
- GENERAL ANAESTHESIA
Definition:
It is a state of unconsciousness accompanied with hyporeflexia, analgesia and muscle relaxation. It is produced by administration of drugs having selective and reversible depression of the central nervous system.
Classification:
General anaesthesia is classified according to the rout of administration of the anaesthetic drugs into:
1- Intravenous general anaesthesia
2- Inhalation anaesthesia
3- Combination of intravenous and inhalation anaesthesia i.e. induction with intravenous and maintenance by inhalation.
Intravenous General Anaesthesia
Indications:
1- For induction of anaesthesia
2- As a sole anaesthetic agent for short term minor procedures.
Advantages:
1- Simple
2- Rapid onset
3- Relatively pleasant for animal
4- No apparatus needed
5- No explosion / pollution hazard
6- Non-irritant to airways.
Disadvantages:
1- Superficial vein may be difficult to find.
2- Animal may struggle.
3- Drug may be irritant if given perivascular.
4- Once injected it cannot be removed.
5- Drug may be cumulative
6- If the animal is not intubated, you are not ready for a respiratory emergency
7- Possible apnea on injection.
Intravenous anaesthetic drugs (Classes of drugs):
1-Barbiturates.
a- Thiopentone sodium
b- Methohexitone sodium
c- Pentobarbitone sodium
2- Propofol
3-Dissociative agents
Dogs
- Only licensed for use in combination with xylazine
- Ketamine (10 mg/kg) / Xylazine (1 mg/kg)
- Ketamine (5 mg/kg) / Diazepam (0.1 mg/kg)
Cats:
- Ketamine alone in a dose of 10-20 mg/kg IM
- Ketamine (10 mg/kg IM) / Xylazine (1 mg/kg IM)
- Ketamine (10 mg/kg IM) / Acepromazine (0.1 mg/kg IM)
4- Steroids mixture SaffanÒ
5- Neuroleptanaesthetic mixtures.
INHALATION ANAESTHESIA
Stages and planes of anaesthesia
|
Reflex response |
Muscular tone |
Pupil response to light |
Pupil size |
Eyeball position |
Cardiovascular function |
Respiration |
Stage of anaesthesia |
|
All present |
Good |
Yes |
Normal |
Central |
Normal |
Normal rate in dog (20-30 breath/min.) |
I) Induction |
|
All present |
Good |
Yes |
May be dilated |
Central may be nystagmus |
HR may increase |
Irregular , may hold breath or hypoventilation |
II) Excitement |
|
Swallowing poor or absent. Other present but diminished |
Good |
Yes |
Normal |
Central or rotated , may be nystagmus |
HR > 90 beat/min |
Regular rate (12-20 breath/min) |
III) Plane 1 Light anaesthesia |
|
Patellar, palpebral , and corneal may be present others are absent |
Relaxed |
Sluggish |
Slightly dilated |
Often rotated ventrally |
HR>90 beat/min |
Regular may be shallow (12-16 breath/min) |
III) Plane 2 Medium surgical anaesthesia |
|
All reflexes diminished or absent |
Greatly reduced |
Very sluggish |
Moderately dilated |
Centrally, may rotate ventrally |
HR is 60-90 beat/min, pulse is less stronger |
Shallow rate < 12 breath/ min |
III) Plane 3 Deep surgical anaesthesia |
|
No reflex activity |
Flaccid |
Unresponsive |
Widely dilated |
Central |
Cardiovascular collapse |
Apnea |
IÑ) Toxic stage |
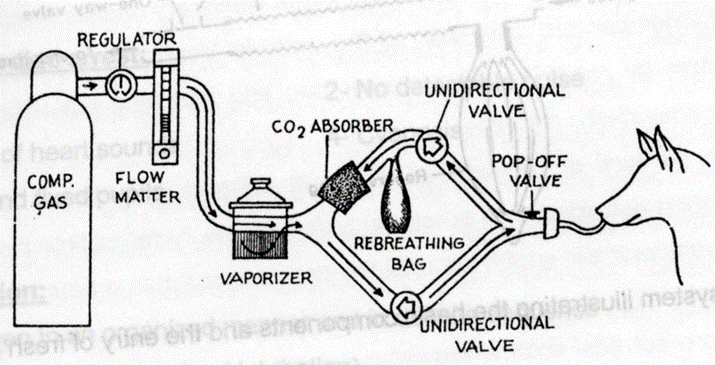
System of Classification of Inhalation Anaesthetic Apparatus
|
Closed |
Semi-closed |
Semi-open |
Open |
System |
|
Circle system |
- Circle system |
- Magill system - Ayre-piece - Norman elbow |
Mask Open drop Anaesthetic box |
|
|
Yes |
Yes |
Yes |
No |
Reservoir bag |
|
Complete |
Partial |
No |
No |
Rebreathing |
|
Yes |
Yes |
No |
No |
Co2-absorber |
|
- Flowmeter - Vaporizer - Reservoir bag Soda lime canister |
- Flowmeter - Vaporizer - Reservoir bag Soda lime canister |
- Flowmeter - Vaporizer - Reservoir bag - O2 cylinder |
- |
Component |
