Traumatic disease in cattle
| Site: | EHC | Egyptian Health Council |
| Course: | Large ruminant Medicine and surgery Guidelines |
| Book: | Traumatic disease in cattle |
| Printed by: | Guest user |
| Date: | Wednesday, 6 May 2026, 12:52 AM |
Description
"last update: 7 December 2025" Download Guideline
- Acknowledgement
We would like to acknowledge the committee of National Egyptian Guidelines for Veterinary Medical Interventions, Egyptian Health Council for adapting this guideline.
Executive Chief of the Egyptian Health Council: Prof. Dr Mohamed Mustafa Lotief.
Head of the Committee: Prof. Dr Ahmed M Byomi
The rapporteur of the Committee: Prof. Dr Mohamed Mohamedy Ghanem.
Scientific Group Members: Prof. Nabil Yassien, Prof. Ashraf Aly Eldesoky Shamaa, Prof. Amany Abbas, Prof. Dalia Mansour, Essam Sobhy Mohamed Elsharkawy, Prof. Gamal A. Sosa., Dr Naglaa Radwan, Dr Hend El Sheikh
Author: Prof. Mohamed Ghanem
- Traumatic Pericarditis in Cattle
1. Introduction
Traumatic pericarditis is a serious condition commonly observed in adult cattle, especially dairy cows, resulting from the migration of a foreign object from the reticulum through the diaphragm into the pericardial sac. The resulting infection and inflammation impair heart function and may be fatal if not promptly treated. It is part of a broader condition known as traumatic reticuloperitonitis (TRP).
2. Etiology
- Primary cause: Ingestion of metallic foreign objects such as nails, wires, needles..
- Cattle are indiscriminate eaters and often ingest foreign materials while consuming hay or silage contaminated with metal debris.
- The object typically settles in the reticulum due to its weight and the hexagonal folds of reticular mucosa.
- With reticulorumen contractions, the object may penetrate:
- The reticulum wall
- The peritoneum
- The diaphragm
- The pericardium
3. Pathogenesis
1. Ingested metallic foreign body reaches the reticulum.
2. Reticular contractions push the object through the reticulum wall and peritoneum.
3. The object may:
▪️ Perforate the diaphragm
▪️ Enter the pericardial sac, leading to:
- Fibrinous pericarditis
- Purulent pericarditis
- Cardiac tamponade (pressure on heart due to accumulation of fluids in pericardium)
- Extension to pleura or lungs causing pleuropneumonia
4. Inflammatory exudate in pericardial sac leads to cardiac dysfunction, reduced cardiac output, and right heart failure.
4. Clinical Signs
Acute Stage:
- Fever (up to 41°C)
- Anorexia, milk drop
- Painful expression, grunting
- Abduction of elbows
- Arched back, reluctance to move
- Positive withers pinch test and pole test
- Tachycardia, muffled heart sounds
- Pericardial friction rubs (early), then splashing or washing machine sounds
- Jugular distension, brisket edema
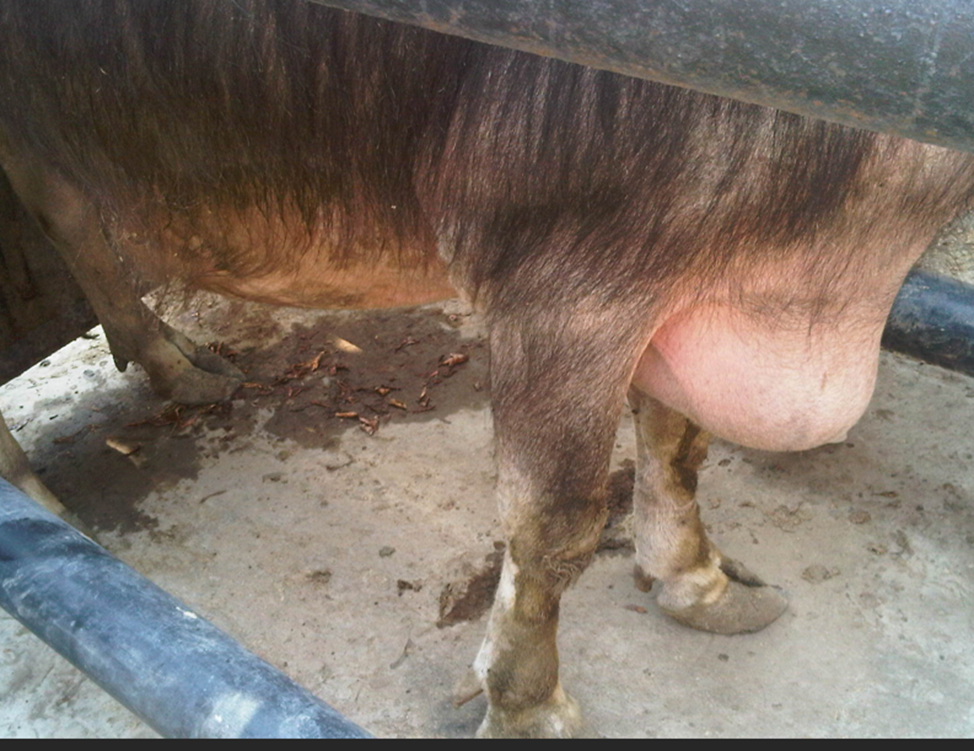
Ventral edema and abduction of forelimb in a cow with TRP and TP
Chronic Stage:
- Emaciation, chronic weight loss
- Pale mucous membranes
- Ascites, edema of ventral body parts
- Laboured breathing
5. Diagnosis
Clinical Diagnosis:
- Characteristic posture and pain responses (pain test)
- Signs of cardiac involvement (brisket edema, jugular distension and pulsation)
- Use of Mine detector
Laboratory Diagnosis:
- Leukocytosis with a left shift
- Elevated fibrinogen and total protein
- Anemia at chronic stages
Imaging:
- Ultrasonography:
- Pericardial fluid
- Fibrin strands in pericardium
- Radiography:
- Metallic foreign body in reticulum
- Diaphragmatic penetration
6. Differential Diagnoses
- Endocarditis
- Simple TRP (traumatic reticuloperitonitis without cardiac involvement)
- Congestive heart failure from other causes
- Pleuropneumonia
7. Treatment
Medical Management:
- Oral magnet (if not already given) to trap metallic objects
- Long-acting antibiotics:
- Penicillin
- Oxytetracycline
- NSAIDs (e.g., flunixin, ketoprofen)
- Diuretics in cases of fluid accumulation
- Pericardiocentesis: to relieve pressure (rare in field settings)
- Keep the animals feeding with fore limbs at upper level
Surgical interference:
- Left-flank rumenotomy to remove foreign body from reticulum
- Pericardial drainage
8. Prognosis
- Guarded to poor in most cases, especially if heart failure signs are evident.
- Prognosis is better if diagnosed early and treated before cardiac tamponade develops.
- Most cases with brisket edema or extensive fibrinous pericarditis do not recover.
9. Prevention
- Prophylactic oral magnets for all replacement heifers and adult cattle
- Use of magnets in feed processing equipment
- Avoid feeding contaminated feed (baled hay with scrap metal or fencing)
- Proper disposal of metal materials in cattle areas
- Regular inspection of feedlots and pastures
- Vagal indigestion (Hoflund syndrome) in cattle
1. Overview & Historical Context
Vagal indigestion, also termed Hoflund syndrome, refers to a functional motility disorder in ruminants characterized by impaired transit through the fore‑stomachs and/or abomasum—not always caused by direct injury to the vagus nerve itself. Vagal indigestion in cattle is a multifactorial syndrome involving functional obstruction of fore stomach or abomasal outflow, often secondary to STEERING conditions like traumatic reticuloperitonitis or abscesses rather than primary nerve damage.
Types of vagal indigestions
Originally described by Sven Hoflund in the 1940s, it was historically classified into Types I–IV. As follow:
1. Type I (failure of eructation), causing gas bloat and ruminal distension.
2. Type II (failure of omasal transport), leading to ingesta accumulation and a distended rumen
3. Type III (failure of pyloric flow), resulting in abomasal and omasal distension from ingesta accumulation.
4. Type IV (external compression), typically seen in late pregnancy when a uterus compresses the forestomach.
Functionally vagal indigestion is categorized as:
- Proximal (anterior) functional stenosis: at the reticulo‑omasal orifice
- Distal (posterior) functional stenosis: at the abomasum–pylorus outlet
Etiology & Pathogenesis
A. Vagal Nerve Involvement vs. Functional Obstruction
- Traditional thinking emphasized vagal nerve damage, often due to traumatic reticuloperitonitis (“hardware disease”)
- However, more recent research shows mechanical inhibition (adhesions, abscesses, neoplasia) frequently underlies motility failure, even without direct nerve injury (
B. Common Predisposing Factors
- Traumatic reticuloperitonitis (TRP) → inflammation, adhesions secondary to puncture
- Liver/perihepatic abscesses, lymphosarcoma, abomasal ulcers, gastric impaction (
- Post‑surgical complications, especially after correction of displaced abomasum (RDA/AVV)—can lead to VI within ~5 days post-op due to peritonitis or nerve injury
Prevalence and Types
• Vagal indigestion accounts for approximately 5.5% of digestive cases in cattle, with Type II being the most common, representing 40% of cases
• Other types include Type I (24.3%), Type III (18.6%), and Type IV (10%)
Clinical Signs & Diagnostic Findings
A. Clinical Presentation
Common findings include:
- Progressive, chronic abdominal distension, often with the characteristic “papple” shape: apple‑shaped on the left, pear‑shaped on the right
- Ruminal distension with soft or liquid contents; may be accompanied by free‑gas bloat in Type I.
- Reduced appetite, weight loss, decreased fecal output, sporadic or foul diarrhea, decreased milk production, bradycardia, and dehydration .
B. Laboratory/Diagnostic Data
- Rumen chloride concentration: elevated (>30 mEq/L) in distal (post‑pyloric) forms
- CBC may show neutrophilia, left shift (in abscess/peritonitis cases)
- Ultrasonography: reticular motility significantly reduced in distal cases vs proximal; contraction frequency averages differ (proximal ~4.6/3 min, distal ~3.6/3 min) (
Imaging & Ultrasonographic Evaluation
Ultrasound is a key diagnostic tool:
- Evaluates reticular contractile patterns, motility, and signs of abscesses or adhesions.
- In perihepatic abscess cases: visualization of echogenic capsules with heterogeneous content between rumen, reticulum and thoracic wall
- Ultrasonography quantified motility and helped distinguish proximal vs distal functional stenosis (
Treatment & Prognosis
A. Treatment Strategies
- Type I (free‑gas bloat): release gas via stomach tube or rumen fistula; remove esophageal obstruction if present
- Type II/III (omasal transport or abomasal emptying failure): supportive care (fluids, electrolytes, mineral oil, rumen cathartics, calcium supplements); surgical exploration (left paralumbar rumenotomy, possible abomasotomy) in advanced cases (
- Abscess-related vs neoplastic vs TRP etiologies: drainage or surgical resection if feasible; antimicrobial therapy essential if peritonitis is present (e.g., after RDA correction)
Prognosis
- Generally poor if the underlying cause is not confirmed or treatable.
- Prognosis improves slightly if specific causes (e.g. TRP, abscess) are identified early and treated; however retrospective studies report ~80% poor outcomes
- References
- Radostits, O.M., et al. Veterinary Medicine, 10th Edition.
- Smith, B.P. Large Animal Internal Medicine, 6th Edition.
- Andrews, A. H., Blowey, R. W., Boyd, H., Eddy, R. G. Bovine Medicine.
4. Soares, G. S. L., Afonso, J. A. B., Souto, R. J. C., Cajueiro, J. F. de P., Conceição, Ângela I. da, Ribeiro, A. C. S., … Mendonça, C. L. de. (2022). Vagal indigestion in cattle: a retrospective study. Semina: Ciências Agrárias, 43(6), 2579–2594. https://doi.org/10.5433/1679-0359.2022v43n6p2579