Fluoride for adults
| Site: | EHC | Egyptian Health Council |
| Course: | Conservative Dentistry Guidelines |
| Book: | Fluoride for adults |
| Printed by: | Guest user |
| Date: | Wednesday, 6 May 2026, 12:52 AM |
Description
"last update: 19 May 2025 Download Guideline
- Executive Summary
This guideline offers evidence-based recommendations on fluoride application for prevention of dental caries in adults. The recommendations are intended to provide healthcare professionals with practical guidance for using fluoride formulations for preventing dental caries in adults.
- Recommendations
➡️For coronal caries prevention in adults older than 18:
· Apply 2.26 % fluoride varnish years at least every three to six months for adults at risk of developing dental caries in a clinical setting.
(Conditional recommendation, low certainty evidence 5,6)
· Apply 1.23 % acidulated phosphate fluoride (APF) gel for four minutes at least every three to six months in a clinical setting.
(Conditional recommendation, low certainty evidence7-9)
· Apply home-use 0.09 % fluoride mouthrinse at least weekly.
(Good practice statement)
· Apply home-use 0.5 % fluoride gel or paste twice daily.
(Good practice statement)
➡️For root caries prevention in adults:
· Apply 2.26 % fluoride varnish at least every three to six months in a clinical setting.
(Conditional recommendation, low certainty evidence7-9)
· Apply 1.23 % acidulated phosphate fluoride (APF) gel for four minutes at least every three to six months in a clinical setting.
(Good practice statement)
· Apply home-use 0.09 % fluoride mouthrinse daily.
(Good practice statement)
· Apply home-use 0.5 % fluoride gel or paste twice daily.
(Good practice statement)
➡️Remarks: Adults with a history of frequent caries or those with reduced salivary flow should consider application of 2.26% fluoride varnish or 1.23% acidulated phosphate fluoride (APF) gel in a clinical setting or using prescription-strength fluoride products at home, such as 0.5% fluoride gel or paste and 0.09% fluoride mouthrinse. The recommendations for adults are based on expert opinion due to the lack of direct evidence specifically for this age group. Therefore, the panel judged that the benefits of these fluoride applications outweigh the potential for harm. However, these recommendations should be integrated with the practitioner's professional judgment and the patient's needs and preferences.
➡️Summary of evidence: Evidence supports the efficacy of fluoride gel in reducing caries in adults with history of caries or high caries risk. Clinical trials have shown that fluoride varnish significantly reduces the incidence of dental caries in adults, particularly those with root caries or high caries risk.5, 6 Evidence from studies on children and adolescents suggests a benefit of Acidulated Phosphate Fluoride gel (1.23% APF) application twice per year for four minutes.7-9 The panel extrapolated these findings to adults in preventing both coronal and root caries. Regarding the use of prescription-strength fluoride products at home, such as 0.5% fluoride gel or paste and 0.09% fluoride mouthrinse; limited studies have demonstrated the effectiveness of these products in high-risk adult populations or adults with exposed root surfaces, but studies in younger populations and expert opinion support their use.
➡️Rationale for the recommendation: Professionally applied fluoride varnish provides a high concentration of fluoride directly to the teeth, enhancing remineralization and inhibiting demineralization, which is especially beneficial for adults with exposed root surfaces.4 In addition, professional application of fluoride gel ensures a controlled and concentrated dose of fluoride, which can be particularly beneficial for adults with a history of caries or those undergoing orthodontic treatment. Home-use fluoride products allow for regular, sustained exposure to fluoride, which is crucial for ongoing caries prevention, especially in adults with exposed root surfaces or with higher caries risk due to factors like dry mouth or previous dental work.
- Acknowledgement
We would like to acknowledge the Conservative Dentistry Scientific Committee for developing these guidelines.
Chair of the GDG: Randa ElSalawy, School of Dentistry, Newgiza University
Members of the Guideline Development Group (GDG):
Dr Randa Elsalawy Professor and Dean of school
of dentistry New Giza University Dr Karim Albattoty professor and Dean of
school of dentistry Ain Shams University
Dr Ahmed Emad Fayyad, Professor at faculty of dentistry Cairo University
Dr Ahmed El Zohairy, Professor at faculty of dentistry Cairo University
Dr Osama Elshahawy, Professor at faculty of dentistry Cairo University
Dr Foad Sharaby, Professor at faculty of dentistry Cairo University
Dr Mohamed Khalifa Zayet, Professor at faculty of dentistry Cairo University
Dr Mohamed Ahmed Alsholkamy, Professor at Suiz Canal University
Dr Mohamed Tarek Alhalawany, Lecturer at Elalameen University
Dr Hussein Abdelhady, Lecturer at Minia University
Dr Ahmed Amin Musselhy, Associate professor at the Military Medical Academy
Dr Rafik Kamal Gerges Associate professor, at the Military Medical Academy
Dr Omar Shaalan, Associat professor, Faculty of Dentistry, Cairo University
Dr Marwa AbdelHafez, School of Dentistry, Newgiza University, Cairo
- Abbreviations
ADA
American Dental Association
APF
Acidulated phosphate fluoride
CSA
Council on Scientific Affairs
- Introduction
Dental caries is one of the most frequent chronic diseases affecting people all over the world, and it can develop at any age. Dental caries emerges over time as a result of a complex interplay between acid-producing bacteria, fermentable carbohydrates, and host factors such as teeth and saliva.2 The application of fluoride in preventing caries has been shown to be a beneficial public health intervention, and it is considered as one of the twentieth century's top ten successes. Fluoride found in toothpaste, mouthwashes, varnishes, gels, foams, and prophylaxis paste minimizes enamel demineralization, enhances remineralization, and prevents microorganisms in dental plaque from utilizing sugar.3
- Scope and Purpose
➡️The objectives of the present guidelines are:
· To provide guidance on professionally applied topical fluorides for caries prevention in adults.
· To provide guidance for using prescription-strength, home-use topical fluorides for caries prevention in adults.
- Target Audience
This guideline targets; healthcare professionals, policy makers, as well as non-governmental organizations (NGOs) and other stakeholders to afford the most appropriate prevention measures for individuals at risk to develop dental caries.
- Methodology
A comprehensive search for guidelines was undertaken to identify the most relevant guidelines to consider for adaptation.
Inclusion/ exclusion criteria followed in the search and retrieval of guidelines to be adapted:
• Selecting only evidence-based guidelines (guideline must include a report on systematic literature searches and explicit links between individual recommendations and their supporting evidence).
• Selecting only national and/or international guidelines.
• Specific range of dates for publication (using Guidelines published or updated in 2015 and later).
• Selecting peer reviewed publications only
• Selecting guidelines written in English language
• Excluding guidelines written by a single author, not on behalf of an organization to be valid and comprehensive, a guideline ideally requires multidisciplinary input.
• Excluding guidelines published without references as the panel needs to know whether a thorough literature review was conducted and whether current evidence was used in the preparation of the recommendations.
The following characteristics of the retrieved guidelines were summarized in:
• Developing organization/authors
• Date of publication, posting, and release
• Country/language of publication
• Date of posting and/or release
• Dates of the search used by the source guideline developers.
All retrieved Guidelines were screened and appraised using AGREE II instrument (www.agreetrust.org) by at least three members. The panel decided on a cut-off point or ranked the guidelines (any guideline scoring above 50% on the rigor dimension was retained). The GDG decided to adapt the American Dental Association (ADA) guidelines on professionally applied and prescription-strength, home-use topical fluoride agents for caries prevention – 2013.4
➡️Evidence assessment
According to WHO Handbook for Guidelines, we used the GRADE (Grading of Recommendations, Assessment, Development and Evaluation) approach to assess the quality of a body of evidence, develop and report recommendations. GRADE methods are used by WHO because these represent internationally agreed standards for making transparent recommendations. Detailed GRADE information is available on the following site:
https://www.gradeworkinggroup.org/
Table 1 Quality and Significance of the four levels of evidence in GRADE:
|
Quality |
Definition
|
Implications |
|
High |
The guideline development group is very confident that the true effect lies close to that of the estimate of the effect. |
Further research is very unlikely to change confidence in the estimate of effect |
|
Moderate |
The guideline development group is moderately confident in the effect estimate: the true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different |
Further research is likely to have an important impact on confidence in the estimate of effect and may change the estimate |
|
Low |
Confidence in the effect estimate is limited: the true effect may be substantially different from the estimate of the true effect |
Further research is very likely to have an important impact on confidence in the estimate of effect and is unlikely to change the estimate |
|
Very Low |
The group has very little confidence in the effect estimate: the true effect is likely to be substantially different from the estimate of the effect. |
Any estimate of effect is very uncertain |
Table 2: Factors that determine How to upgrade or downgrade the quality of evidence:
|
Downgrade in presence of |
Upgrade in presence of |
|
Study limitations -1 Serious limitations -2 Very serious limitations Consistency -1 Important inconsistency Directness -1 Some uncertainty -2 Major uncertainty Precision -1 Imprecise data Reporting bias -1 High probability of reporting bias |
Dose-response gradient +1 Evidence of a dose-response gradient Direction of plausible bias +1 All plausible confounders would have reduced the effect Magnitude of the effect +1 Strong, no plausible confounders, consistent and direct evidence +2 Very strong, no major threats to validity and direct evidence |
➡️The strength of recommendations:
The strength of a recommendation communicates the importance of adherence to the recommendation.
➡️Strong recommendations
With strong recommendations, the guideline communicates the message that the desirable effects of adherence to the recommendation outweigh the undesirable effects. This means that in most situations the recommendation can be adopted as policy.
➡️Conditional recommendations
These are made when there is greater uncertainty about the four factors above or if local adaptation has to account for a greater variety in values and preferences, or when resource use makes the intervention suitable for some, but not for other locations. This means that there is a need for substantial debate and involvement of stakeholders before this recommendation can be adopted as policy.
➡️Good practice recommendations:
Clinical opinion suggests this advice is well established or supported. No robust underpinning research evidence exists. Good practice points are primarily based on extrapolation from research on related topics and/or clinical consensus, expert opinion and precedent, and not on research appropriate for rating the certainty or quality of the evidence.
➡️When not to make recommendations:
When there is lack of evidence on the effectiveness of an intervention, it may be appropriate not to make a recommendation.
- Research needs
Multiple well designed, appropriately powered, placebo-controlled randomized trials that follow the Consolidated Standards of Reporting Trials16 (CONSORT) guidelines with standardized reporting according to age, dentition and caries risk status should be conducted in Egypt. Standard methodologies for caries and fluoride randomized controlled trials should be developed. Future trials should be registered with ClinicalTrials.gov or equivalent registries. Specific areas of research recommendations are as follows:
· Determining of the mechanism of action and caries-preventive effects of various topical fluorides when in use at the current level of background fluoride exposure (fluoridated water and fluoride toothpaste).
· Evaluation of fluoride in arresting or reversal of caries progression.
· Comparative effectiveness of different fluoride strategies in high-risk populations, including: adults aged 18 through 65 years, adults older than 65 (including those living in long-term care facilities), adults who are at extremely high risk of developing caries, special needs populations (cognitive disabilities, compromised self-care abilities or physical disabilities) and populations with chronic diseases (such as Sjögren syndrome).
· Comparative effectiveness of different strategies to manage xerostomia-induced coronal and root caries.
· Evaluation of the effectiveness and risks of specific products in the following areas: self-applied, prescription-strength, home-use fluoride gels, toothpastes or drops; 2% professionally applied sodium fluoride gel; alternative delivery systems, such as foam; optimal application frequencies for fluoride varnish and gels; one-minute applications of APF gel; and combinations of products (home-use and professionally applied).
· Evaluation of caries arrest and reversal using different measures.
· Effectiveness and economic benefit of using topical fluoride in caries prevention of different caries risk populations.
· Incorporation of clinical recommendations of using fluoride into practice.
➡️Monitoring and evaluating the impact of the guidelines:
· Fluoride Treatment Coverage: Percentage of patients receiving fluoride varnish or treatment during visits.
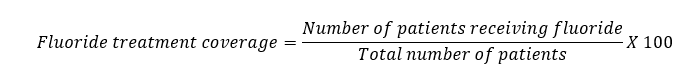
· Caries Prevention Rate Post-Fluoride: Percentage reduction in new caries development in patients treated with fluoride over a defined period.
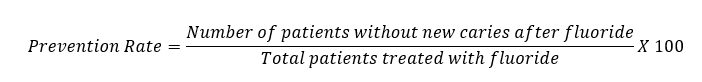
· Reduction in DMFT Index Post-Fluoride: Change in Decayed, Missing, and Filled Teeth (DMFT) index in patients who received fluoride treatment.

· Cost-Effectiveness of Fluoride Programs: Cost per case of dental caries prevented due to fluoride interventions.
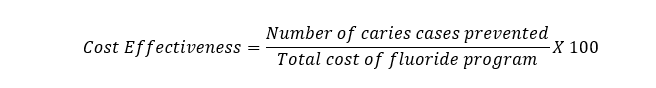
- Updating the guidelines
These guidelines will be updated whenever there is new evidence.
Adapted from ADA “Professionally Applied and Prescription-Strength, Home-Use Topical Fluoride Agents for Caries Prevention Clinical Practice Guideline ” 2013
- References
1. Walsh T, Macey R, Ricketts D, Carrasco Labra A, Worthington H, Sutton AJ, et al. Enamel Caries Detection and Diagnosis: An Analysis of Systematic Reviews. J Dent Res. 2022;101(3):261-9.
2. Selwitz RH, Ismail AI, Pitts NB. Dental caries. The Lancet. 2007;369(9555):51-9.
3. Šket T, Kukec A, Artnik B. The history of public health use of fluorides in caries prevention. Slovenian Journal of Public Health. 2017;56(2):140-6.
4. Weyant RJ, Tracy SL, Anselmo T, Beltrán-Aguilar ED, Donly KJ, Frese WA, et al. Topical fluoride for caries prevention. The Journal of the American Dental Association. 2013;144(11):1279-91.
5. Johnston DW, Lewis DW. Three-Year Randomized Trial of Professionally Applied Topical Fluoride Gel Comparing Annual and Biannual Applications with/without Prior Prophylaxis. Caries Research. 2009;29(5):331-6.
6. Ripa LW, Leske GS, Sposato A, Varma A. Effect of Prior Toothcleaning on Bi-Annual Professional Acidulated Phosphate Fluoride Topical Fluoride Gel-Tray Treatments: Results after Three Years. Caries Research. 2009;18(5):457-64.
7. Olivier M, Brodeur JM, Simard PL. Efficacy of APF treatments without prior tooth cleaning targeted to high‐risk children. Community Dentistry and Oral Epidemiology. 1992;20(1):38-42.
8. Cobb HB, Rozier RG, Bawden JW. A clinical study of the caries preventive effects of an APF solution and APF thixotropic gel. Pediatr Dent. 1980;2(4):263-6.
9. Agrawal N, Pushpanjali K. Feasibility of including APF gel application in a school oral health promotion program as a caries-preventive agent: a community intervention trial. Journal of oral science. 2011;53(2):185-91.
10. Seppä L, Hausen H, Pöllänen L, Kärkkäinen S, Helasharju K. Effect of intensified caries prevention on approximal caries in adolescents with high caries risk. Caries Research. 1991;25(5):392-5.
11. Hausen H, Kärkkäinen S, Seppä L. Application of the high‐risk strategy to control dental caries. Community Dentistry and Oral Epidemiology. 2000;28(1):26-34.
12. Weyant RJ, Tracy SL, Anselmo TT, Beltran-Aguilar ED, Donly KJ, Frese WA, et al. Topical fluoride for caries prevention: executive summary of the updated clinical recommendations and supporting systematic review. J Am Dent Assoc. 2013;144(11):1279-91.
13. Aminabadi NA, Balaei E, Pouralibaba F. The effect of 0.2% sodium fluoride mouthwash in prevention of dental caries according to the DMFT index. Journal of dental research, dental clinics, dental prospects. 2007;1(2):71.
14. Augenstein WL, Spoerke DG, Kulig KW, Hall AH, Hall PK, Riggs BS, et al. Fluoride ingestion in children: a review of 87 cases. Pediatrics. 1991;88(5):907-12.
15. Beltrán-Aguilar ED, Goldstein JW, Lockwood SA. Fluoride varnishes: a review of their clinical use, cariostatic mechanism, efficacy and safety. The Journal of the American Dental Association. 2000;131(5):589-96.
16. Schulz KF, Altman DG, Moher D, Group* C. CONSORT 2010 statement: updated guidelines for reporting parallel group randomized trials. Annals of internal medicine. 2010;152(11):726-32.