
- Formula Feeding
Formula milk should be prepared in bottles in quantities enough for a single feeding or for up to 4 hours if using continuous feeding via gastric tube. Refrigerated formula can be stored for up to 24 hours but should be used within 4 hours after opening.
Preparing and Giving Formula Milk:
Bottle Feeding:
- Use small nipples for premature babies, soft nipples for weak feeders, and regular nipples for strong feeders.
Preparation:
- Follow the doctor’s instructions regarding the formula type, concentration, and quantity.
Required Equipment:
- Bottle sterilizer or a large pot for boiling bottles.
- Bottles with nipples and caps.
- Kettle for boiling water.
- Sterile tray.
- Bottle tongs.
- Bottle brush.
- Liquid soap for washing bottles.
- Infant formula (check expiration date).
- Formula scoop.
- Knife.
- Clean cotton pad.
Steps:
- Wash hands properly.
- Boil the necessary amount of water plus 60ml extra to compensate for evaporation. Boil for one minute to sterilize.
- Let the water cool to room temperature.
- Pour the required amount of warm water into sterilized bottles.
- Add the correct formula amount using a leveled scoop.
- Shake well to mix.
- Test the temperature by dropping a few drops on the inner wrist before feeding.
- Cool the formula if needed by placing the bottle in cold water.
Feeding Steps:
- Wash hands properly.
- Verify baby’s full name and medical number, type of formula, and amount.
- Measure abdominal circumference as instructed.
- Ensure the baby is fully awake.
- Hold the baby as if breastfeeding.
- Place a cotton pad on the baby’s chest.
- Stimulate the baby’s lips with the nipple; once the baby opens its mouth, gently insert the nipple.
- Keep the nipple filled with milk at a 45-degree angle to avoid air intake.
- Maintain eye contact and emotional bonding with the baby.
- Encourage burping mid-feed and after feeding to prevent gas.
- Lay the baby on the right side to prevent choking and reduce stomach pressure.
- Clean the baby’s mouth with sterile saline-soaked gauze to prevent fungal growth.
- Discard any remaining milk—do not reuse.
- Wash hands properly.
- Record the amount of milk consumed, any vomiting, or abnormal signs (e.g., bluish skin) and inform the doctor.
Feeding via Nasogastric Tube:
Required Equipment:
- Sterile feeding tube (size 6 for preemies <1500g, size 8 for larger babies).
- Syringe (10-20ml).
- Clean towel.
- Stethoscope.
- Warm formula per doctor’s instructions.
- Adhesive tape for fixation.
- Sterile water ampoules.
- Bottle nipple with cotton filling.
- Sterile gloves.
- Waste disposal bins (black & red bags, sharps box).
Tube Insertion Steps:
- Wash hands properly.
- Open the sterile feeding tube package.
- Wear sterile gloves.
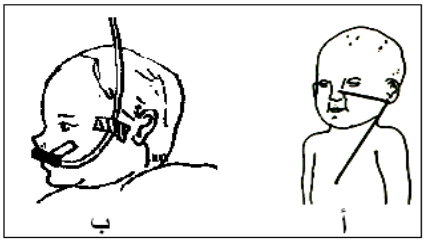
- Measure the tube length from nose/mouth to the earlobe, then from earlobe to the bottom of the sternum, marking with tape.
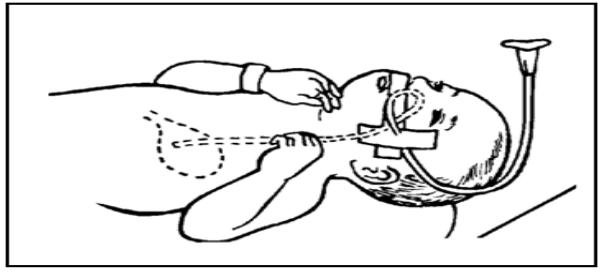
- Insert the tube while positioning the baby’s head at a 30° angle.
- If resistance, choking, or blue discoloration occurs, immediately remove the tube and retry.
- Verify correct placement by injecting 0.5-1ml air and listening for gurgling sounds in the stomach with a stethoscope.
- Secure the tube with adhesive tape.
Continuous Drip Feeding and Intravenous Nutrition
1. Continuous Drip Feeding:
This method is preferred for:
- Newborns with severe gastroesophageal reflux (GERD).
- Low birth weight infants weighing less than 1000g at birth.
Preparation of Feeds:
- Follow the doctor's instructions regarding formula type, concentration, and quantity.
Feeding Procedure:
- Draw the required amount of milk into a syringe.
- Attach the syringe to a syringe pump, then connect it to the feeding tube using a syringe extension.
- Set the pump speed to the required drip rate per hour as per the doctor's instructions.
- Administer the feed using the syringe pump.
- Change milk containers (syringes) and connecting extensions every 4 hours to prevent milk exposure to room temperature for too long.
