
- Regulating Newborn Temperature
The body temperature remains stable when heat loss and heat gain are balanced. If heat loss exceeds heat production, hypothermia occurs, and vice versa. Therefore, maintaining an optimal thermal environment is a key goal for neonatal caregivers to preserve normal body temperature and reduce energy loss.
Neutral Thermal Environment (NTE):
- The ideal environmental conditions that help maintain the newborn’s core body temperature between 36.5°C and 37.5°C with minimal energy loss and oxygen consumption.
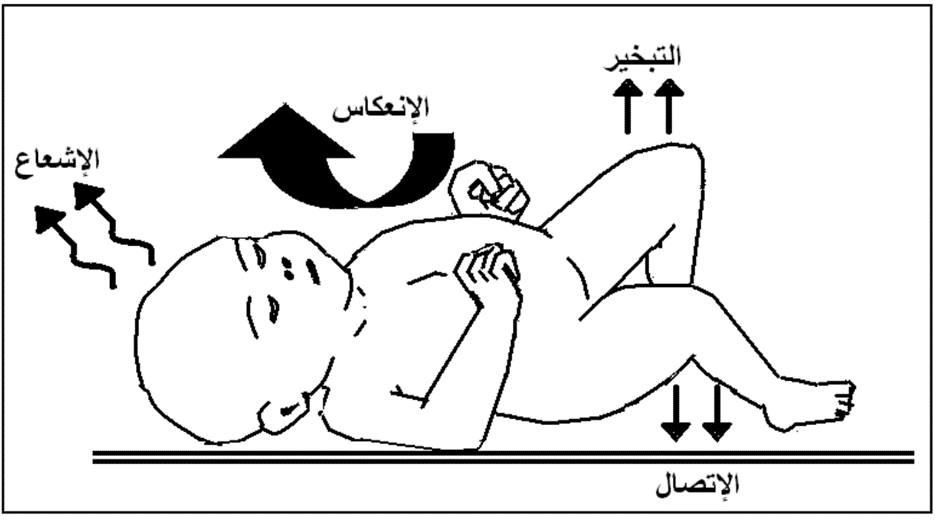
Ways Newborns Lose Heat:
1. Evaporation:
- Occurs when moisture (e.g., amniotic fluid or bath water) evaporates from the newborn's skin.
- Preventive measures:
- Dry the newborn thoroughly with a dry cotton towel immediately after birth and after bathing, especially the head.
2. Conduction:
- Occurs when the newborn's skin comes into direct contact with a cold surface (e.g., metal objects).
- Examples:
- Placing the newborn on a cold mattress or examination table.
- Using a cold weighing scale or X-ray plate without insulation.
- Placing a cold stethoscope on the newborn's skin.
- Preventive measures:
- Ensure insulation (e.g., cloth layers) between the newborn’s skin and any cold surfaces.
3. Convection:
- Occurs when air currents replace the warm air around the newborn with cooler air, leading to heat loss.
- Examples:
- Exposure to cold oxygen from a humidifier.
- Exposure to air currents from air conditioners or fans.
- Preventive measures:
- Keep newborns away from air drafts.
- Use warm water in oxygen humidifiers and change it regularly.
4. Radiation:
- Occurs when the newborn loses heat to a colder solid object nearby without direct contact.
- Example:
- Placing an incubator near a cold wall without maintaining the required 1-meter clearance on all sides.
- Preventive measures:
- Maintain room temperature at 24–26°C in delivery and neonatal units.
- Place incubators centrally in the room and ensure the 1-meter clearance from walls.
Body Temperature Regulation Disorders in Neonates
These disorders manifest either as hypothermia or hyperthermia.
I. Hypothermia
Definition:
A decrease in the infant’s core body temperature below 36.5 °C.
Causes:
- Exposure to a cold external environment due to failure to maintain the delivery room temperature at the appropriate range (24–26 °C).
- Failure to maintain the neonate’s temperature immediately after birth, especially in preterm infants, where body temperature may drop by 1 °C right after birth. Examples include:
- Not placing the neonate under a pre-warmed radiant warmer during immediate postnatal care.
- Delayed drying of the neonate, or leaving wet towels underneath.
- Separation from the mother.
- Giving the neonate a bath immediately after birth, even with warm water.
- Dressing the neonate inadequately or in light clothing.
Infants at higher risk of hypothermia:
- Low birth weight or growth-restricted infants.
- Infants with hypoglycemia.
- Infants with birth asphyxia.
- Infants with neonatal sepsis.
- Infants with congenital heart or gastrointestinal anomalies (e.g., omphalocele, gastroschisis).
- Infants with hemolytic disease due to Rh incompatibility.
- Infants with respiratory distress.
Clinical manifestations of hypothermia:
Early signs:
- Cool skin to touch, especially extremities, with peripheral cyanosis.
- Weak suck or poor feeding ability.
- Signs of respiratory distress (increased respiratory rate) and tachycardia.
- Lethargy and weak crying.
- Skin color changes from pallor and cyanosis to mottling.
Late signs:
- Apneic episodes.
- Bradycardia.
- Hypoglycemia.
- Metabolic acidosis.
- Intracranial or pulmonary hemorrhage.
- Sclerema neonatorum (hardening of subcutaneous fat tissue).
II. Hyperthermia
Definition:
An increase in the infant’s core body temperature above 37.5 °C.
Causes:
- Exposure to excessive environmental heat.
- Overheating due to high incubator temperature.
- Exposure to phototherapy without adjusting incubator settings.
- Severe dehydration.
- Neonatal sepsis.
- Intracranial hemorrhage.
Clinical manifestations of hyperthermia:
- Warm skin to touch, initially flushed then later pale.
- Tachycardia.
- Tachypnea.
- Irritability.
Role of the Nurse in Maintaining Neonatal Temperature
1. In the Delivery Room:
- Prepare a warm environment, free from air drafts, with room temperature maintained at 24–26 °C.
- Preheat the radiant warmer (servo-controlled) 10–20 minutes before delivery.
- Dry the neonate immediately after birth, ensuring no wet towels remain underneath.
- Encourage skin-to-skin contact with the mother whenever possible.
2. In the Neonatal Intensive Care Unit (NICU):
- Upon admission, undress the neonate except for the diaper, and place under the radiant warmer.
- Attach the temperature probe to the right upper abdominal wall.
- Adjust the radiant warmer to 36.5 °C.
- Measure the neonate’s temperature every 30–60 minutes or as prescribed until it stabilizes.
- Monitor temperature every 3–4 hours, and adjust incubator settings according to age and weight (Table 8-1).
- Place incubators away from sunlight or drafts.
- Minimize incubator door openings.
- Monitor temperature closely during phototherapy to prevent overheating.
Table 8-1. Neutral Thermal Environment (Incubator Temperature Settings)
|
Age & Weight |
Incubator Temperature (°C) |
|
|
Initial Temperature (°C) |
Range (°C) |
|
|
0–6 hours <1200 g |
35.0 |
34.4 – 35.0 |
|
1200–1500 g |
34.1 |
33.9 – 34.4 |
|
1501–2500 g |
33.4 |
32.8 – 33.8 |
|
>2500 g |
32.9 |
32.0 – 33.8 |
