
- Recommendations
1- Patient evaluation before CTA
1.1 The clinician properly evaluates the patient before requesting CTA guided by the patient's history, clinical presentation, ECG, and initial biomarker assessment. Clinically appropriate patients should have reasonable clinical pre-test likelihood of ACS and exclude alternative non-coronary diagnoses as shown in (Fig.1).
Good Practice Statement (5.6)
1.2 The clinician should acquire ECG and review it for STEMI and Cardiac troponin should be measured as soon as possible.
Good Practice Statement (5.6)
1.3 The clinician should categorize patients into low-, intermediate- and high-risk according to the risk stratification tools. The clinician should indicate the appropriate criteria for performing CCTA.
Good Practice Statement (5.6)
2. Non-contrast Coronary Calcium Scoring (Coronary Agatston Scoring)
2.1 The clinician may request non-contrast coronary calcium scoring for asymptomatic individuals and intermediate-risk individuals (Framingham Risk Score 10% to 20 to document atherosclerotic cardiovascular disease risk stratification and guide preventive measures in
Conditional recommendation
High-Quality Evidence (7,8).
2.2 The clinician should not request non-contrast coronary calcium scoring for high-risk individuals, patients already receiving statin treatment or asymptomatic low-risk adults
Strong recommendation
High-quality evidence (7,8).
2.3 The radiologist should report and categorize patients as no CAC (Agatston score 0), mild (1-100), moderate (101-400), or severe (>400).
Strong recommendation
High-quality evidence (7,8).
3. Coronary CT of the Native Coronary Arteries
3.1 Clinicians should
request CTA as the first line test for evaluating patients with or without
history of CAD who present with stable typical or
atypical chest pain, or other symptoms that are thought to represent a possible
angina equivalent (e.g., dyspnea on exertion, jaw pain).
3.2 Clinicians should request CTA following a non-conclusive functional test, to obtain more precision regarding diagnosis and prognosis if such information will influence subsequent patient management.
3.3 Clinicians should request CTA for patients at higher pretest risk for ACS, including patients with non-ST elevation myocardial infarction (NSTEMI) when the invasive strategy is not preferred (e.g., bleeding risk, vascular access issues, patient preference).
3.4 Clinician should not recommend CTA for low-risk patients or patients with high probability (cardiac catheterization is recommended).
Strong recommendation
High-quality evidence (9,10)
4. Coronary CTA for Coronary Artery Stents
4.1 Clinicians should request CTA for the assessment of coronary stents in symptomatic patients with coronary stents >3mm, with current generation drug-eluting stents that have struts <3mm, and with current generation drug-eluting stents that have struts <100µm
Strong recommendation
High-quality evidence (11).
4.2 Clinicians should not request CTA for the assessment of stents with smaller diameters (<3mm) as they are more challenging to assess, yet CTA may still be a reasonable test for assessing proximal, non-bifurcation thin strut stents that are <3mm.
Conditional recommendation
High-quality evidence (11).
5. Coronary CT for Coronary Artery Bypass Grafts
5.1 Clinicians should request CCTA for the assessment patency of coronary artery bypass grafts in symptomatic patients. CTA offers a non-invasive and reliable method to assess the patency of coronary artery bypass grafts, including both arterial and venous grafts.
Strong recommendation
High-quality evidence (12).
5.2 Clinicians should request CCTA for assessment of graft patency, anastomotic sites, and stenosis, in presurgical planning of redo bypass graft.
Strong recommendation
High-quality evidence (12)
5.3 Clinicians should request CCTA for assessment of coronary grafts and not for assessment of the native coronary arteries in patients with prior CABG as it is of limited value due to severe calcification of the native coronary artery.
Strong recommendation
High-quality evidence (12)
6. Computed Tomography-Fractional Flow Reserve (CT-FFR)
6.1 Clinicians may request CT-FFR for evaluation of lesion-specific physiology from a coronary CTA dataset using computational flow dynamic modeling and some hemodynamic assumptions, increasing the specificity of CCTA (if available).
CT-FFR estimates the pressure drop across a stenosis providing a ratio indicative of lesion-specific ischemia. It reduces the proportion of patients referred to ICA with anatomical stenoses on CCTA that are not hemodynamically significant. CT-FFR is not widely available as it requires high-quality computational resources, leading to off-site analyses, increased cost of testing, and consequently time delays.
Conditional Recommendation
High-quality evidence (13,14)
7. CCT-Extracellular Volume Fraction (CCT-ECV)
7.1 Clinicians may request CCTA for measuring extracellular volume fraction (ECV), which is an important imaging parameter to estimate the expansion of the myocardial extracellular space secondary to myocardial fibrosis. Yet, the gold standard for measuring ECV is Cardiac MRI.CT-based ECV measurements involve the acquisition of pre- and post-contrast images (or post-contrast images and virtual unenhanced images if acquired using dual-energy CT), allowing for the calculation of hematocrit-corrected ECV.
Conditional Recommendation
Moderate-quality evidence (15,16)
8. CCTA Myocardial Perfusion and Viability
8.1 Clinicians may request CCTA for estimation of myocardial perfusion and viability as an alternative modality to Cardiac MR in patients with MRI contraindications.
Myocardial computed tomography perfusion (CTP), to evaluate the presence and extent of myocardial ischemia by visualizing myocardial distribution of iodinated contrast material at rest and after pharmacologically induced stress
There are many associated challenges of myocardial CTP, including the need for pharmacological stress agents and additional radiation exposure, making careful patient selection critical. Cardiac MR is the gold standard for assessing myocardial perfusion and viability
Conditional recommendation
Moderate-quality evidence: (15, 17)
9. Patient Education
9.1- The clinician should inform the patient about the nature of the examination, its objectives, possible risks including radiation dose, their required cooperation, and the sensations they are likely to feel. This is a critical component of shared decision-making. Patients should be given a chance to request an alternative diagnostic strategy if they feel unable or unwilling to proceed.
9.2- The radiologist should repeat the educational process after premedication, just before scanning, to ensure patients remember instructions on breath-holding and are prepared for the sensations likely to occur from nitroglycerin and contrast administration.
Good Practice Statement (5.6)
10- CT Scanner Requirements
10.1 The radiologist/radiographer should obtain CTA according to the minimum CT scanner specifications which meet or exceed criteria outlined by the American College of Radiology, North American Society for Cardiovascular Imaging, and the Society for Pediatric Radiology practice parameters as listed below:
· 64-detector row or greater or dual-source scanners
· Axial resolution ≤0.5×0.5mm
· Z-axis resolution ≤1mm
· Temporal resolution ≤250ms
Strong recommendation
High-quality evidence (18,19).
11. Coronary CTA Acquisition Protocol
11.1 The radiologist/radiographer should obtain Prospective
ECG-triggering CCTA (the most commonly protocol) when the heart rate is regular
and low (< 65 BPM) .
The data acquisition in best diastole phase when there is less motion to
minimize cardiac motion blurring.
Strong recommendation;
High-quality evidence (18, 20).
11.2 The radiologist/radiographer should obtain Retrospective ECG gating is for coronary artery evaluation when the heart rate is high and in cases of arrhythmia
Strong recommendation;
High-quality evidence (18,20).
11.3 The radiologist/radiographer may obtain Retrospective ECG gating is for ventricular functional assessment when other modalities are not available.
Conditional recommendation;
High-quality evidence (18,20)
12. Radiation Safety
12.1 The radiologist is responsible for safety considerations of coronary CTA related to radiation exposure using the principle of As Low As Reasonably Achievable (ALARA). The radiologist/radiographer should perform CCTA with the minimum accepted radiation dose (approximately 3 mSv), by applying the radiation protection measures:
- ECG-based tube current modulation, whereby the mAs is reduced to 20% or 40% during part of the cardiac cycle, typically systole.
- A high-pitch helical scan (pitch of 3.2-3.4) is available on dual-source CT scanners that enable imaging of the entire heart during a single beat, which reduces radiation exposure.
- Reducing the tube potential from 120 to 100 kVp, it is possible to reduce the radiation dose while improving vascular enhancement. N.B., The ability to reduce kVp is often guided by the patient’s weight. Larger patients require a higher kVp for optimal image quality.
- Noise reduction methods such as iterative reconstruction were introduced as an effective radiation dose reduction strategy.
- Suitable Z-axis coverage should be limited to the minimum clinically required. For coronary imaging, scanning from the carina to just beyond the bottom of the heart is generally sufficient. If there is a history of coronary artery bypass surgery, the coverage should begin at the lung apices to include the entire course of internal mammary grafts
Strong recommendation
High-quality evidence (21,22).
13- Contrast Medium Administration
13.1 The radiologist is responsible for safety considerations of coronary CTA related to allergic reactions to iodinated contrast agents, and contrast-induced nephropathy. The radiologist/radiographer should perform CCTA after administration of intravenous iodinated water-soluble contrast media to ensure optimal vascular enhancement between 250 and 300HU in the ascending aorta by applying the following measures.
- The concentration of the contrast medial used should be 300-350 mg Iodine/ml
- In adult patients, the injection rate should be from 5 to 7mL/s using an 18G size needle recommended in an antecubital vein, preferably on the right
- The timing of contrast administration should be determined by using a test injection or bolus tracking technique
- Both dual injectors, biphasic (contrast followed by saline) and triphasic (contrast followed by mix of diluted contrast and then saline) protocols are used
- Check the renal function tests. If the eGFR value is greater than 30 the patient can receive IV iodinated contrast. If eGFR is less than or equal to 30 the case will need approval by the radiologist before IV contrast is used to minimize the risk of contrast-related AKI.
Strong recommendation
High-quality evidence (23,24).
13.2 The radiologist should ensure the presence of patient safety equipment including:
- Advanced cardiovascular life support (ACLS) equipment in the patient preparation and scanner areas.
- Properly trained ACLS-certified nurses or similar qualified staff should supervise the premedication of patients as administration of beta blockers and nitrates.
- A rapid response team and/or an ACLS-certified physician should be readily available for prompt response to urgent or emergent complications.
· Strong recommendation
· High-quality evidence (23,24).
14 - Patient Pre-medication
14.1 Beta-blocker
14.1.1 The radiologist should perform CCTA after preparing the patient by Beta-blocker (metoprolol) to control the heart rate for maximum image quality during low and regular heart rates.
-
Oral Beta-blocker : 50-100mg oral metoprolol given at
least 1h prior to CCTA; some suggest giving 24 h prior to CCTA for more
effective heart rate reduction
-
Intravenous Beta-blocker : 5mg intravenous metoprolol given
with repeated checks of blood pressure and heart rate up to a maximum of 25mg.
14.1.2 The radiologist should be familiar with the common contra-indications for beta-blockers such as heart block, hypotension, systolic dysfunction, poorly controlled asthma, severe aortic valve stenosis, severe bradycardia.
Strong recommendation
High-quality evidence (25.26).
14.2- Nitroglycerin
14.2.1 The radiologist may perform CCTA after preparing the patient by giving oral
(sublingual) nitroglycerin :
0.4-0.8mg (1-2 tablets), 5min prior to CCTA as the coronary vasodilatation usually
lasts for 20-30min
14.2.2 The radiologist should be familiar with the common contraindications for nitroglycerin which is erectile dysfunction medication (sildenafil, tadalafil, etc.) taken within the last 24-48 hr., increased intracranial pressure, right-sided myocardial infarction, severe anemia, known allergies or hypersensitivity
Conditional recommendations
Moderate-quality evidence (27).
15. Post-Processing Methods
15.1 The radiologist should process the axial source image in a dedicated workstation and get more advanced post-processing techniques to assess cardiac anatomy. These include multiplanar reformats, curved multiplanar reformats, volume-rendered three-dimensional images, and cinematic rendering. If functional information is obtained, then segmentation of the ventricular cavities can be used to quantify ventricular volumes and systolic function
Good Practice Statement (28).
16. Reporting Standard
16.1 The interpreting radiologist must be a physician adequately trained in cardiac CT as defined in recent training guidelines issued by the Society of Cardiovascular CT.
The interpreting radiologist should be promptly available in place or by phone for consultation about patient preparation and scan protocol.
Good Practice Statement (29)
16.2- The Written Conventional Report:
The written comprehensive report should contain the relevant imaging findings, their interpretation, an overall summary/conclusion, and recommendations for further management. A sample report is included in table 3.
Table 3. Sample structured report for coronary CTA. The structure may require modification depending on coronary anatomy, the presence of bypass grafts, etc. The CAD-RADS score may be included but should not replace the conclusion
|
CTA CORONARY REPORT |
||
|
INDICATION: |
|
|
|
COMPARISON: |
|
|
|
TECHNIQUE: |
Coronary CTA performed with [ECG gating, or prospective ECG triggering].
|
|
|
MEDICATION: |
|
|
|
QUALITY: |
|
|
|
CORONARY FINDINGS: |
Coronary origins: |
|
|
|
Coronary Dominance: |
|
|
|
Left main: |
|
|
|
Left anterior descending and branches: |
|
|
|
Left circumflex and branches: |
|
|
|
Right coronary and branches: |
|
|
INCIDENTAL FINDINGS:
|
|
|
|
CONCLUSION:
|
[Summary including most severe stenosis, the extent of plaque, recommendations, and significant incidental findings if any]. |
|
Good Practice Statement (30,31).
16.3 The Coronary Artery Disease-Reporting and Data System (CAD-RADS 2.0).
Recently (CAD-RADS 2.0 was created to standardize reporting and interpretation (table 4). It includes management recommendations based on the most severe coronary plaque stenosis and the overall burden of coronary atherosclerosis. The CAD-RADS provides a structured framework to interpret and report CTA findings and aims to improve communication between cardiac imagers and referring physicians, standardize reporting practices, provide a framework for patient management decisions, and facilitate research in CAD.
Table 4. CAD-RADS Reporting and Data System for Patients Presenting With Acute Coronary Chest Pain
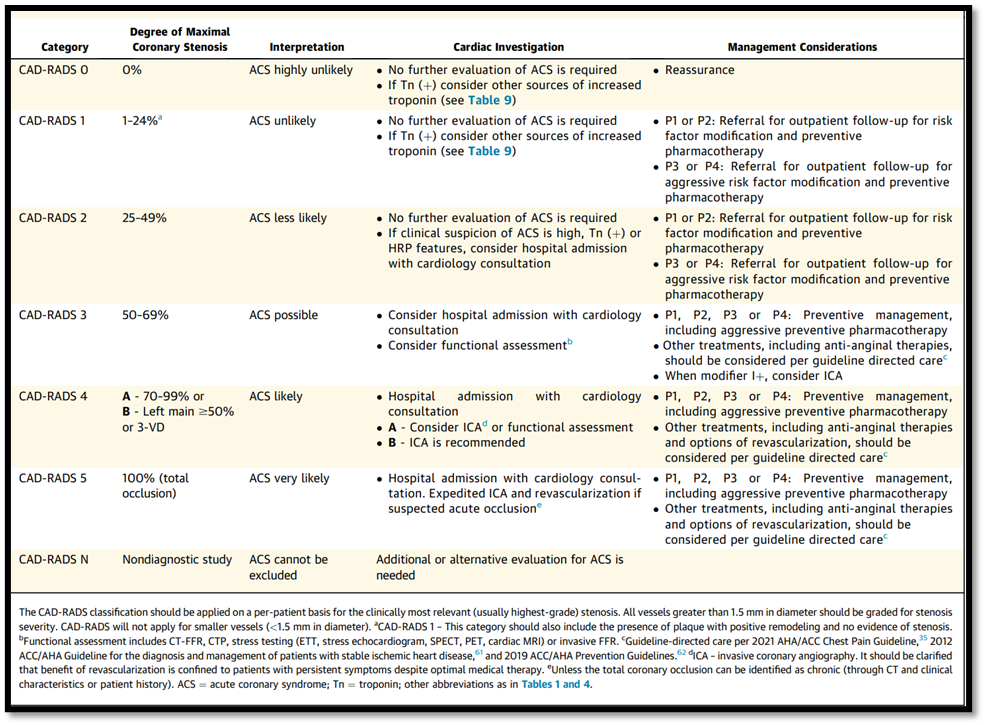
Good Practice Statement (32,33).
