
- Chest Physiotherapy
Objectives:
- Remove accumulated airway secretions
- Increase airway and lung capacity
- Improve respiratory function through better gas exchange
- Prevent endotracheal tube obstruction
- Reduce the risk of respiratory infections
Techniques and Positions for Chest Physiotherapy:
- Postural Drainage: Positioning the neonate to facilitate drainage of secretions from specific lung segments.
- Percussion: Gentle tapping on the chest wall to loosen secretions.
- Vibration: Manual vibration of the chest to mobilize mucus.
- Airway Suctioning: Removal of secretions from the trachea as needed.
These methods are applied according to the neonate’s condition, with continuous monitoring to ensure safety and effectiveness.
|
Technique |
Advantages |
Contraindications / Precautions |
|
Postural Drainage |
- Involves positioning the neonate according to the location of accumulated secretions in the lungs for a set period, using gravity to move secretions toward the center of the chest or carina for suctioning.- Prevents secretion buildup due to immobility or infection spread.- Reduces adhesions in the lungs after extubating from mechanical ventilation. |
- Avoid head-down tilt in cases of: • Preterm infants <1250 g • Intracranial hemorrhage • Untreated hydrocephalus • Immediately after feeding • Birth-related eye hemorrhage • Hypertension- Avoid prone positioning if: • Recent abdominal surgery • Abdominal distension |
|
Percussion |
- Loosens accumulated secretions, moving them from small to large airways for suctioning or cough reflex stimulation.- Gentle tapping on both sides of the chest using a padded mask or soft artificial nipple.- One hand supports the neonate’s head during percussion. |
- Same contraindications as postural drainage- Pneumothorax or emphysema- Bleeding disorders or risk of hemorrhage- Pulmonary hemorrhage- Rib fractures- Skin infections, bruises, or wounds |
|
Vibration |
- Massage over areas of secretion accumulation using the hand or a vibration device to mobilize mucus from small to large airways for suctioning or cough reflex stimulation.- One hand supports the neonate’s head, monitoring tolerance throughout. |
- Same as percussion and postural drainage |
Role of the Nurse in Chest Physiotherapy
1. Assessment and Preparation Before Chest Physiotherapy
The nurse is responsible for evaluating the neonate’s condition and preparing all necessary equipment prior to performing chest physiotherapy:
- Assess the need for chest physiotherapy and select the appropriate technique based on the neonate’s condition.
- Ensure vital signs are stable: temperature, heart rate, respiratory rate, blood pressure, and oxygen saturation.
- Connect the neonate to a monitor.
- Auscultate the chest to identify areas of secretion accumulation.
- Perform a chest X-ray if needed to locate areas of pulmonary secretions.
- Prepare all required equipment depending on the chosen technique, including:
- Padded masks in various sizes suitable for the neonate
- Suction machine
- Vibration device with specifications:
- Battery operated
- Electrically safe
- Smooth surface
- Easy to disinfect between patients
- Suction catheters of different sizes (6, 8, 10 Fr)
- Sterile gloves
- Saline solution
- Sterile dressings
- Small towel
- Oxygen source
- Pulse oximeter or monitor
- Ambu bag
- Stethoscope
2. Steps for Postural Drainage
- Identify the area of secretion accumulation in the lungs and choose the optimal positions to mobilize the secretions.
- Apply postural drainage positions, maintaining the neonate’s posture using a small towel for support, for 10–15 minutes per position or as instructed by the physician.
- Maintain a schedule for changing the neonate’s positions.
- Perform airway suctioning after drainage.
Potential Risks and Complications of Postural Drainage
- Dislodgement of endotracheal tube, umbilical catheter, or chest tube
- Increased intracranial pressure
- Pressure on the diaphragm
- Aspiration of stomach contents into the airway
- Apnea caused by airway obstruction
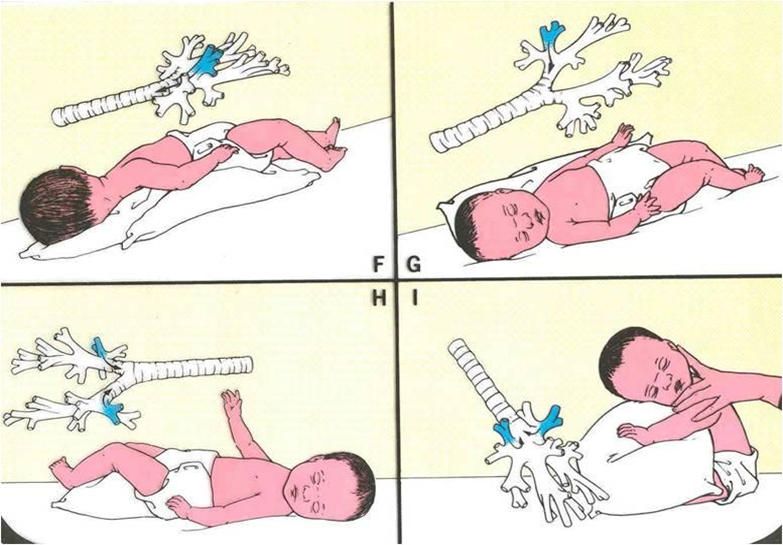
Examples of Chest Physiotherapy Positions
Chest Physiotherapy Techniques: Vibration and Percussion
Vibration Technique (Vibration)
Steps:
- Identify the area of secretion accumulation in the lungs.
- Place the neonate on one side.
- Place a soft barrier (e.g., cloth) between the skin and the vibration device (electric brush).
- Apply the device to the back of the neonate, moving in an upward circular motion from bottom to top.
- Coordinate vibrations with the neonate’s exhalation for effectiveness.
- Duration: 2–3 minutes per area or as prescribed by the physician.
- Perform airway suctioning after the session.
Potential Complications:
- Hypoxemia (low blood oxygen)
- Skin abrasions
Percussion Technique (Percussion / Clapping)
Steps:
- Identify the area of secretion accumulation in the lungs.
- Place the neonate on one side.
- Perform gentle percussion using a padded mask, tapping the affected chest area from bottom to top.
- Duration: 5–10 minutes per area depending on tolerance.
- Perform airway suctioning after percussion.
Notes for Both Techniques:
- Monitor vital signs and oxygen saturation throughout the session.
- Adjust technique according to the neonate’s tolerance and physician instructions.
- Always have suction equipment ready to clear secretions immediately.
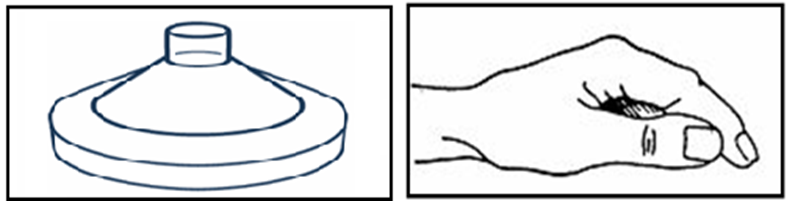
Tools for Performing the Percussion (Clapping) Technique
Potential Complications of the Percussion Technique
- Hypoxemia (low blood oxygen)
- Skin abrasions
- Rib fractures
- Liver or spleen tissue injury
- Pain or discomfort for the neonate
3. Post-Therapy Assessment
After completing chest physiotherapy, the nurse should:
- Check vital signs:
- Temperature, heart rate, respiratory rate, blood pressure, and oxygen saturation to ensure stability.
- Auscultate the chest:
- Listen for improved air entry and reduced crackles or wheezes.
- Palpate the chest:
- Assess for abnormal vibrations or narrowing of airways (tactile fremitus).
- Chest X-ray:
- If necessary, to confirm clearance of pulmonary secretions.
- Evaluate response to therapy:
- Determine if the neonate tolerated the session well and if secretions have been effectively mobilized.
- Document improvements or any complications.
Neonate’s Response to Chest Physiotherapy
|
Positive Response |
Negative Response |
|
Improved respiratory effort |
Signs of fatigue or stress |
|
Improved respiratory rate |
Increased respiratory effort and rate |
|
Improved oxygen saturation |
Decreased oxygen saturation |
|
Improved arterial blood gas results |
Recurrent apnea episodes |
|
Overall improvement in general condition |
Deterioration of general condition |
