
- Annexes
Table 1 Quality of Evidence in GRADE
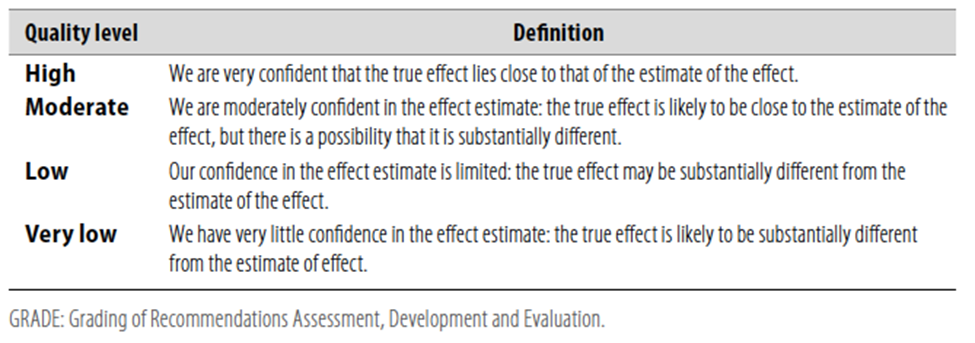
Table 2 Significance of the four levels of evidence
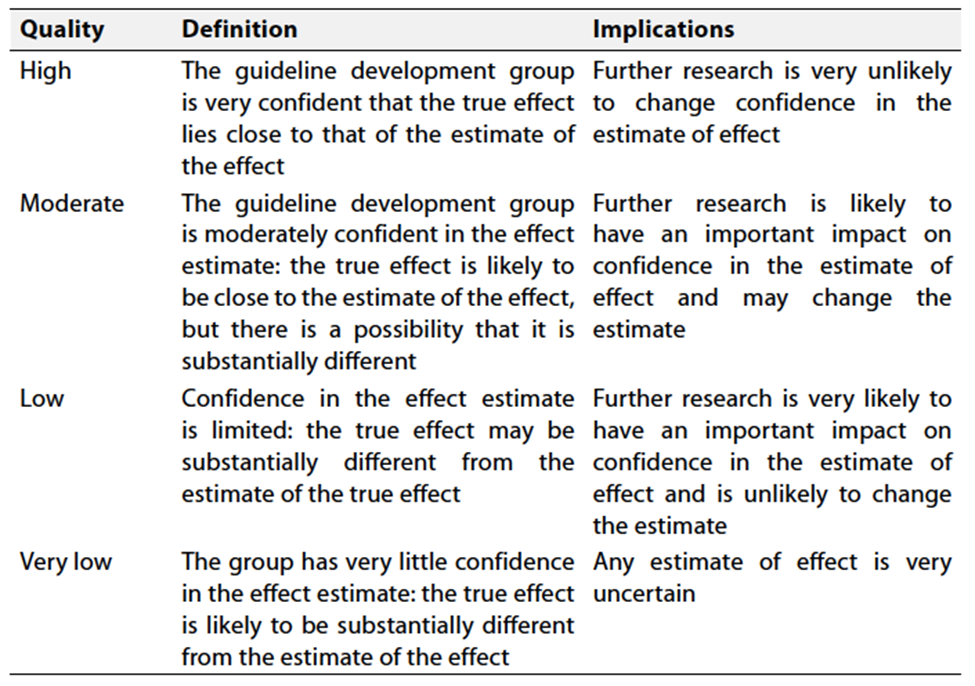
Table 3 Factors that determine How to upgrade or
downgrade the quality of evidence
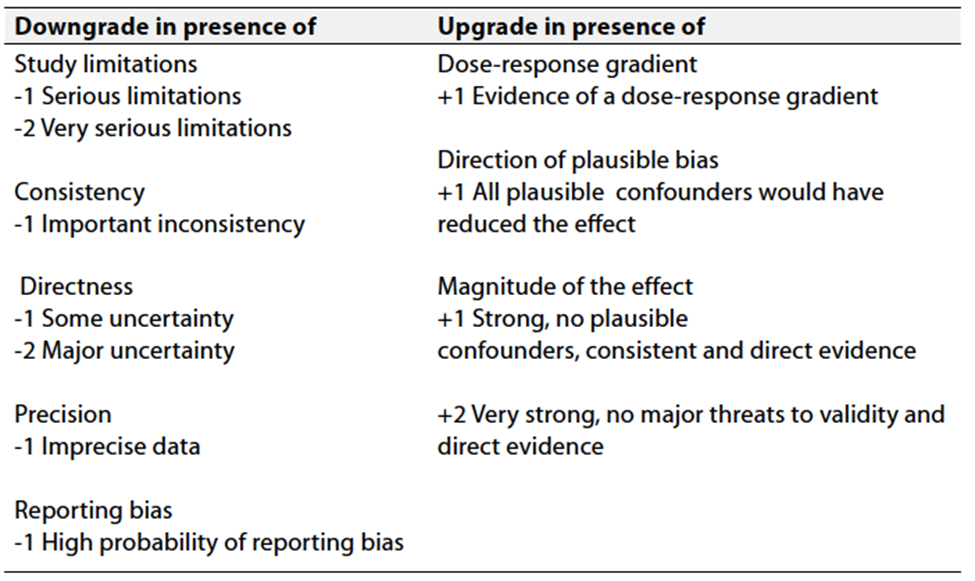
Table 4 Relevant history from a woman suspected to be suffering from OHSS adopted from Green-top Guideline No. 5, February 2016 – The Management of Ovarian Hyperstimulation Syndrome.
|
History |
|
Time of onset of symptoms relative to trigger Medication used for trigger (hCG or GnRH agonist) Number of follicles on final monitoring scan Number of eggs collected Were embryos replaced and how many? Polycystic ovary syndrome diagnosis? |
|
Symptoms |
|
Abdominal bloating Abdominal discomfort/pain, need for analgesia Nausea and vomiting Breathlessness, inability to lie flat or talk in full sentences Reduced urine output Leg swelling Vulval swelling Associated comorbidities such as thrombosis |
Table 5. Proposed RCOG classification of severity of OHSS adopted from Green-top Guideline No. 5, February 2016 - The Management of Ovarian Hyperstimulation Syndrome,
|
Category Features |
|
Mild OHSS Abdominal bloating Mild abdominal pain Ovarian size usually < 8 cma
|
|
Moderate OHSS Moderate abdominal pain Nausea ± vomiting Ultrasound evidence of ascites Ovarian size usually 8–12 cma |
|
Severe OHSS Clinical ascites (± hydrothorax) Oliguria (< 300 ml/day or < 30 ml/hour) Haematocrit > 0.45 Hyponatraemia (sodium < 135 mmol/l) Hypo-osmolality (osmolality < 282 mOsm/kg) Hyperkalaemia (potassium > 5 mmol/l) Hypoproteinaemia (serum albumin < 35 g/l) Ovarian size usually > 12 cma |
|
Critical OHSS Tense ascites/large hydrothorax Haematocrit > 0.55 White cell count > 25 000/ml Oliguria/anuria Thromboembolism Acute respiratory distress syndrome |
|
|
Ovarian size may not correlate with the severity of OHSS in cases of assisted reproduction because of the effect of follicular aspiration. Women demonstrating any feature of severe or critical OHSS should be classified in that category.
Table 6. Examination and investigation of women with suspected OHSS adopted from Green-top Guideline No. 5, February 2016 - The Management of Ovarian Hyperstimulation Syndrome,
|
Examination |
|
General: assess for dehydration, oedema (pedal, vulval and sacral); record heart rate, respiratory rate, blood pressure, body weight Abdominal: assess for ascites, palpable mass, peritonism; measure girth Respiratory: assess for pleural effusion, pneumonia, pulmonary oedema |
|
Investigations |
|
Full blood count Haematocrit (haemoconcentration) C-reactive protein (severity) Urea and electrolytes (hyponatraemia and hyperkalaemia) Serum osmolality (hypo-osmolality) Liver function tests (elevated enzymes and reduced albumin) Coagulation profile (elevated fibrinogen and reduced antithrombin) hCG (to determine outcome of treatment cycle) if appropriate Ultrasound scan: ovarian size, pelvic and abdominal free fluid. Consider ovarian Doppler if torsion suspected |
|
Other tests that may be indicated |
|
Arterial blood gases D-dimers Electrocardiogram (ECG)/echocardiogram Chest X-ray Computerised tomography pulmonary angiogram (CTPA) or ventilation/perfusion (V/Q) scan |
