
- Neonatal Asphyxia
Neonatal asphyxia occurs when oxygen supply to the brain and body tissues is insufficient due to impaired gas exchange in the placenta or lungs during birth. Affected newborns may exhibit:
- Acidosis (pH < 7.45)
- Low Apgar score (<3 at 5 minutes post-birth)
- Seizures
- Multiple organ dysfunction
Severe birth asphyxia can lead to brain damage, cerebral palsy, intellectual disability, or even death. Immediate neonatal resuscitation is crucial to minimize complications.
Causes of Neonatal Asphyxia:
- Maternal Causes During Pregnancy or Labor:
- Placental insufficiency (e.g., placental abruption, abnormal placental position)
- Umbilical cord problems (e.g., cord prolapse, cord compression, nuchal cord)
- Uterine rupture
- Prolonged or difficult labor
- Maternal hypoxia due to heart, lung, or nervous system disorders
- Maternal conditions (thyroid disease, diabetes, preeclampsia, infections)
- Smoking or substance exposure during pregnancy
- Neonatal Causes:
- Prematurity
- Meconium aspiration
- Severe respiratory distress
- Cyanotic congenital heart disease
- Severe anemia (due to hemorrhage or hemolysis)
- Birth trauma
- Neonatal infections and sepsis
Neonatal Asphyxia
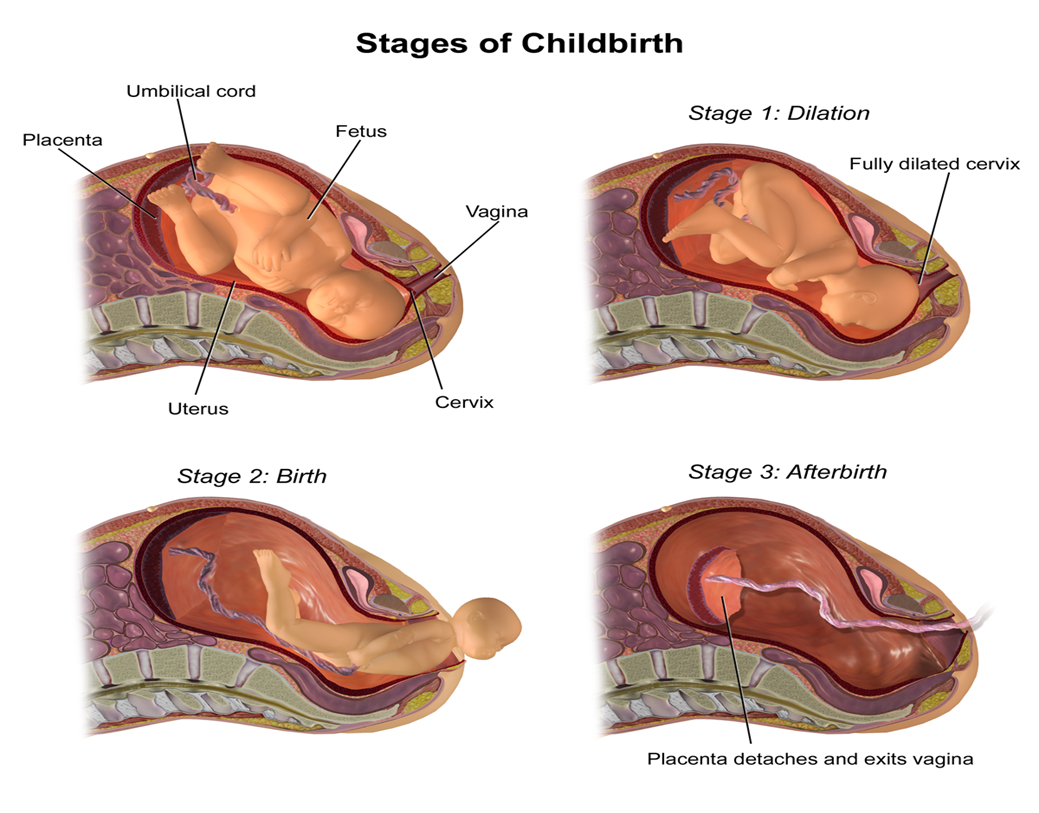
Neonatal asphyxia occurs as a result of prolonged labor, with the first and
second stages exceeding 20 hours in primigravida and more than 14 hours in
multiparous women.
Clinical Manifestations:
There are several indicators during delivery that suggest the possibility of
neonatal asphyxia, such as:
· Meconium-stained amniotic fluid
· Low Apgar score
· Cyanosis or pallor of the body
· Respiratory distress and bradycardia
· Convulsions or generalized muscular hypotonia
Grades of Neonatal Asphyxia:
First Degree – Characterized by:
· Periods of hyperalertness and irritability, with tremors or abnormal movements, either spontaneous or triggered.
· Exaggerated Moro reflex.
· Weak sucking reflex.
· Tachycardia.
· Pupil dilation.
· Absence of seizures at this stage.
· Symptoms typically resolve within 24 hours.
Second Degree – Characterized by:
· Lethargy.
· Weak Moro reflex.
· Weak or absent sucking reflex.
· Bradycardia and hypotension.
· Pupil constriction.
· Seizures occurring in 50–70% of neonates within 24 hours after birth.
Third Degree – Characterized by:
· Coma.
· Severe muscle hypotonia.
· Absence of Moro reflex.
· Loss of sucking reflex.
· Episodes of apnea.
· Persistent bradycardia and hypotension.
· Seizures are uncommon, but if present, they are usually resistant to treatment.
· Mortality rate reaches approximately 50%; survivors often suffer from serious complications.
Investigations and Laboratory Tests:
· Monitoring blood glucose levels.
· Assessing serum calcium, sodium, and magnesium levels.
· Arterial blood gas analysis.
· Complete blood count.
· Cranial ultrasound and computed tomography (CT) scan.
Management:
1. Prevention of Neonatal Asphyxia – the most effective approach, achieved through:
o Providing adequate antenatal care to identify high-risk pregnancies and manage them appropriately during the perinatal period, ensuring maternal and neonatal safety.
o Effective implementation of neonatal resuscitation protocols.
2. Supportive management for the brain and other body systems.
3. Seizure control.
4. Whole-body therapeutic hypothermia to protect the brain and minimize complications of moderate to severe hypoxic-ischemic encephalopathy, achieved by reducing the infant’s core body temperature.
Nursing Care:
· Ensuring airway patency at all times by maintaining proper positioning and performing suctioning when indicated.
· Maintaining the neonate’s body temperature within the normal range.
· Administering oxygen appropriately as prescribed.
· Monitoring blood glucose levels regularly.
· Preparing and administering intravenous fluids as ordered by the physician.
· Recording fluid intake and output, ensuring accurate urine measurement.
· Monitoring for seizure activity and reporting immediately to the physician if it occurs.
· Performing neurological assessments, including level of consciousness, activity, posture, muscle tone, sucking reflex, Moro reflex, heart rate, respiration, and pupillary reaction
