
- Skin problems
1-Rabbit Syphilis
Spirochetosis, Treponematosis
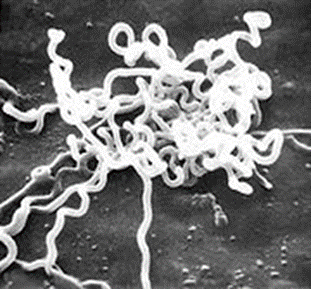
Etiology:
Treponema
cuniculi. Characteristic Gram-negative, 5-20 um, helical rods with tight or
irregular spirals
General: The disease is also referred to as
rabbit syphilis and vent disease and
is
common
in wild hares. This disease occurs occasionally in conventional facilities and
asymptomatic rabbits may be serologically positive.
Transmission: Zoonotic disease (from human to
rabbit not from rabbit to human)
Venereal,
although transmission through extragenital contact can occur. The organism can
penetrate intact mucous membranes. Susceptibility is age and breed dependent.
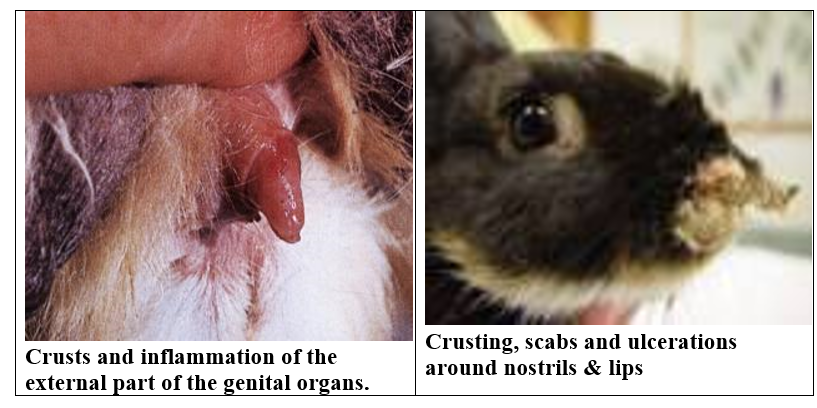
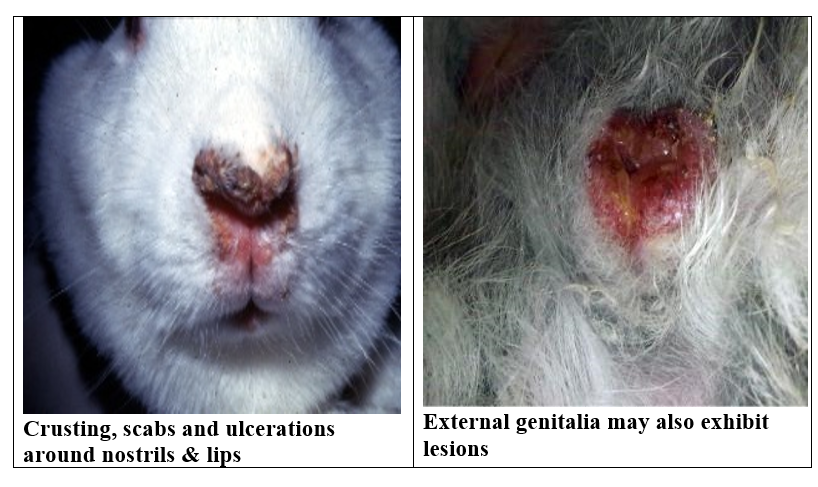
Clinical signs:
Edema
and erythema at the mucocutaneous junctions of the vulva, prepuce, anal region,
muzzle and periorbital area. Lesions are often crusty. Popliteal and inguinal
lymph nodes may be enlarged. Desire for mating is lost.
P.M:
Lesion
is confined to the epithelium and superficial dermis.
Epidermal
hyperplasia, epidermal cell necrosis, erosions and ulceration and infiltration
by predominantly plasma cells and lymphocytes with fewer heterophils.
Diagnosis:
-Scrapings
with wet mount preparation and examination under dark-field microscopy or in
silver-stained tissue sections.
-Serological
( Reagin antibody and fluorescent treponemal antigen test) .
Differential diagnosis:
Pasteurella sp. infections of the
external genitalia and lesions due to trauma, Listeriosis, Fleas,
Pseudotuberculosis(yersiniosis)
Treatment:
Penicillin
40,000 IU/kg q7days for rabbit (syphilis) may lead to diarrhea., so
tetracycline or arsenic preparation injected.
2-Ectoparasites (Mange)
Mange (“ear canker.”)
A non-burrowing fur mite that is
non-pathogenic even in heavy infestations The life cycle is about 5 weeks.. It
is not zoonotic.
Psoroptes cuniculi Rabbit ear mite.
-Non-burrowing mite that causes intense irritation – head shaking, scratching of the ears, hyperaemia - and the production of exudate leading to thick crust formation filling the auditory canal. Mites irritate the lining of the ear and cause serum and thick brown crusts to accumulate, creating an “ear canker.”
Lesions can spread to the face and neck, the ear drum can perforate leading to a purulent otitis media (secondary bacterial infection) and meningitis, reach the CNS, and result in torticollis.

N.B:
-The brown crumbly exudate should never be removed in a conscious rabbit, because this is very painful.
- The crusts will slowly slough off as the mites die and the tissue underneath heals. -The incidence is much lower when rabbits are housed in wire cages instead of solid cages.
Transmission:
The mite is readily transmitted by direct contact.
Diagnosis:
-Mites can be visualized on otoscopic examination.
- Microscopic examination of aural debris.
Diagnosis
- The examined areas of the body are ears, head, neck, thorax, abdomen, and extremities.
In ear mange, the lesion score is as follows:
0 for apparently normal ears
1 for lesions inside the ear
2 for lesions on the bottom third of the ear
3 for lesions extending to the two thirds of the ea
and 4 for lesions with a greater extension than two thirds of the ear.
- Serological tests such as enzyme-linked immunosorbent assay are used to detect the antibodies against Sarcoptic scabiei
Different strategies to control mange in rabbits
Control of rabbit mange:
-Hygienic measures
-Using acaricides:
A) Systemic ( organophosphorous compounds, synthetic pyrethroids).
b) local (Mcrolactones, benzyl- benzoatessulpher- based compounds).
-Using vitamin (A,D and E)
Treatment:
-Should be aggressive with supportive therapy given for
toxic shock, and ivermectin will kill any larvae that emerge from unremoved
eggs.
- Bath with chlorhexidine or a povidene-iodine cleanser.
Give fliuds s/c or, i.v. or i.p. plus ivermectin i.m. 200mcg/kg to kill those maggots out of reach.
- Injectable ivermectin treatment regimens effective against both fur and ear mites have been reported, with the dosage of ivermectin 200–400 mcg/kg, SC, two or three treatments 10–21 days apart.
-Mites may also be treated with selamectin (20 mg topically every 7 days has been effective).
