Traumatic Brain edema
| Site: | EHC | Egyptian Health Council |
| Course: | Neurosurgery Guidelines |
| Book: | Traumatic Brain edema |
| Printed by: | Guest user |
| Date: | Wednesday, 6 May 2026, 12:53 AM |
Description
"last update: 13 March 2025" Download Guideline
- Executive Summary
This topic is concerned with diagnosis and treatment guidelines of traumatic brain edema.
➡️Recommendations:
Conservative Management of traumatic brain edema is divided into 4 tiers:
Tier 0
▪️ Head elevation.
o Strong recommendation
▪️Avoid hypoxia.
o Strong recommendation.
▪️ Avoid hypotension
o Strong recommendation.
▪️ Secure the airway (endotracheal intubation) in patients with GCS ≤8 who are unable to maintain their airway or who remain hypoxic despite supplemental O2 with ICP monitoring.
o Strong recommendation.
▪️ Brain imaging (CT) must be available and repeated as much as needed. (if not available refer to a tertiary center)
o Strong recommendation
▪️ We recommend ICU admission and close neurological observation with CT monitoring for the development and progression of brain stem compression. ( if not available refer to a tertiary center)
o Strong recommendation.
Tier 1
▪️ We recommend mannitol for control of IC-HTN (within hospitals).
▪️ Intermittent boluses may be more effective than continuous infusion
▪️ Effective doses range from 0.25–1 gm/kg body weight
▪️ Avoid hypotension (SBP < 90mm Hg) which may result from the diuretic effect of mannitol, which can lead to decreased circulating fluid volume
o Strong recommendation.
▪️ Try to adjust partial pressure of carbon dioxide (PaCO2) at lower ranges of normal values (i.e. 35-38 mmHg).
o Conditional recommendation.
Tier 2
▪️ Consider the use of neuromuscular blocking agents (NMBAs).
o Conditional recommendation
▪️ We recommend targeting a cerebral perfusion pressure (CPP) of 60-70mm Hg
o Strong recommendation.
▪️ Try to adjust the partial pressure of CO2 at 32-35 mmHg (mild hypocapnia)
o Conditional recommendation
Tier 3
▪️ High-dose barbiturate therapy may be used for IC-HTN refractory to maximal medical and surgical ICP-lowering therapy. Patients should be hemodynamically stable before and during treatment.
o Conditional recommendation
▪️ The availability of equipped neurosurgery operating room is essential for management. (if not available refer to a tertiary center)
o Strong recommendation.
➡️ Surgical Intervention:
▪️ We recommend decompressive craniectomy ± duroplasty for patients with late refractory ICP elevations
o Strong recommendation
▪️ Timing of surgery: patients meeting surgical criteria should be operated as soon as possible due to the potential for rapid deterioration
o Strong recommendation.
- Recommendations
Table 4: Medical Management
|
Items: |
Strength of Recommendation: |
Level of Evidence: |
|
▪️ Head elevation. |
Strong |
Moderate quality evidance6 |
|
▪️ Avoid hypoxia |
Strong |
Moderate quality evidance6 |
|
▪️ Avoid hypotension |
Strong |
Moderate quality evidance6 |
|
▪️ Secure the airway (endotracheal intubation) in patients with GCS ≤8 who are unable to maintain their airway or who remain hypoxic despite supplemental O2 with ICP monitoring |
Strong |
Moderate quality evidance6 |
|
▪️ Brain imaging (CT) must be available and repeated as much as needed. (if not available refer to a tertiary center) |
Strong
|
Moderate quality evidance6 |
|
▪️ We recommend ICU admission and close neurological observation with CT monitoring for the development and progression of brain stem compression. (if not available refer to a tertiary center) |
Strong |
Moderate quality evidance6 |
|
▪️ We recommend mannitol for control of IC-HTN (within hospitals). ▪️ Intermittent boluses may be more effective than continuous infusion ▪️ Effective doses range from 0.25–1 gm/kg body weight ▪️ Avoid hypotension (SBP < 90mm Hg) which may result from the diuretic effect of mannitol, which can lead to decreased circulating fluid volume |
Strong |
Moderate quality evidance6 |
|
▪️ Try to adjust partial pressure of carbon dioxide (PaCO2) at lower ranges of normal values (i.e. 35-38 mmHg). |
Conditional
|
Low quality evidance7 |
|
▪️ Consider the use of neuromuscular blocking agents (NMBAs). |
Conditional
|
Moderate quality evidance6 |
|
▪️ We recommend targeting a cerebral perfusion pressure (CPP) of 60-70mm Hg |
Strong |
Moderate quality evidance6 |
|
▪️ Try to adjust the partial pressure of CO2 at 32-35 mmHg (mild Hypocapnia) |
Conditional |
High-Quality Evidence 8 |
|
▪️ High-dose barbiturate therapy may be used for IC-HTN refractory to maximal medical and surgical ICP-lowering therapy. Patients should be hemodynamically stable before and during treatment. |
Conditional
|
High-Quality Evidence 8 |
|
▪️ The availability of equipped neurosurgery operating room is essential for management. (if not available refer to a tertiary center) |
Strong
|
High-Quality Evidence 8
|
Table 5: Surgical Intervention
|
Items: |
Strength of Recommendation: |
Level of Evidence: |
|
▪️ We recommend Decompressive craniectomy ± duroplasty for patients with late refractory ICP elevations |
Strong
|
Low quality evidance9 |
|
▪️ Timing of surgery: patients meeting surgical criteria should be operated as soon as possible due to the potential for rapid deterioration |
Strong recommendation.
|
Low quality evidance10 |
➡️Implementation Considerations:
Training of neurosurgeons on guideline application
➡️Research gaps:
▪️ CT‐Based Classification of Acute Cerebral Edema: association with Intracranial Pressure and Outcome
➡️Clinical / Radiological Indicators:
▪️Glascow coma scale (GCS) recording
▪️CT brain request.
➡️Updating the guideline
To keep these recommendations up to date and ensure its validity it will be periodically updated. This will be done whenever strong new evidence is available and necessitates updating.
- Acknowledgement
Chair of the Committee:
Nasser M. F. El-Ghandour, MD
Members: (Alphabetically-arranged)
Abd-Elhafiz Shehab-Eldien, MD
Ahmed S. Kamel AbdelWahed, MD
Ahmed Zohdi, MD
Ayman Mohamed Ismail, MD
Diaa Eldin Galal Radwan, MD
Ihab El Refaee, MD
Mohamed Ahmed Hewedy, MD
Mohamed Khallaf, MD
Mohamed Salah Sedeek, MD
Omar Elwardany, MD
Osama Abdelaziz, MD
Sameh Saleh, MD
Waleed Abbass, MD
Zeiad Yossry Fayed, MD
We acknowledge Osama Ramadan for his collaboration with the committee during writing this chapter.
- Abbreviations
CPP: cerebral perfusion pressure.
DC: decompressive craniectomy.
EEG: electroencephalography.
EVD: external ventricular drain.
IC-HTN Intra cranial Hypertension.
ICP Intra cranial pressure.
PaCO2: partial pressure of carbon dioxide.
SBP Systolic blood pressure.
TBI: Traumatic brain injury.
- Glossary
Cerebral edema: is an increase in the water content of central nervous system [CNS] cells or interstitium.1
Refractory intracranial hypertension after traumatic brain injury: recurrent increase of intracranial pressure above 20-22 mmHg for sustained period of time (10-15 min), despite conventional therapies, such as osmotic therapy, cerebral spinal fluid drainage and mild hyperventilation.2
- Introduction
Posttraumatic cerebral edema is a complex process. The incidence is around 60% in trauma-related hematoma or mass lesion and around 15% without mass lesions. cerebral edema is described as a special condition of the brain with excessive tissue volume due to the increase water content in the brain. The excessive tissue volume leads to increase in intracranial pressure (ICP) and decrease cerebral perfusion pressure (CPP), which eventually increases the mortality after traumatic brain injury (TBI). Diverse pathways are involved in the development of cerebral edema after brain injury. 1
Mainly two types cerebral edema occur after TBI-vasogenic edema and cytotoxic edema. Vasogenic edema is the fluid accumulation in interstitial space, and cytotoxic edema is swelling of the cells. 2
Cytotoxic edema occurs due to the involvement of different pathways or ionic channels and correlates with the secondary type of brain injury.3
Vasogenic edema develops due to disruption of the blood-brain barrier (BBB) or altered permeability of BBB and correlates with the level of impact and activation of molecular pathways related with neuroinflammation. Occasionally, mixed type of cerebral edema exits due combination of the vasogenic and cytotoxic component.4
Symptoms appear as the intracranial pressure (ICP) rises above 20 cmHg in most patients. Treatment for cerebral edema targets the underlying cause and any life-threatening complications. Treatments include hyperventilation, osmotherapy, diuretics, corticosteroids, and surgical decompression.5
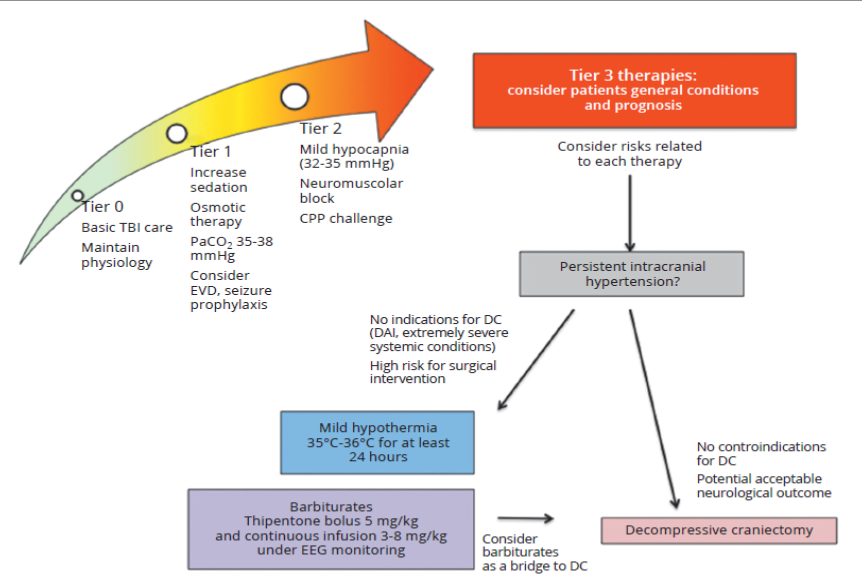
Staircase clinical approach to the use of tier-three therapies for the management of increased intracranial pressure.
- Purpose
The purpose of this multidisciplinary guideline is to identify improvement in the diagnostic tools and treatment strategies in managing patients with post traumatic brain edema and to create actionable recommendations to implement these strategies in clinical practice.
- Scope
The guidelines are concerned with recommendation for traumatic brain edema. selection of management approach (conservative - surgical) is defined. The aim is to achieve clear decision regarding each management line.
- The target audience
The guideline is intended for all neurosurgeons who are likely to diagnose and manage patients with post traumatic brain edema, and it applies to any setting in which patients with post traumatic brain edema would be identified, monitored, or managed.
- Methods
A comprehensive online search for guidelines and articles was undertaken to identify the most relevant articles to be reviewed and guidelines to consider for adaptation.
Inclusion/exclusion criteria followed in the search were:
▪️ Selecting only national and/or international guidelines.
▪️ Specific range of dates for publication (using Guidelines published or updated 2005 and later)
▪️ A large series none controlled, prospective clinical trials of treatment using surgical versus nonsurgical management have been reviewed.
▪️ Selecting peer reviewed publications only.
▪️ Selecting guidelines written in English language.
▪️ Papers with the following characteristics were also excluded: case series with less than 10 patients evaluated by CT scan and with incomplete outcome data (mortality or GOS (Glasgow outcome score)), case reports, operative series with operations occurring longer than 14 days from injury.
▪️ Excluding guidelines written by a single author, not on behalf of an organization to be valid and comprehensive, a guideline ideally requires multidisciplinary input
▪️ Excluding guidelines published without references
▪️ Selected articles were evaluated for design, prognostic significance, therapeutic efficacy, and overall outcome.
▪️ All retrieved Guidelines were screened and appraised using the AGREE II instrument (www.agreetrust.org) by at least two members. The panel decided on a cut-off point or ranked the guidelines (any guideline scoring above 50% on the rigour dimension was retained). We selected “Guidelines for the Management of Severe Traumatic Brain Injury 4th Edition: Brain Trauma Foundation: September 2016.6
➡️Evidence assessment:
According to the WHO Handbook for Guidelines, we used the GRADE (Grading of Recommendations, Assessment, Development and Evaluation) approach to assess the quality of a body of evidence, develop and report recommendations. GRADE methods represent internationally agreed standards for making transparent recommendations. Detailed GRADE information is available on the following sites:
■ GRADE working group: https://www.gradeworkinggroup.org/
■ GRADE online training modules: http://cebgrade.mcmaster.ca/
Table 1: Quality of evidence in GRADE
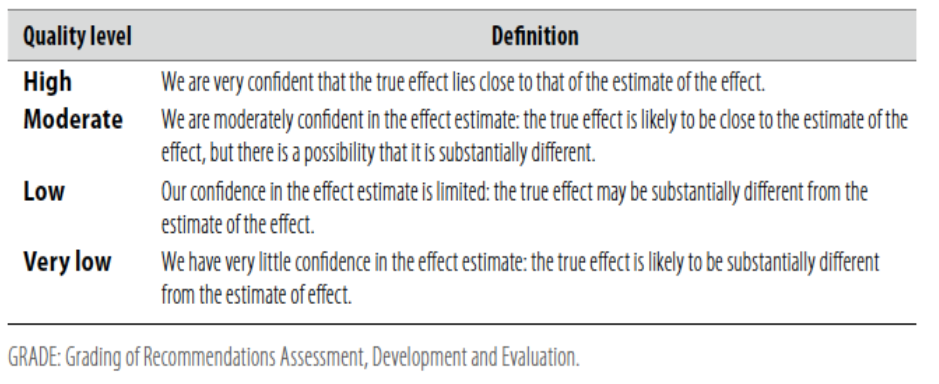
Table 2: Significance of the four levels of evidence
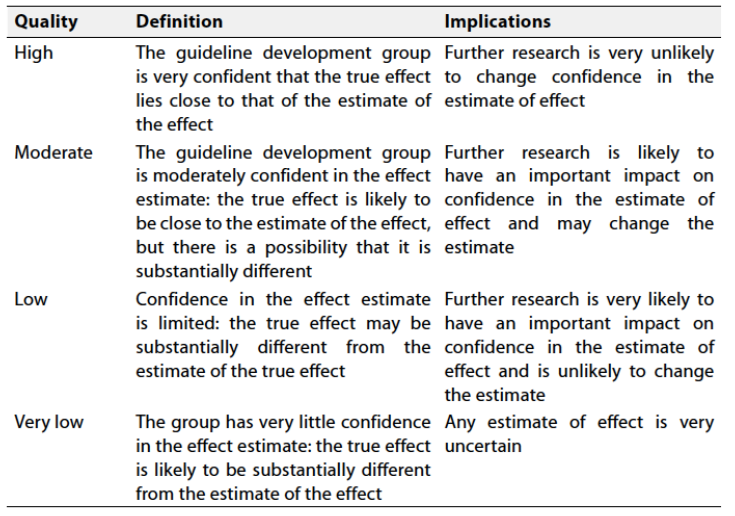
Table 3: Factors that determine How to upgrade or downgrade the quality of Evidence
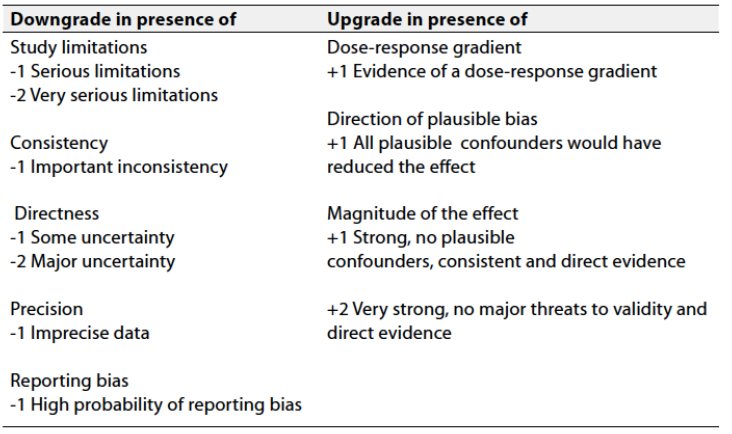
➡️The strength of the recommendation:
The strength of a recommendation communicates the importance of adherence to the recommendation.
➡️Strong recommendations:
With strong recommendations, the guideline communicates the message that the desirable effects of adherence to the recommendation outweigh the undesirable effects. This means that in most situations the recommendation can be adopted as policy.
➡️Conditional recommendations
These are made when there is greater uncertainty about the four factors above or if local adaptation has to account for a greater variety in values and preferences, or when resource use makes the intervention suitable for some, but not for other locations. This means that there is a need for substantial debate and involvement of stakeholders before this recommendation can be adopted as policy.
➡️When not to make recommendations
When there is lack of evidence on the effectiveness of an intervention, it may be appropriate not to make a recommendation.
- References
1. Konar SK, Shukla D, Agrawal A. Posttraumatic brain edema: Pathophysiology, management, and current concept. Apollo Medicine. 2019 Jan 1;16(1):2-7.
2. Robba C, Iannuzzi F, Taccone FS. Tier-three therapies for refractory intracranial hypertension in adult head trauma. Minerva Anestesiologica. 2021 Aug 2;87(12):1359-66.
3. Zusman BE, Kochanek PM, Jha RM. Cerebral Edema in Traumatic Brain Injury: a Historical Framework for Current Therapy. Curr Treat Options Neurol. 2020 Mar;22(3):9
4. Iqbal, U., Kumar, A., Arsal, S.A. et al. Efficacy of hypertonic saline and mannitol in patients with traumatic brain injury and cerebral edema: a systematic review and meta-analysis. Egypt J Neurosurg 38, 54 (2023).
5. Berger-Pelleiter E, Émond M, Lauzier F, Shields JF, Turgeon AF. Hypertonic saline in severe traumatic brain injury: a systematic review and meta-analysis of randomized controlled trials. Canadian Journal of Emergency Medicine. 2016 Mar;18(2):112-20.
6. Guidelines for the Management of Severe Traumatic Brain Injury 4th Edition: Brain Trauma Foundation: September 2016.
7. Cook, A.M., Morgan Jones, G., Hawryluk, G.W.J. et al. Guidelines for the Acute Treatment of Cerebral Edema in Neurocritical Care Patients. Neurocrit Care 32, 647–666 (2020).
8. Greenberg’s Handbook of Neurosurgery, Tenth Edition.
9. Hawryluk GW, Rubiano AM, Totten AM, O’Reilly C, Ullman JS, Bratton SL, Chesnut R, Harris OA, Kissoon N, Shutter L, Tasker RC. Guidelines for the management of severe traumatic brain injury: 2020 update of the decompressive craniectomy recommendations. Neurosurgery. 2020 Sep;87(3):427.
10. Chandra VR, Prasad BC, Banavath HN, Reddy KC. Cisternostomy versus decompressive craniectomy for the management of traumatic brain injury: a randomized controlled trial. World Neurosurgery. 2022 Jun 1;162: e58-64.