Metabolic disorders in cattle
| Site: | EHC | Egyptian Health Council |
| Course: | Large ruminant Medicine and surgery Guidelines |
| Book: | Metabolic disorders in cattle |
| Printed by: | Guest user |
| Date: | Wednesday, 6 May 2026, 12:53 AM |
Description
"last update: 12 April 2026" Download Guideline
Table of contents
- - Acknowledgment
- - Introduction
- - Classifications of metabolic diseases
- - Definition of milk fever
- - Etiology of milk fever
- - Pathogenesis of milk fever
- - Clinical Signs of milk fever
- - Diagnosis of milk fever
- - Treatment in milk fever
- - Prevention of milk fever
- - Complications of milk fever
- - Differential Diagnosis for milk fever
- - Prognosis of milk fever
- - References
- Acknowledgment
We would like to acknowledge the committee of the National Egyptian Guidelines for Veterinary Medical Interventions, Egyptian Health Council for adapting this guideline.
Executive Chief of the Egyptian Health Council: Prof. Mohamed Mustafa Lotief.
Head of the Committee: Prof. Ahmed M Byomi
The rapporteur of the Committee: Prof. Mohamed Mohamedy Ghanem.
Scientific Group Members: Prof. Nabil Yassien, Prof. Ashraf Aldesoky Shamaa, Prof. Amany Abbas, Prof. Dalia Mansour, Dr Essam Sobhy Dr Mohamed Elsharkawy, Prof. Dr Gamal A. Sosa., Dr Naglaa Radwan, Dr Hend El Sheikh
Editor/Author: Prof. Mohamed Ghanem
- Introduction
Metabolic disorders in cattle represent a significant challenge to global livestock production, animal health, and farm profitability. These disorders commonly arise when nutrient intake does not match physiological demands, particularly during the transition period (three weeks pre‑ and post‑calving). They impair metabolic homeostasis, reduce productivity, and increase susceptibility to secondary diseases.
These disorders typically arise from nutritional imbalances, hormonal irregularities, or genetic predispositions. They are called “production diseases “because of its relation to high milk production in cattle.
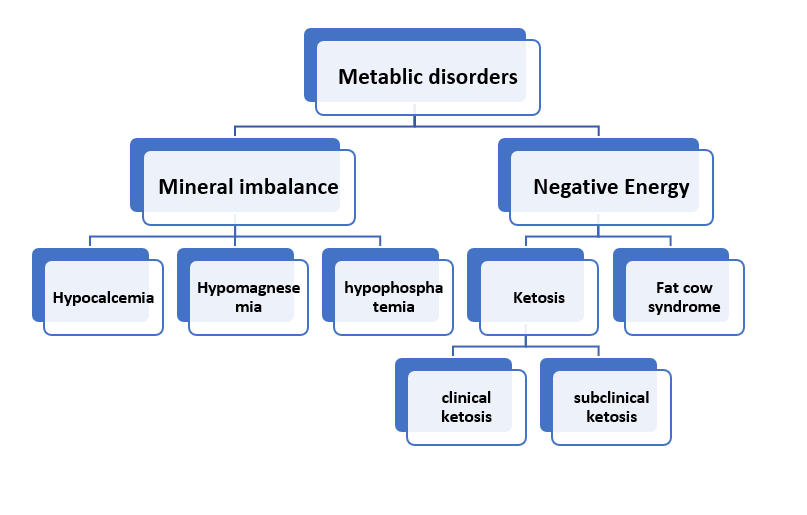
- Classifications of metabolic diseases
|
Category |
Etiology |
Disease name |
|
Mineral imbalance |
Hypocalcemia |
Milk fever |
|
Hypomagnesemia |
Lactation tetany |
|
|
hypophosphatemia |
Post-parturient VBNM12hemoglobinuria |
|
|
Negative energy balance (carbohydrate) |
Hypoglycemia |
Ketosis |
|
Fatty liver |
Fat cow syndrome |
|
|
Downer cow syndrome |
Metabolic or traumatic |
|
- Definition of milk fever
Milk fever (parturient paresis) is a metabolic disease of dairy cattle characterized by low blood calcium levels (hypocalcemia) occurring around parturition, usually within 24–72 hours after calving, due to the sudden demand for calcium for colostrum and milk production.
It mainly affects high-producing multiparous dairy cows, especially Jersey and Holstein breeds.
- Etiology of milk fever
Milk fever occurs when calcium homeostasis mechanisms fail to respond quickly to the sudden calcium drain into milk.
Main causes:
1. Sudden calcium demand at parturition
2. Reduced calcium mobilization from bone
3. Insufficient intestinal calcium absorption
4. Improper dry cow nutrition
Predisposing factors:
- High milk production
- Older cows (3rd lactation and above)
- High calcium diet during dry period
- Low magnesium levels
- Metabolic alkalosis
- Lack of exercise
- Obesity
- Breed susceptibility (Jersey > Holstein)
- Pathogenesis of milk fever
At calving:
- Large amounts of calcium are removed in colostrum
- Blood calcium drops rapidly
Normally the body responds through:
- Increased Parathyroid hormone (PTH) → mobilizes calcium from bone
- Increased Vitamin D activation → increases gut absorption of calcium
- Increased renal calcium reabsorption
In milk fever:
- Tissue response to PTH is delayed
- Bone mobilization is slow
- Intestinal absorption is insufficient
Result:
Serum calcium drops below 5–7 mg/dl (normal 8-10 mg/dl)
Calcium is activator of acetylcholine which is essential mediator at the neuromuscular junction enhancing muscular contractility, therefore decreased Ca level causes:
- Neuromuscular dysfunction
- Muscle weakness
- Paresis
- Reduced smooth muscle contraction
- Clinical Signs of milk fever
Milk fever occurs in three stages:
Stage 1 (Early stage) – Excitement stage
Duration: short (often missed). clinical signs include:
- Restlessness
- Hypersensitivity
- Muscle tremors
- Ear twitching
- Mild weakness
Stage 2 (Sternal recumbency stage)
Is the most commonly observed stage. Clinical Signs:
- Sternal recumbency
- Depression
- Cold ears and muzzle
- Dilated pupils
- Reduced rumen motility
- Constipation
- Tachycardia (weak pulse)
- Body temperature may be normal or low
- Characteristic S-shaped neck

Figure (1): sternal recumbency in a cow with milk fever.
Stage 3 (Lateral recumbency stage - comatosed)
Severe stage (emergency): signs include:
- Lateral recumbency
- Severe depression
- Coma
- Bloat
- Severe hypothermia (cold ears and extremities)
- Weak heart sounds
- Death if untreated
- Diagnosis of milk fever
Clinical diagnosis:
- History at late pregnancy or recently calved cow
- Recumbency (sternal then lateral)
- Cold extremities
- Good response to calcium therapy (therapeutic diagnosis)
Laboratory diagnosis:
- Low serum calcium
- There may be hypophosphatemia, mild hyperglycemia
- Increased CK due to muscle damage
- Treatment in milk fever
Milk fever is considered as a medical emergency.
Primary treatment:
IV Calcium therapy: Calcium borogluconate - or Cal-D-Mag (25%)
- 500 ml slowly IV
- Given over 10–20 minutes
Response:
- Improvement within minutes
- Eructation
- Urination
- Standing within 1–2 hours
- If no response, repeat ca therapy after 12 hrs.
Additional therapy:
- Subcutaneous calcium (to prevent relapse)
- Oral calcium gels
- Phosphorus supplementation if needed
- Magnesium if hypomagnesemia is suspected
Important precautions for calcium therapy in cattle:
- Give slowly (risk of cardiac arrhythmia)
- Monitor heart during IV infusion
- Stop if arrhythmia occurs
- Prevention of milk fever
1. Low calcium diet before calving
Low Ca diet Stimulates calcium mobilization before parturition by activating parathyroid hormone (less than 50 g Ca/day).
2. Dietary Cation Anion Difference (DCAD diet)
Use anionic salts such as Ammonium chloride, Calcium sulfate, and Magnesium sulfate (to produce pH between 6-6.5). This mild metabolic acidosis improves PTH response.
3. Vitamin D supplementation
Given before calving (use cautiously). 10 millin IU given SC of IV about 10 days before calving.
4.Magnesium supplementation: Magnesium improves calcium metabolism.
- Complications of milk fever
Milk fever predisposes cattle to the following diseases and problems:
- Dystocia
- Retained placenta
- Ketosis
- Displaced abomasum
- Mastitis
- Metritis
Reason:
Smooth muscle weakness and immune suppression.
- Differential Diagnosis for milk fever
|
Disease |
Distinguishing Features |
|
Hypomagnesemia (Grass tetany) |
Excitement, convulsions, not flaccid paralysis |
|
Ketosis |
Acetone smell, normal calcium |
|
Downer cow syndrome |
Cow remains recumbent after calcium correction |
|
Mastitis |
Fever, abnormal milk |
|
Metritis |
Foul uterine discharge |
|
Botulism |
Progressive paralysis without hypocalcemia |
|
Rabies |
Aggression, neurological signs |
- Prognosis of milk fever
Good prognosis if:
- Treated early
- Cow treated within 6–12 hrs
Poor prognosis if:
- Stage 3 (comatose)
- Delayed treatment
- Muscle damage occurs
- Secondary complications
Recovery rate:
85–95% if treated early
- References
Bobe, G., Young, J. W., & Beitz, D. C. (2004). Invited review: Pathology, etiology, prevention, and treatment of fatty liver in dairy cows. Journal of Dairy Science, 87(10), 3105–3124.
Constable, P. D., Hinchcliff, K. W., Done, S. H., & Grünberg, W. (2017). Veterinary medicine: A textbook of the diseases of cattle, horses, sheep, pigs and goats (11th ed.). Elsevier.
Drackley, J. K. (1999). Biology of dairy cows during the transition period: The final frontier? Journal of Dairy Science, 82(11), 2259–2273.
Duffield, T. F. (2000). Subclinical ketosis in lactating dairy cattle. Veterinary Clinics of North America: Food Animal Practice, 16(2), 231–253.
Fares AA, Ghanem MM, El-Raof YMA, El-Attar HM, Megahed AA, El-Khaiat HM (2022). Metabolomics of periparturient Holstein-Friesian cows associated with feeding a negative dietary cation-anion difference (DCAD). Adv. Anim. Vet. Sci. 10(7):1504-1512.
Ghanem MM (2013). Comparative Study on the Clinical and Subclinical Hypomagnesemia in Calves with Evaluation of Therapeutic Response. The XX International Congress of Mediterranean Federation of Health and Production of Ruminants, Faculty of Veterinary Medicine, Assiut University, pp. 123-134.
Ghanem MM and El-Deep WM (2010) lecithin cholesterol acyltransferase (LCAT) activity as a predictor for ketosis and parturient haemoglobinuria in Egyptian water buffaloes. Research in Veterinary Science, 88(1):20-25
Ghanem, M., Fares A.; Abdel-Raof Y. M.; El-Attar H. E. (2017). Clinico-biochemical, oxidative markers and trace elements changes in cows with ketosis. Benha Veterinary Medical Journal, 33(2), 224-236
Ghanem, M.M. El-Fkhrany, S.F.b, Abd El-Raof, Y.M., El-Attar, H.M. (2012). Clinical and haematobiochemical evaluation of diarrheic neonatal buffalo calves (bubalas bubalis) with reference to antioxidant changes. Benha veterinary medical journal, 23 (2), 275-288
Ghanem, M.M., Mahmoud, M.E., Abd El-Raof, Y.M., El-Attar, H.M. (2016). Efficacy of different cow side tests for diagnosis of ketosis in lactating cows. Benha Vet Medical Journal, 31(2): 225-230.
Goff, J. P. (2006). Macromineral disorders of the transition cow. Veterinary Clinics of North America: Food Animal Practice, 22(2), 329–350. https://doi.org/10.1016/j.cvfa.2006.03.006
Goff, J. P. (2008). The monitoring, prevention, and treatment of milk fever and subclinical hypocalcemia in dairy cows. Veterinary Journal, 176(1), 50–57. https://doi.org/10.1016/j.tvjl.2007.12.020
Goff, J. P. (2014). Calcium and magnesium disorders. In B. P. Smith (Ed.), Large animal internal medicine (5th ed., pp. 1430–1445). Elsevier.
Gowda, N. K. S., Ledoux, D. R., Rottinghaus, G. E., Bermudez, A. J., & Chen, Y. C. (2004). Efficacy of antioxidant combinations in preventing hemolysis associated with hemoglobinuria. Veterinary Research Communications, 28(3), 221–232.
Grummer, R. R. (1993). Etiology of lipid-related metabolic disorders in periparturient dairy cows. Journal of Dairy Science, 76(12), 3882–3896.
Guliński P. Ketone bodies - causes and effects of their increased presence in cows' body fluids: A review. Vet World. 2021 Jun;14(6):1492-1503. doi: 10.14202/vetworld.2021.1492-1503. Epub 2021 Jun 11. PMID: 34316197; PMCID: PMC8304442.
Horst, R. L., Goff, J. P., & Reinhardt, T. A. (1997). Strategies for preventing milk fever in dairy cattle. Journal of Dairy Science, 80(7), 1269–1280. https://doi.org/10.3168/jds.S0022-0302(97)76065-4
Kavibharathy S, Sunandhadevi S, Enbavelan PA, Venkatesakumar E. Bovine ketosis: A comprehensive review on pathophysiology, diagnosis, monitoring strategies, therapeutics, and prevention in dairy cattle. Int J Vet Sci Anim Husbandry 2025;10(8S):72-82.
Kichura, T. S., Horst, R. L., Beitz, D. C., & Littledike, E. T. (1982). Relationships between phosphorus depletion and glucose metabolism in cattle. Journal of Nutrition, 112(6), 1133–1140.
Oetzel, G. R. (2007). Herd-level ketosis diagnosis and prevention in dairy cows. The Veterinary Clinics of North America—Food Animal Practice, 23(2), 379–402.
Ospina, P. A., Nydam, D. V., Stokol, T., & Overton, T. R. (2010). Evaluation of nonesterified fatty acids and β‑hydroxybutyrate in transition dairy cattle in the northeastern United States: Critical thresholds for prediction of clinical diseases. Journal of Dairy Science, 93(2), 546–554.
Peek, S. F., & Divers, T. J. (2018). Rebhun's diseases of dairy cattle (3rd ed.). Elsevier.
Simões, J., Lei, M.C., Stilwell, G. (2025). Downer Cow Syndrome. In: Simões, J. (eds) Encyclopedia of Livestock Medicine for Large Animal and Poultry Production. Springer, Cham. https://doi.org/10.1007/978-3-031-52133-1_317-1
Smith, B. I., & Hogan, J. S. (2006). The role of the immune system in mastitis and ketosis interactions. Veterinary Immunology and Immunopathology, 111(2), 195–204.
Smith, B. P. (2014). Large animal internal medicine (5th ed.). Elsevier.
Suttle, N. F. (2010). Mineral nutrition of livestock (4th ed.). CABI Publishing.
Underwood, E. J., & Suttle, N. F. (1999). The mineral nutrition of livestock (3rd ed.). CABI Publishing.
van Knegsel, A. T., van den Brand, H., Dijkstra, J., Tamminga, S., & Kemp, B. (2005). Effects of dietary energy source on energy balance and ketosis incidence in dairy cows. Journal of Dairy Science, 88(6), 2090–2096.
Van Saun, R. J. (2000). Metabolic profiling and health risk in transition cows. Veterinary Clinics of North America: Food Animal Practice, 16(2), 239–272.