
- PROTOZOAL DISEASES
1- Coccidiosis
General: Coccidiosis is a common,
widespread problem in commercial operations
and
research facilities. It is an important economic and complicating disease.
Coccidia may act as a co-pathogen in other infections. As with the other causes
of enteritis, changes in management practices such as feeding or experimental
procedures can predispose to infection and disease.
There are two forms of coccidiosis in rabbits - an intestinal form, and a hepatic form. Eimeria species commonly cause enteric disease in large groups of rabbits, especially in young animals.
Disease Forms/Subtypes
Hepatic
caused by:
Eimeria stiedae.
-Subclinical
disease is common.
-Acute mortality is associated with large infective oocyst dose.
-When clinical disease is present, the signs are variable.
Intestinal form (Intestinal Coccidiosis)
- Subclinical disease is common in adult rabbits. Pathogenicity varies with Species of Eimeria. All intestinal species of Eimeria appear to be pathogenic in young rabbits.
- In adult rabbits, E. coecicola, E. irresidua, and E. magna are highly pathogenic; E. piriformis and E. media are moderately pathogenic; and E. perforans is mildly pathogenic.
Although rabbits are cecotrophic, it is generally accepted that cecotropes do not contain infectious oocyst.
Transmission:
Fecal-oral.
After passage in the feces, the oocysts require one or more days to sporulate.
Pathogenesis:
-After
the sporulated oocysts are ingested, sporozoites are released which invade
enterocytes
and multiply via schizogony.
- One or more sexual cycles
(depending on the species) takes place, then gametogony occurs and oocysts are
formed and passed in the feces.
-
Most Eimeria species in rabbits affect one or more segments of small
intestine;
a few affect cecum or colon also.
- Parasitized enterocytes are lost
resulting in superficially necrotizing enteritis. Severity of epithelial
destruction and degree of inflammatory response vary considerably.
Clinical signs
Intestinal Coccidiosis
Varies from none to profuse watery, even bloody, diarrhea and death, depending
on susceptibility of host (young or
not previously exposed are more susceptible),
species
of causative organism, and inoculating dose. Mild or no signs are more
common.
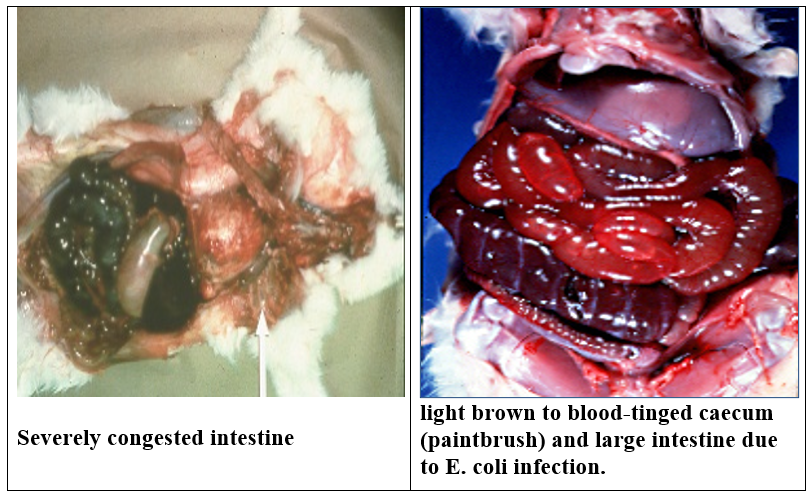
The cecum and colon contain dark green to brown, watery, foul smelling
material. The mucosa is congested and edematous.
Pathology: Location of the lesions is
dependent on the species involved. Destruction of
enterocytes,
villous atrophy, marked heterophilic infiltration and presence of gametocytes
and oocytes.
Hepatic coccidiosis
Etiology: Eimeria stiedae.
-Infected
rabbits showed poor weight gains, clinical disease and even death in affected
colonies.
-Weanlings are most often affected; older rabbits develop immunity.
-The liver is enlarged owing to papillary hyperplasia of the bile duct epithelium (and gallbladder occasionally) with different developmental stages of coccidia within bile ducts.
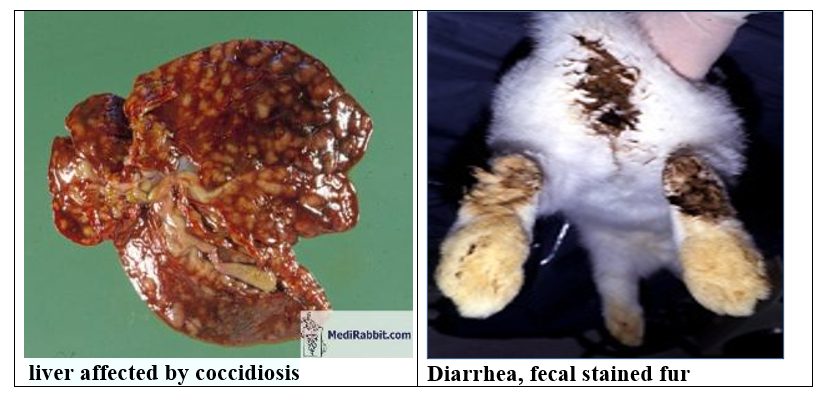
-Acute cases may show numerous miliary hepatic abscesses.
-Chronic cases develop a fibrotic response around affected ducts.
-Other organs are not infected.
Life-cycle of Eimeria stiedae.
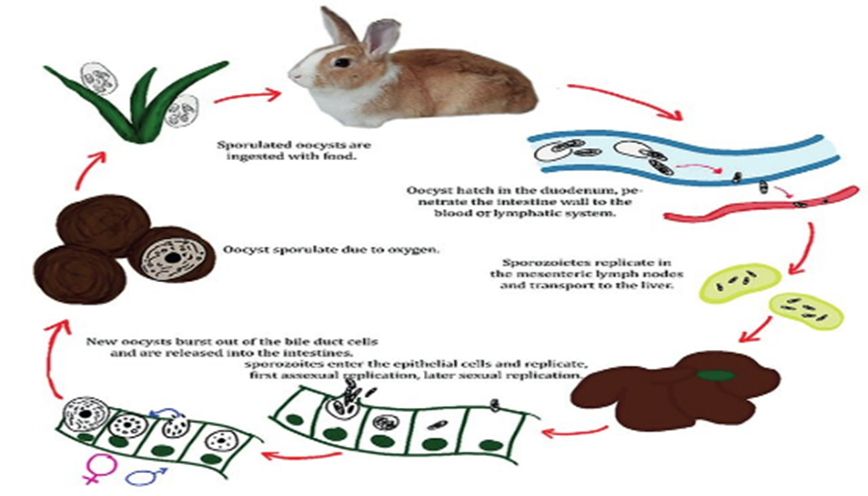
Transmission:
After
ingestion of sporulated oocysts, sporozoites penetrate intestinal epithelial
cells then are transported to the liver where they invade epithelial cells
lining bile ducts and undergo schizogony. After gametogony, oocysts are
released into bile ducts, pass to the intestinal tract via the bile and are
then passed into the feces.
Clinical
signs:
-
None to anorexia, debilitation, constipation or diarrhea. May also see
hepatomegaly, pendulous abdomen, icterus and death. Elevated liver enzymes and serum bilirubin on clinical
pathology.
-
Hepatomegaly with multifocal, raised, yellow to pearl grey, circumscribed,
0.5-2 um foci which contain an inspissated dark green to tan material. In the
liver; these are bile ducts chronically inflamed and dilated with bile and
exudate.
- Microscopic:
chronic proliferative cholangitis and cholecystitis, with numerous schizonts,
microgametes, macrogametes, and developing oocysts in the epithelial cells;
also, oocysts in the lumen.
D.D:
Enteric
Diseases: (enterotoxemia, Tyzzer’s disease, coccidiosis, and mucoid
enteropathy, E.coli , salmonella)
