Al-Assal |
11 |
- Introduction to the Concept of Artificial Openings
An artificial opening is the result of a procedure designed to remove disease and relieve symptoms. It is an artificial opening that allows stool to exit the intestines or urine from the ureter. The opening is created by bringing the end of the intestine through the abdominal wall to form the artificial opening.
- Types of Artificial Openings in the Abdominal Wall
There are two types of artificial openings related to the digestive system:
- Colostomy (Colon Stoma):
- A part of the patient's large intestine (called the colon) is brought to the abdominal wall to form an opening.
- This allows stool to pass through the opening, typically on the left side of the abdomen, where the stool is more solid.
- The presence of this opening means that the patient cannot control defecation, requiring a bag to be attached to the opening to collect the stool.
- Ileostomy:
- When a portion of the small intestine (called the ileum) is brought to the abdominal wall to form the opening.
- The stool is more liquid in this part of the intestine and is typically found on the right side of the abdomen.
- Like colostomy, the presence of this opening means the patient cannot control defecation, requiring a bag to collect the stool.
- Colostomy
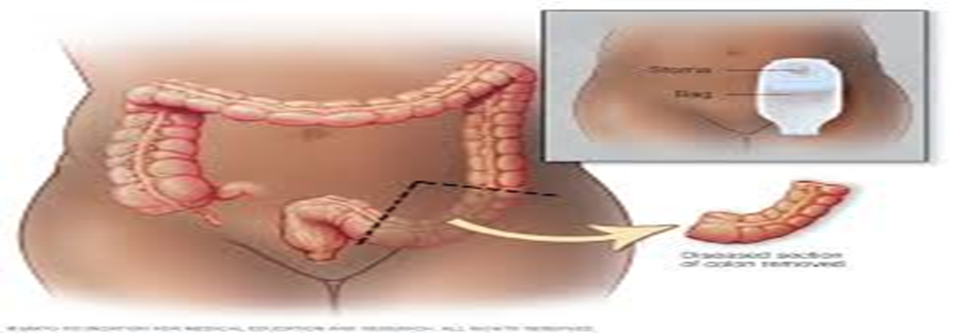
Colostomy is a surgical procedure where part of the colon is connected to the abdominal wall, leaving the patient with an opening called a "colostomy." This opening is formed from the end of the removed part of the colon, which is stitched to the skin at the edges of the incision. This is the main exit for food waste, which is collected in special plastic bags either temporarily or permanently, with changes as needed.
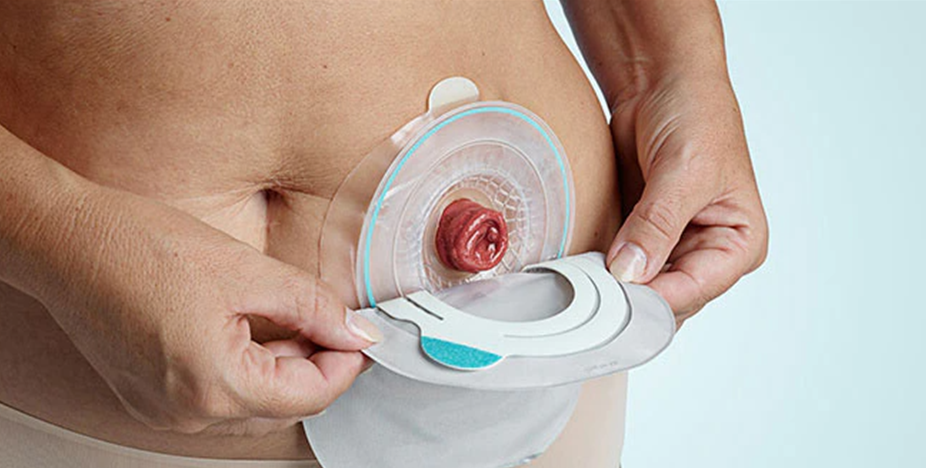
There are two types of colostomy surgery:
- Terminal Colostomy: When the opening is made at the end of the colon, and the other part of the colon is either removed or stitched shut.
- Loop Colostomy: This is often used in emergencies, and the opening is temporary and larger, where a loop of the intestine is brought to the abdominal wall and fixed in place with an external device. The intestine is then stitched to the abdomen, creating two openings: one for stool and the other for mucus.
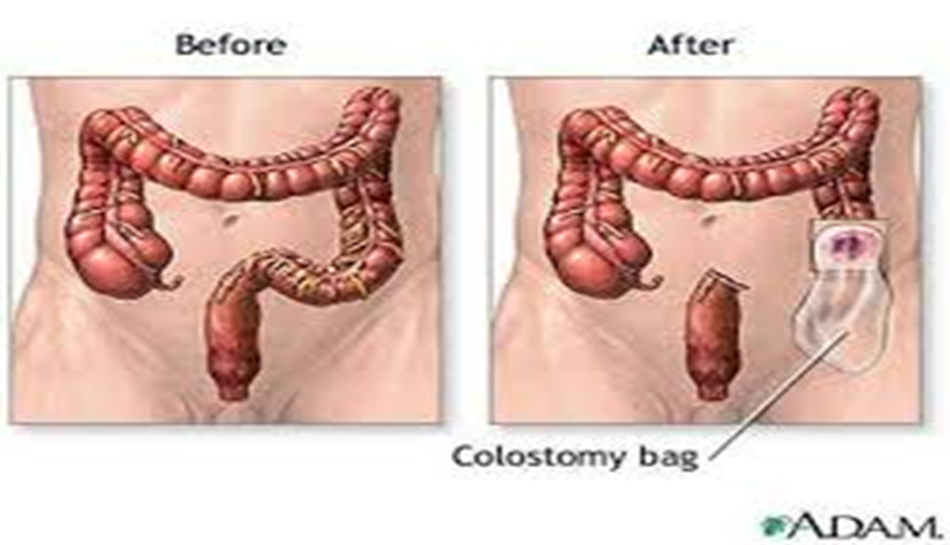
- Types of Colostomy
- Surgical Site Locations:
- Sigmoid Colon: The most common location, found in the lower left side of the abdomen, where most colon cancers occur.
- Ascending Colon: The least common type of colostomy.
- Transverse Colon: May result in one or two openings in the upper or mid-abdomen.
- Descending Colon: This type is the most common and typically produces semi-formed to well-formed stool.
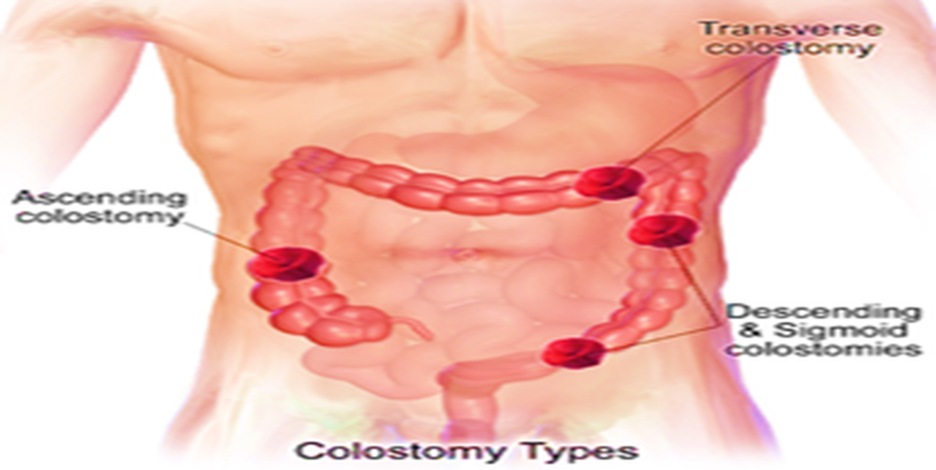
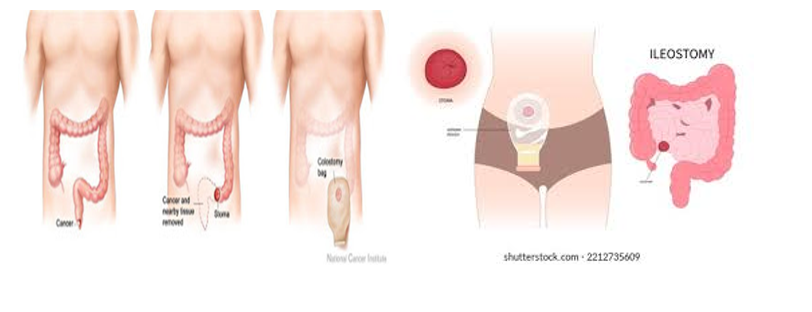
Artificial Opening Types in the Colon:
- Loop Colostomy: Often used in emergencies, temporary and large, with two openings: one for stool and the other for mucus.
- End Colostomy: Created by removing part of the intestine and closing off one end.
- Double Barrel Colostomy: Both ends of the colon are brought to the surface, but only one opening is functional.
- Ileostomy:
- When a portion of the small intestine (called the ileum) is brought to the abdominal wall to form the opening.
- The stool is more liquid in this part of the intestine and is typically found on the right side of the abdomen.
- Like colostomy, the presence of this opening means the patient cannot control defecation, requiring a bag to collect the stool.
- Reasons for Colostomy Surgery
- Removal of part of the colon for various reasons where stool cannot pass through the anus.
- Surgery on part of the colon or large intestine requiring rest for healing, making the colostomy temporary.
- Fecal incontinence unresponsive to other treatments.
- Types of Colostomy
The artificial opening can be either temporary or permanent.
1. Permanent Colostomy:
Reasons for a permanent colostomy include:
o Colon cancer
o Rectal cancer
2. Temporary Colostomy:
Reasons for a temporary colostomy include:
o Injuries to the colon or rectum, such as gunshot wounds or knife stabs
o Facilitating the repair of certain types of fistulas.
Complications of Colostomy Surgery:
- Severe colon protrusion from the opening (Prolapse)
- Colon retraction from the opening
- Necrosis at the distal end of the colon
- Narrowing of the opening (Stenosis)
- Hernia
- Bleeding
- Diarrhea
- Colostomy Care
Important Principles:
- A patient with a colostomy must learn the care techniques from the nurse before leaving the hospital so they can be independent in their own care afterward.
- It is beneficial for a family member to learn how to care for the colostomy in case assistance is needed.
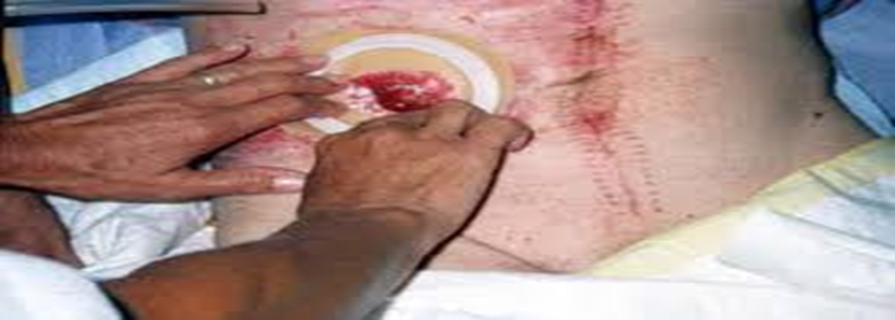
- The appearance of the stoma is generally red, and its diameter ranges between 2–5 cm. It swells immediately after surgery and then gradually becomes less red over time.
- There is no pain when touching the stoma tissue because it is nerve-free, but it may bleed slightly during cleaning or wiping. This is normal and not a cause for concern.
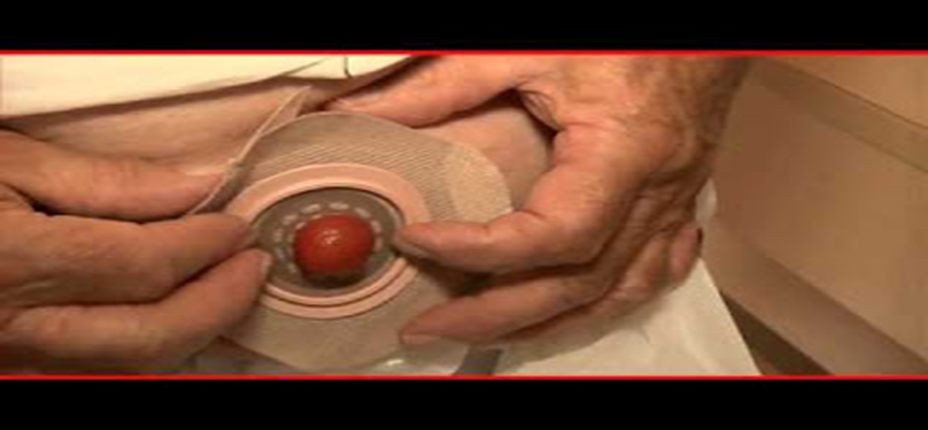
- To correctly apply a colostomy bag, the skin around the stoma must remain healthy and dry.
- Before leaving the hospital, the patient should be trained on how to select and apply the colostomy bag and care for the skin around the stoma.
Once the patient has recovered from surgery, they will need to empty the colostomy bag several times a day. The patient will not be able to control when feces and gas enter the bag. It is best to empty it when the bag is less than half full.
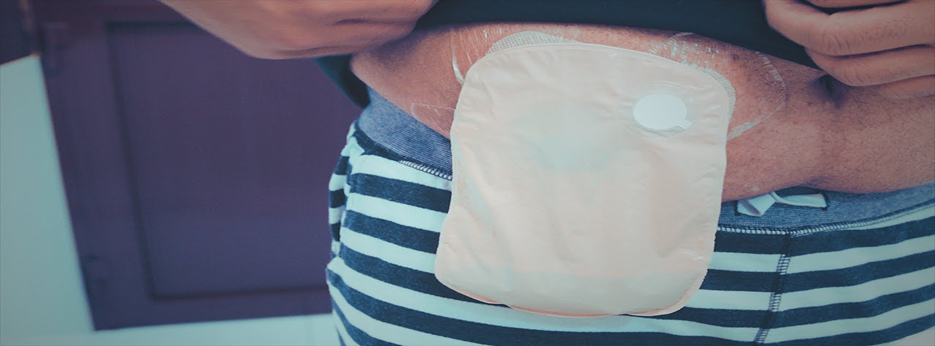
- Types and Sizes of Colostomy Bags
Colostomy bags come in many shapes and sizes, but there are two main types:
• One-piece bags that attach directly to the skin barrier.
• Two-piece bags that have a detachable skin barrier and bag. Other options include open-ended or disposable bags and closed or non-disposable bags. Some bags come with a filter to remove odors and vent gas. This prevents the bag from expanding, detaching from the abdomen, or bursting.
The patient should ask their healthcare team about which type of colostomy bag they will use.



- How to Care for the Colostomy?
Step 1: Prepare the Necessary Tools and Gather Them in a Designated Area:
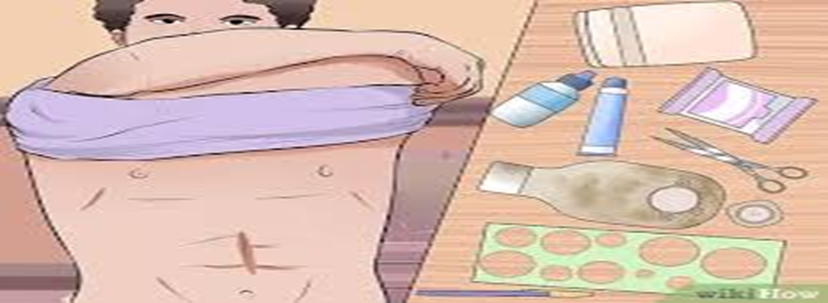
- The appropriate colostomy bag with the right circular measurement. It comes in two forms:
- Open at the bottom for easy cleaning with a clip to seal it.
- Some may include a filter inside.
- Closed at the bottom for single-use.

- Scissors.
- A small waste disposal bag.
- Saline solution.
- Soft toilet paper.
- Powder to reduce sensitivity around the stoma.
- Medical silicone.

Step 2: How to Apply the Colostomy Bag:
- Cut the circular base or bag slightly larger than the stoma before removing the adhesive from the abdominal wall, ensuring the circle is a bit larger than the stoma.
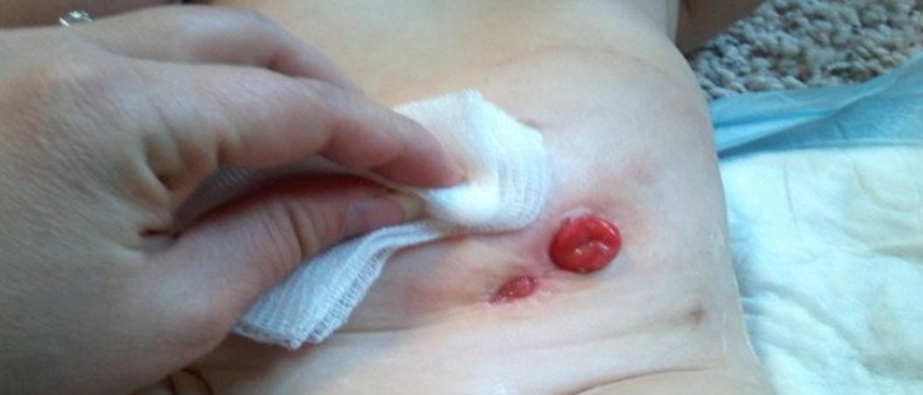
- Clean the stoma and surrounding skin with saline solution only. Soap or disinfectants (e.g., alcohol) should be avoided, as they can dry out and crack the skin.
- Dry the area around the stoma completely before applying the bag to ensure a secure attachment.
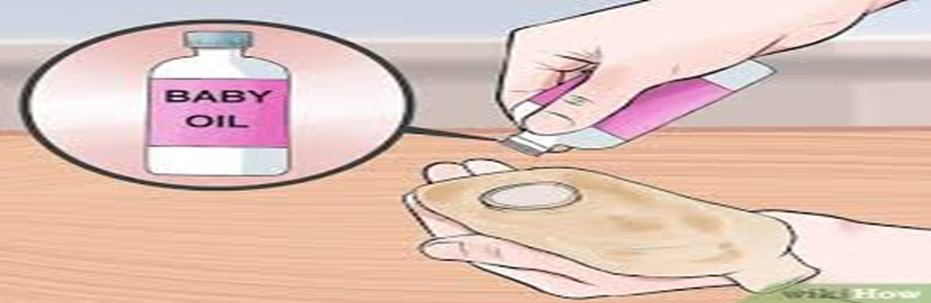 4. Apply the medical silicone
around the base where the bag will be placed.
4. Apply the medical silicone
around the base where the bag will be placed.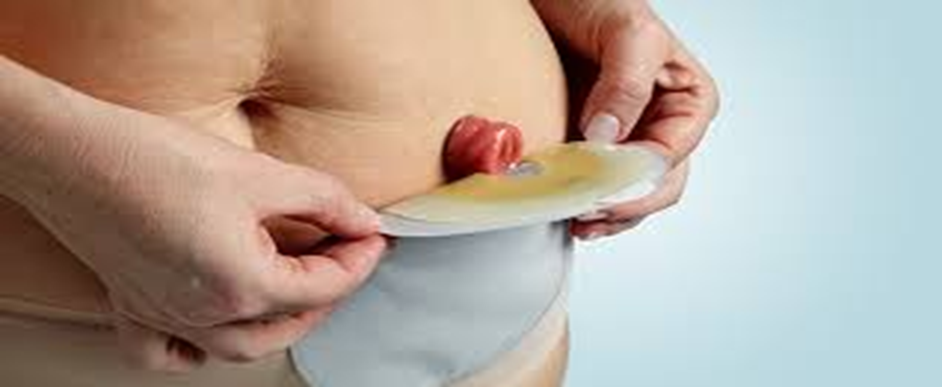 5. Carefully position and secure
the bag around the stoma.
5. Carefully position and secure
the bag around the stoma.
- Dietary Recommendations for Colostomy Patients
- Generally, the patient can eat and drink as they did before. However, they should observe how their stoma reacts to different foods.
- Eat at set times in a calm environment.
- Eat slowly and chew food thoroughly.
- Drink 2 to 4 liters of water a day for the typical stoma patient.
- Avoid gas-producing foods like cabbage, dairy, garlic, onions, and eggs.
- Increase the intake of fruits and vegetables.
- Avoid carbonated drinks.
- Eat more boiled food and avoid fried foods.
- General Tips for Colostomy Patients
- The patient should learn to live with the colostomy, as some people may feel scared, disgusted, or repulsed by it, but these feelings typically subside with time, especially with adequate support.
- Solid foods should be avoided, especially for ileostomy patients, as the small intestine is not accustomed to digesting solid foods initially.
- Ileostomy patients should always carry extra colostomy bags when traveling in case of emergencies.
- Avoid strenuous activities.
- Always be mindful of the colostomy bag.
- Empty the bag regularly.
- Drink plenty of fluids.
- Impact of Colostomy on Daily Life
- After a colostomy operation, the patient will need some time to recover. This is completely normal, and recovery time varies from person to person.
- The appearance of the stoma will change in the first weeks after surgery in terms of size and output. The patient may also gain or lose weight during this time.
- The patient is always advised to wear the colostomy bag correctly to manage output, control odors, and reduce skin irritation or damage.
- The patient should be informed that the colostomy is not an obstacle to work, daily activities, exercise, travel, or hobbies, and that the patient's physical and mental health plays a major role in determining the quality of life.
- Consult a Doctor After a Colostomy Procedure
- The skin around the colostomy turns an abnormal color or becomes painful.
- The stool has an unpleasant odor.
- Part of the intestine protrudes from the colostomy opening.
- Symptoms of obstruction occur, such as vomiting, increased abdominal pain, or bloating without passing gas.
- The patient experiences a fever without a clear cause.
- Urostomy
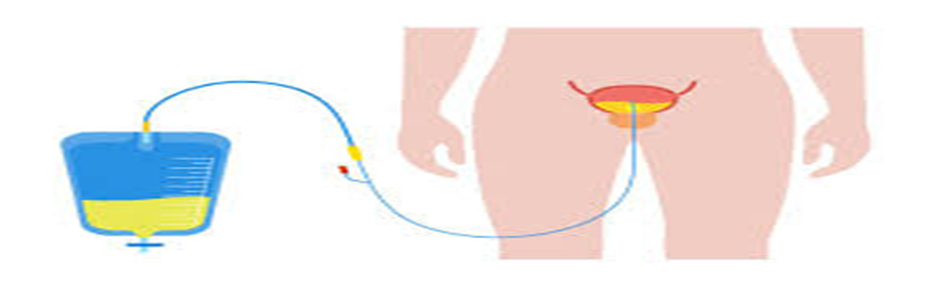
Urostomy is a surgical procedure where an opening is created in the abdomen, called a stoma, to allow urine to drain outside the body. This procedure is typically done when the bladder is damaged, diseased, or not functioning properly.
- Types of Urostomy
There are several types of urostomy procedures, each with its unique characteristics and benefits. Below are some of the most common types:
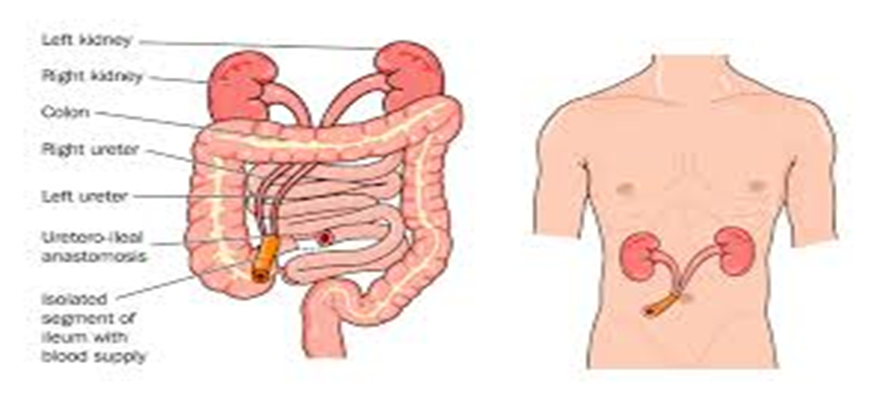
1) Ileal Loop Urostomy (Most Common)
a. Procedure: A part of the small intestine (ileum) is brought to the abdominal wall to create the stoma, and urine is collected in an external bag.
b.Benefits: Simple procedure, low complication risk, easy to manage.
2) Bowel Urostomy (Less Common)
a. Procedure: A pouch is created from the bowel to store urine, and a valve is placed at the stoma to control the flow of urine.
b. Benefits: Provides more control over urine output, reduces the need for frequent bag changes, improves quality of life.
3) Cutaneous Urostomy (Less Common)
a. Procedure: The stoma is created directly from the abdominal skin.
b. Benefits: Can be a good option for some patients but may require more frequent care and be associated with higher complication rates.
4) Percutaneous Urostomy (Similar to Cutaneous Urostomy)
- Procedure: The stoma is created through the skin, but it is often used for temporary drainage or in cases where a permanent solution is not suitable.
Choosing the type of urostomy depends on several factors, including:
- The underlying cause of bladder dysfunction
- The patient’s overall health
- The patient’s preferences and lifestyle
- Reasons for Urostomy Surgery
Urostomy surgery is often performed to treat a variety of medical conditions that affect the bladder or urinary system. Some common reasons for this procedure include:
- Bladder Cancer: If the bladder is affected by cancer, it may be necessary to perform a urostomy to remove the cancerous part of the bladder or the entire bladder.
- Spinal Cord Injuries: Spinal cord damage can disrupt the nerves that control the bladder, leading to urinary incontinence. Urostomy can help manage this condition.
- Congenital Defects: Some individuals are born with abnormalities in the urinary system that make it difficult to control urine, and urostomy may be a solution in such cases.
- Neurological Diseases: Neurological diseases such as multiple sclerosis or Parkinson’s disease can affect bladder function and may require urostomy.
- Radiation Therapy: Radiation therapy for pelvic tumors can sometimes damage the bladder, necessitating a urostomy.
- Chronic Infections: Some chronic urinary infections that do not respond to treatment may require a urostomy.
- Complications of Urostomy
- Issues Related to the Stoma:
- Hernia: Protrusion of tissue around the stoma.
- Stenosis: The stoma may narrow, limiting urine flow.
- Skin Irritation: The skin around the stoma may become irritated or painful.
- Prolapse: A part of the bowel may protrude through the stoma.
- Urinary System Complications:
- Urinary Tract Infections (UTIs): Bacterial infections can enter the stoma, possibly leading to kidney stones.
- Psychological Complications:
- Body Image: Adjusting to a visible stoma may be challenging for some individuals.
- Anxiety or Depression: Psychological difficulties may arise due to lifestyle changes or body image concerns.
- Less Common Complications:
- Stoma Reversal: Part of the intestine may protrude through the stoma.
- Bowel Obstruction: Intestinal blockages may occur in some cases.
- Urostomy Care
- Stoma Care:
- Daily Inspection: The patient is advised to check the stoma for any changes in color, size, or shape.
- Skin Care: The patient should keep the skin around the stoma clean and dry to prevent irritation.
- Protective Products: The use of creams or pastes to protect the skin from urine and leakage is recommended.
- Changing the Urostomy Device: The patient should follow healthcare provider instructions for changing the urostomy device.
- Bag Care:
- Emptying: The patient should empty the bag regularly to prevent overflow and odors.
- Cleaning: The bag and cover should be cleaned after each emptying.
- Odor Control: The patient should use odor-control products or bags with built-in odor control.
- Urinary Health:
- Hydration: The patient should drink plenty of fluids to prevent dehydration and maintain urine flow.
- Diet: The patient should follow dietary recommendations from their healthcare provider to manage any underlying health conditions or potential complications.
- Monitoring Urine Output: The patient should track urine output for any changes.
- Lifestyle Considerations:
- Activities: Patients can engage in a wide range of activities, avoiding excessive stress.
- Travel: Patients should plan their travels in advance to ensure they have sufficient supplies and access to healthcare if needed.
- Psychological Support: Emotional support from family, friends, or support groups is recommended for patients to cope with living with a urostomy.
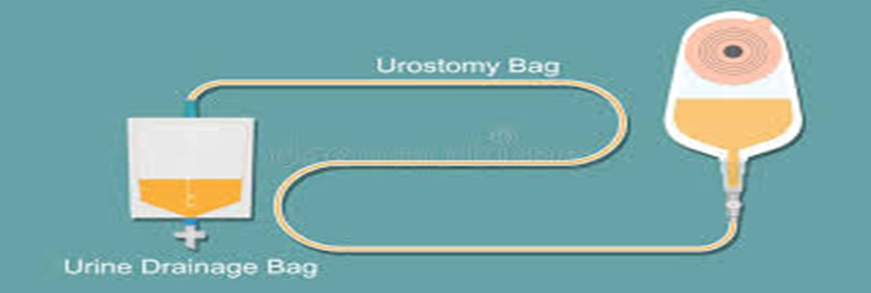
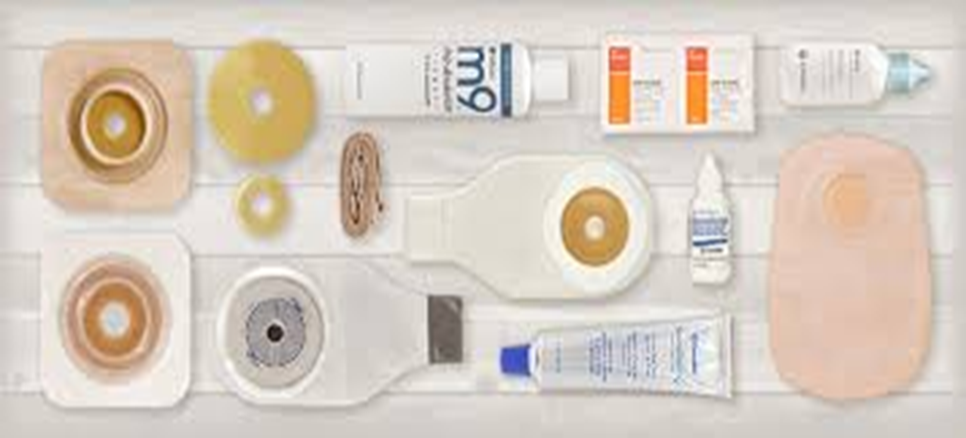
Types and Sizes of Urostomy Bags:
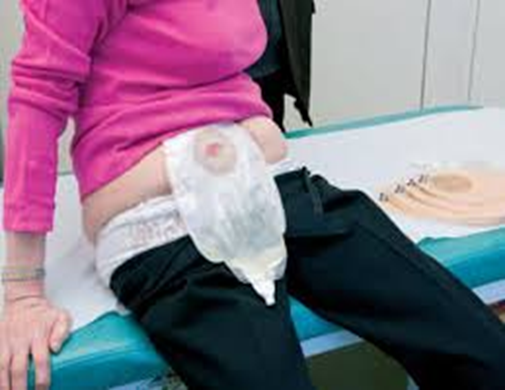
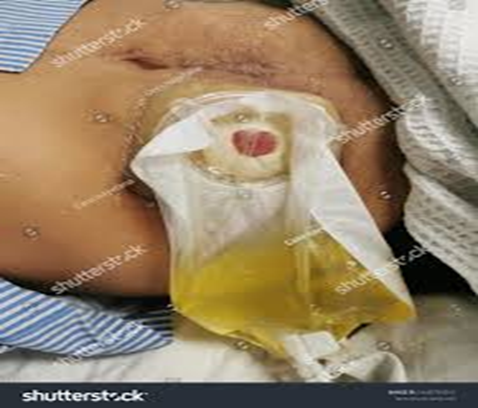
- Types of Urostomy Bags
- One-Piece: The bag and base plate (adhesive part that attaches to the skin) are integrated into a single unit.
- Two-Piece: The bag and base plate are separate, allowing flexibility in changing the bag without removing the base plate.
- Closed-End: The bag has a closed end and needs to be emptied regularly.
- Drainable: The bag has a drainage valve that allows for emptying without removing the entire bag.
- Night-Time Bags: Larger bags designed for longer wear, typically used overnight.
- Urostomy Bag Sizes: Urostomy bags come in various sizes depending on the size of the stoma and the individual’s needs. They are usually measured in millimeters. It is essential to use the correct size to ensure a secure fit and prevent leakage.
Factors to Consider When Choosing the Bag Size:
- Stoma Size: The bag should be slightly larger than the stoma to prevent skin irritation.
- Activity Level: Active individuals may prefer smaller, lighter bags.
- Urine Output: The amount of urine produced will affect the capacity of the bag.
- Comfort: Personal preferences and comfort levels should also be taken into account.

- Nursing Care for Urostomy Patients
Preoperative Care:
- Education: Comprehensive education should be provided about the urostomy procedure, including the benefits, risks, and potential complications.
- Psychological Support: Any concerns or anxieties the patient may have about the surgery and its impact on their lifestyle should be discussed.
- Physical Assessment: A thorough physical assessment should be conducted to identify any underlying health conditions that may affect the urostomy procedure.
Postoperative Care:
- Pain Management: Monitor pain levels and administer appropriate pain relief medications as prescribed.
- Stoma Care: Teach the patient proper stoma care techniques, including inspection, skin care, and device changes.
- Urine Output: Monitor urine output to ensure adequate kidney function and prevent complications.
- Nutritional Support: Provide guidelines on nutrition to maintain hydration and support healing.
- Psychological Support: Offer psychological support and encouragement to help the patient adapt to the changes associated with the urostomy.
Ongoing Care:
- Urostomy Appliance Fitting: Assist the patient in choosing the correct type and size of urostomy appliance.
- Skin Care: Provide education on preventing and managing skin irritation around the stoma.
- Self-care: Teach the patient self-care techniques, including changing the pouch, stoma care, and managing potential complications.
- Home Health Care: Coordinate home health care services as necessary to provide ongoing support and monitoring.
- Referrals: Refer the patient to support groups, therapists, or other specialists as needed.
Basic Nursing Skills:
- Wound Care: Proper wound care techniques are essential to manage the stoma and prevent complications.
- Urostomy Care: Nurses must be knowledgeable about the various types of surgeries and appropriate care techniques for each.
- Patient Education: Effective communication and patient education are critical to ensuring the patient understands and follows care instructions.
- Assessment and Monitoring: Nurses should be able to assess the patient's condition, monitor vital signs, and identify any potential complications.
- Dietary Tips for Urostomy Patients
- Hydration: Drink plenty of fluids to prevent dehydration and maintain adequate urine flow (8-10 cups of water daily unless otherwise advised).
- Fiber: A fiber-rich diet (fruits, vegetables, whole grains, legumes) can help prevent constipation and promote regular bowel movements.
- Avoid Irritating Foods: Some foods may irritate the stoma or cause digestive issues, including spicy foods, carbonated drinks, alcohol, and caffeine.
- Urinary Health: Certain foods and drinks can irritate the bladder. If the patient experiences bladder discomfort, acidic foods (citrus fruits, tomatoes), caffeine, and alcohol should be reduced or avoided.
- Sodium Intake Monitoring: Excessive sodium intake can lead to fluid retention and increased urine output. It is advised to reduce consumption of processed foods and salty snacks.
- Vitamins and Minerals: A balanced diet providing essential vitamins and minerals should be followed after consulting a nutritionist.
- Specific Nutritional Needs: If the patient has underlying health conditions such as kidney stones or gout, specific dietary modifications may be recommended.
- General Tips for Urostomy Patients
Living with a urostomy requires adjustments, but with proper care and support, a good quality of life can be maintained.
- Self-care:
- Regular Check-ups: Schedule regular follow-up appointments to monitor for any issues and address any concerns.
- Stoma Care: Provide instructions for stoma care, including inspection, skin care, and appliance changes.
- Pouch Care: Provide instructions and ensure proper care of the pouch to prevent leaks and odor.
- Hydration: Maintain hydration to ensure adequate urine flow and prevent dehydration.
- Diet: Follow a balanced diet to support overall health and any specific nutritional needs.
- Lifestyle Adjustments:
- Physical Activity: The patient should engage in regular physical activity as tolerated.
- Stress Management: Teach the patient stress management techniques such as relaxation exercises, meditation, or deep breathing.
- Psychological Support: Provide psychological support from family, friends, or support groups.
- Traveling: The patient should plan travel in advance to ensure they have the necessary supplies and access to health care.
- Additional Tips:
- Join a Support Group: Connecting with others who have undergone urostomy surgery can provide valuable support and advice.
- Consult a Stoma Care Nurse: Seek guidance and specialized assistance from a nurse experienced in urostomy care.
- Impact of Urostomy on Daily Life
Living with a urostomy may require adjustments in daily life, but with appropriate support, individuals can lead fulfilling lives. Here are some potential effects:
- Physical Changes:
- Visible Appliance: A visible urostomy pouch may affect body image and self-esteem.
- Activity Limitations: While most individuals with a urostomy can participate in a wide range of activities, there may be temporary restrictions during the initial recovery period.
- Skin Irritation: Skin irritation around the stoma may occur, requiring diligent hygiene and protective products.
- Psychological Impact:
- Body Image: Adjusting to a visible stoma may be challenging for some individuals.
- Anxiety or Depression: Emotional difficulties may arise due to lifestyle changes or body image concerns.
- Social Concerns: Individuals may feel anxious about social interactions and acceptance due to the urostomy surgery.
- Lifestyle Adjustments:
- Traveling: Travel may require additional planning, such as packing supplies and ensuring access to health care services.
- Work: Individuals with urostomies can often continue working, but accommodations such as access to private bathrooms or flexible work arrangements may be needed.
- Intimacy: Intimate relationships may be affected by the urostomy. Open communication with partners is essential.
- When to Consult a Doctor After Urostomy
Patients should consult a doctor immediately if they experience any of the following symptoms or changes:
- Stoma-Related Issues:
- Changes in size, shape, or color of the stoma
- Skin irritation or redness around the stoma
- Hernia (bulging around the stoma)
- Stoma retraction
- Stoma narrowing
- Urinary Issues:
- Frequent or urgent urination
- Pain or burning during urination
- Blood in the urine
- Foul-smelling urine
- Fever or chills
- Pouch-Related Issues:
- Persistent leakage
- Difficulty emptying the pouch
- Skin rash or irritation from the pouch adhesive
- Other Concerns:
- Changes in overall health
- Anxiety about the urostomy or its impact on life
- References
- Burgess-Stocks J. Eating with an ostomy. United Ostomy Associations of America. https://www.ostomy.org/diet-nutrition.
- Colostomy nutrition therapy. Nutrition Care Manual. Academy of Nutrition and Dietetics. https://www.nutritioncaremanual.org.
- Ileostomy nutrition therapy. Nutrition Care Manual. Academy of Nutrition and Dietetics. https://www.nutritioncaremanual.org.
- Landmann RG, et al. Ileostomy or colostomy care and complications. https://www.uptodate.com/contents/search.
- Living with an ostomy: FAQs. United Ostomy Associations of America. https://www.ostomy.org/living-with-an-ostomy.